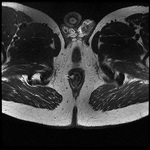
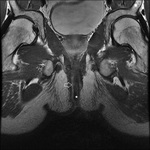
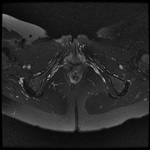
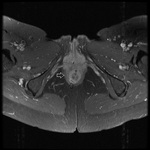
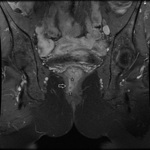
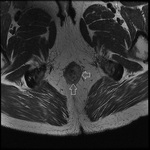
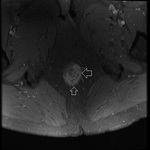
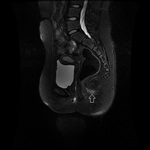
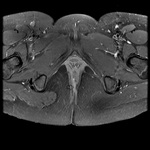
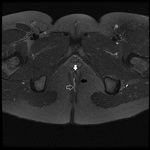
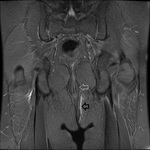
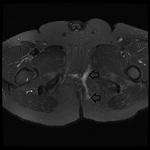
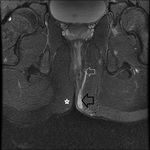
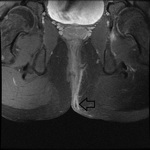
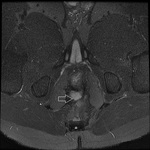
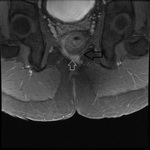
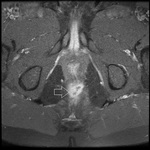
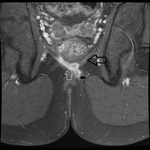
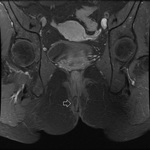
MRI appearance and classification of perianal fistulas using the St James University Hospital Classification(1).
Grade 1 = simple intersphincteric fistula.
Fistulous tract extends from skin of perineum or natal cleft to the anal canal.
No ramification or abscess formation in the intersphincteric plane,
or involvement of the ishioanal or ischiorectal fossa is present.
The fistula is confined entirely within the external sphincter (Fig.
9 & 10).
Grade 2 = intersphincteric fistula with either ramification,
secondary sinus tract or abscess formation within the intersphincteric plane.
No extension beyond the external sphincter is present,
nor is there involvement of the ishioanal and ischiorectal fossa.
The secondary tracts may cross the midline resulting in a horseshoe shape (Fig.
11-13) and (Fig.
14 & 15).
Grade 3 = trans-sphincteric fistula that pierces both layers of the sphincter complex and arcs down within the ishiorectal and ischioanal fossa to the skin (Fig. 16-18).
Grade 4 = a trans-sphincteric fistula with either ramification,
secondary sinus tract or abscess formation in the ischiorectal or ischioanal fossa,
beyond the external sphincter (Fig.
19 & 20) and (Fig.
21 & 22).
Grade 5 = supralevator fistula and abscess extending above the levator ani muscle.
These can result in occult pelvic sepsis and are important as they require different management options (Fig 23-26).
Management options:
Can include either medical management or surgery.
Medical management is often aimed at treating the cause of fistula formation.
For example,
in Crohn’s disease medial treatment would focus on controlling active disease to prevent complications.
This would typically involve using progressively aggressive but also toxic therapy beginning with 5-aminosalycyclic acid (5-ASA),
antibiotics and nutritional therapy.
If this fails,
the next step up would involve corticosteroids and immunomodulators with 6-mercaptopurine (6-MP)/azathioprine or methotrexate.
Biologic agents such as infliximab or adalimumab are reserved for patients with severe Crohn's disease(10).
If medial therapy is insufficient or if there are complications such as fistula/abscess formation,
strictures or bowel perforation,
surgical treatment is indicated.
This can be varied and include seton placement (Fig.
27-29),
fistulotomy,
mucosal advancement flaps,
plugs and adhesives,
bowel resection with primary anastomosis or diversion with colostomy(11).
Proposed reporting checklist:
We propose the following to be paid attention to when reporting fistula MRI studies:
1.
The anatomy of the fistula and its relation to surrounding structures using the anal clock configuration.
2.
Fistula classification including grading (we use the St James Classification at our institution),
location,
and enteric and cutaneous openings.
3.
Any complications associated ie.
pus or secondary sinus/tract formation including their location.
This includes checking for any supralevator extension or pelvic sepsis.
4.
Any evidence of previous surgery/seton placement/fibrous scar tissue.
5.
Any signs of active disease involving the rectum or anus.
6.
Pelvic lymphadenopathy and other miscellaneous findings.