Congress:
EuroSafe Imaging 2020
Keywords:
Not applicable, Quality assurance, Pathology, Biological effects, Structured reporting, Diagnostic procedure, Audit and standards, MR, Image manipulation / Reconstruction, Cone beam CT, Radioprotection / Radiation dose, Head and neck, eHealth, Action 8 - Radiation protection training and learning material
Authors:
F. Akbarian Tefaghi, A. Adams, J. makdissi
DOI:
10.26044/esi2020/ESI-03588
Description of activity and work performed
We present a case where the use of previous imaging has aided the diagnosis and prevented unnecessary exposure to the patient.
This is a 67-year-old patient attended for a surgical removal of lower left third molar.
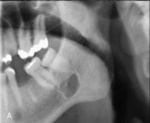
A sectioned panoramic radiograph (Fig.1) showed an incidental finding of a well-defined, unilocular radiolucency measuring 10x7 mm apical to the lower left second and third molars. This was partially superimposed over the outline of the ID canal. A Stafne’s bone cavity (SBC) was considered as the most likely diagnosis 2. Further imaging was considered due to location not being fully below the ID canal as usually described in the literature.
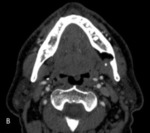
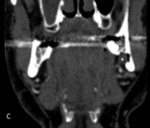
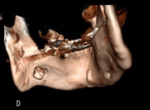
A radiologist opinion was sought. Reviewing previous imaging on PACS revealed the patient has had a CT Angiogram of the head and neck five years prior (Fig.2, Fig.3 & Fig.4).
This showed a lingual bone defect of the surface of the mandible in the region of interest. The extension of the submandibular gland into the defect confirmed the likely nature of SBC .3,4
This is a benign condition also known as lingual mandibular bone defect (LMBD), idiopathic bone cavity, static bone defect or ectopic salivary gland. It describes a cavity on the lingual surface of the mandible often filled with normal salivary gland tissue, but occasionally they contain skeletal muscle, fibrous connective tissue, adipose tissue, lymphatic tissue and blood vessels. 5,6
It requires no further management.