Normal Anatomy
The origins of the hypoglossal nerve are from the hypoglossal nuclei,
which extends through the medulla oblongata in a paramedian location (intra-axial segment).1 The roots of the hypoglossal nerve lie posterolateral to the verteberal artery within the premedullary cistern (cisternal segment).
The roots then merge together to form the hypoglossal nerve,
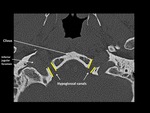
exiting the hypoglossal canal of the occipital bone (skull base segment).
Just medial to the lower border of the jugular foramen is an elevation,
is the jugular tubercle.
Arising from the concave inferolateral margins of the clivus,
the jugular tubercle projects posterosuperioly over the hypoglossal canal.
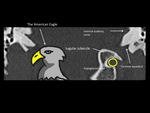
Anteriorly,
the jugular tubercle resemble an eagle's head or beak as it arches over the obliquely oriented hypoglossal canal.2 Fig. 2 The hypoglossal canal contains the nerve and a surrounding venous plexus.
It may occasionally contain a meningeal branch of the ascending pharyngeal artery.
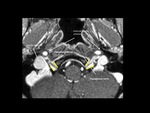
From the hypoglossal canal,
the nerve enters the carotid space,
lying deep to the internal jugular vein,
internal carotid artery,
and glossopharyngeal and vagus nerves.
The hypoglossal nerve is responsible for the motor innervation of the intrinsic and extrinsic muscles of the tongue,
with the exception of the palatoglossus,
which is innervated by the vagus nerve.
Imaging Techniques
Both CT and MR imaging are useful in the assessment of hypoglossal nerve pathology. MR imaging is able to give soft-tissue contrast,
while CT imaging is able to delineate cortical bone.
There are two important sequences which are used when imaging the hypoglossal canal - the cisternographic sequence (eg FIESTA,
SPACE,
CISS) and the post contrast T1 performed as a 3D gradient echo acquisition.
When assessing other nerves in the skull base,
such as the 7th and 8th cranial nerves,
the cisternographic sequence is very useful as it deliniates the nerve from the surrounding CSF.
However,
due to the lack of CSF within the hypoglossal canal,
we have found this sequence to be of limited utility.
In our experience,
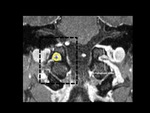
the post gadolinium 3D sequence can delineate the nerve from the surrounding venous plexus.
Imaging Findings
This exhibit is a pictorial review of the normal anatomy,
various imaging techniques and a range of pathologies that can present in the hypoglossal canal.
Hypoglossal Denervation
The denervation process of the hypoglossal nerve can be classified into acute,
subacute or chronic denervation,
each having its own set of imaging features.4 It is important for the radiologist to be aware of these stages as this will allow us to differentiate the inflammatory of neoplastic processes.
Awareness of abnormal enhancement should direct the radiologist to look for a denervating lesion.4
Imaging findings related to the tongue denervation process depends on the chronicity of the denervation process.
In the acute and subacute stage,
the denervated muscle may show increased signal intensity on T2-weighted images.4 Fig. 17,
Fig. 19 This process is likely due to the increase in extracellular water,
which has a longer T2 prolongation than intracellular water,
most likely accounts for the increased T2 signal intensity in the acute and subacute stages of denervation.4 However,
this process may also be attributable to an increase in the extracellular space,
with the expanded extracellular space in the denervated muscle allowing for more contrast to be accmulated in the extracellular space.4 In the acute and subacute stages of denervation,
the initial insult is likely to occur days to weeks following the intiial insult.
Note also that,
on T1 weighted imaging of the patient with acute/subacute denervation,
the image appears normal and one cannot make the diagnosis of denervation.
Fig. 18
Chronic denervation of the hypoglossal nerve is characterised by a loss of volume of the musculature with extensive fatty replacement.4 Fig. 20 In long standing cases,
there will be extensive fatty replacement with significant volume loss of the musculateure.
This process is likely to occur months to years following the intial insult.
However,
further research is required to define the exact time course of these changes.4