Radiation safety in health care
The World Health Organization (WHO) is working to enhance quality and safety in paediatric imaging under the framework of the WHO Global Initiative on Radiation Safety in Health Care Settings, building upon the ten priorities for improving radiation protection in medicine identified in the Bonn Call for Action [2]:
-
Enhance the implementation of the principle of justification
-
Enhance the implementation of the principle of optimization
-
Strengthen manufacturers’ role in contributing to the overall safety regime
-
Strengthen radiation protection education and training of health professionals
-
Shape and promote a strategic research agenda for radiation protection in medicine
-
Increase global information on radiation exposures in medicine
-
Improve prevention of medical radiation incidents and accidents
-
Strengthen radiation safety culture in health care
-
Foster an improved radiation benefit-risk-dialogue
-
Strengthen the implementation of safety requirements globally
The promotion of radiation safety in paediatric imaging has been a priority of this initiative, including activities in the field of risk assessment, management and communication [3].
Current trends in the use of paediatric imaging
Advances in health technologies have led to an ever-increasing number of clinical applications of radiation in paediatric health care. Ionizing radiation imaging modalities include the use of X-rays in paediatric radiography, fluoroscopy and computed tomography. Digital radiography is replacing conventional film-based radiography in children, providing images that are instantly available for analysis and electronic distribution, with lower costs and facilitated access. Fluoroscopy-guided interventional procedures can replace surgical options which carry a relatively higher risk of adverse events in children. Computed tomography (CT) is a valuable tool for assessing paediatric illness and injury, often replacing less accurate or more invasive diagnostic procedures. Cone-beam CT is increasingly used in children by dentists and orthodontists in some regions to obtain 3D views of the face and teeth, delivering substantially higher doses compared to other dental X-ray exams.
The use of ionizing radiation imaging also includes gamma-rays for diagnostic nuclear medicine in children. Through the injection, inhalation or ingestion of a radioactive tracer, nuclear medicine examinations allow both structural and functional evaluations. Single Photon Emission Computed Tomography (SPECT) and Positron Emission Tomography (PET) scans are the two most common imaging modalities in paediatric nuclear medicine.
Paediatric imaging is also performed by using non-ionizing radiation such as ultrasonic waves (i.e. ultrasonography/ US) and magnetic fields (i.e. magnetic resonance imaging/ MRI). Hybrid imaging is the fusion of complementary imaging modalities (e.g. PET/CT, SPECT/CT, PET/MRI and others), thus improving diagnostic accuracy. This enables identification of images that are not visible by applying other modalities: while PET highlights areas of abnormal metabolism, CT or MRI can accurately localize those areas in the child’s body within various organ and tissues. Advanced imaging techniques can also provide information about prognosis, help assessing therapeutic response and support long-term follow-up.
Considerable disparities exist in the access to paediatric radiology services: while many low- and middle-income countries lack adequate capacity and resources, high income countries are facing issues related with overuse and misuse. Inappropriate or unskilled use of these technologies may cause unnecessary radiation exposures and preventable risks. Radiation risks should be controlled while maximizing the benefits of radiology in children’s care.
Challenges for radiation protection in paediatric health care
Paediatric imaging can save lives and prevent the need for more invasive procedures. The impressive growth of its use during the last two decades was not accompanied by a similar increase in the level of awareness of health professionals about the radiation doses and associated risks. There is a need for raising awareness and building capacity around this issue. A balanced approach is needed that recognizes the multiple health benefits that can be obtained, while assuring that risks are minimized particularly with regards to childhood exposure to ionizing radiation.
While the radiation dose delivered during diagnostic procedures is usually too low to cause any tissue reaction in paediatric patients, some image-guided interventional procedures may deliver doses high enough to cause deterministic effects such as skin injuries in some patients. Stochastic radiation risks are of special concern in paediatric patients since children are more vulnerable than adults to the development of certain cancer types and have longer lifespans to develop long-term radiation-induced health effects [4].
Epidemiological data suggest that exposure to ionizing radiation increases cancer risk at organ dose ranges of approximately 50–100 mSv, a level of dose that can be achieved after several CT scans, and that cancer risk from radiation exposure is higher in children compared to adults, with infants at the greatest risk [3]. Figure 2 illustrates how cancer risk associated with radiation exposure is highly dependent on the age at exposure as well as on the organs exposed (e.g. for the same age at exposure an abdominal CT is associated with a higher cancer risk compared to a head CT). However, the risk of developing cancer from low-level radiation such as with diagnostic imaging procedures is not known with certainty.
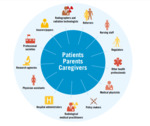
Given the current state of knowledge, and despite the uncertainties about the level of risks associated with multiple exposures/cumulative doses, it is assumed that the low-level of radiation dose used in paediatric imaging may result in a small increase in the risk of developing cancer in the future. Health professionals who prescribe or perform radiological procedures in children need information, education and training to ensure that patients are not exposed to ionizing radiation needlessly or at higher doses than are necessary to produce an image of adequate diagnostic quality. Patients and families should be part of risk–benefit discussions so they understand the information and use it for making informed choices. Figure 3 illustrates the aspects to be considered for the professional- and patient-centered communication and Figure 4 shows the various stakeholders involved in the benefit-risk communication about paediatric imaging.