Keywords:
Diagnostic procedure, Plain radiographic studies, Small bowel, Obstruction / Occlusion
Authors:
H. Tie, P. Edwin; QLD/AU
DOI:
10.1594/ranzcr2016/R-0080
Purpose
Small bowel obstruction is one of the most common reasons for hospital admissions – accounting for approximately 15% of patients admitted from the Emergency Department to the Surgical Unit.1 It may be classified as a complete/high grade obstruction with no fluid or gas beyond the transition point,
an incomplete/partial obstruction with some fluid or gas beyond the transition point,
a closed-loop obstruction with 2 points of obstruction which may lead to volvulus and strangulated obstruction which can result in bowel ischaemia and potentially fatal complications like bowel perforation and sepsis2.
Studies have shown that mortality associated with simple small bowel obstruction range from 2-8% but may be as high as 25%4 with associated bowel ischaemia,
which highlights the importance of early diagnosis and management.
However,
patients usually present with clinical symptoms of abdominal pain,
abdominal distension,
nausea,
vomiting and less frequently,
absent or high pitched bowel sounds,
which have low sensitivity and specificity for the diagnosis of small bowel obstruction and its complications.
Suspected small bowel obstruction is therefore one of the most common indications for emergency diagnostic imaging.
The main questions clinicians seek to answer through medical imaging are: 1) Is there a small bowel obstruction? 2) Where is the site of the obstruction? 3) What is the cause of the obstruction? 4) Is it an uncomplicated obstruction for conservative management with nasogastric tube decompression or are there associated complications requiring emergency surgery? 5) Is there another diagnosis for the patient’s symptoms?
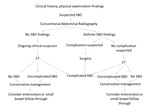
A general algorithm for the diagnostic work up of patients with suspected small bowel obstruction is demonstrated in Fig. 1 .
Plain abdominal radiography currently remains the preferred initial examination3 due to its accessibility,
low cost and for many years,
has been the most accurate diagnostic tool available.4 It is a useful modality in determining if small bowel obstruction is present,
with a sensitivity of 46-80% depending on the grade of obstruction12,
prior to cross sectional imaging for determining the exact location of the obstruction,
aetiology,
presence of complications and other causes for the clinical presentation.
Each institution in Queensland has its own protocol on the acquisition of abdominal radiographs – some preferring only supine radiographs as studies have suggested that the diagnosis of small bowel obstruction is unaffected by the lack of erect abdominal radiographs3 while others obtain both supine and erect images as other studies have shown that sensitivity and specificity increases with the number of positive radiographic signs.4,5
We hypothesize that erect abdominal radiographs add minimal value when acquired with supine abdominal radiographs in the diagnosis of small bowel obstruction.
The purpose of this study is to evaluate if erect conventional abdominal radiography increases sensitivity when used in conjunction with supine abdominal radiography in the diagnosis of small bowel obstruction so as to minimise potentially unnecessary imaging,
decrease radiation exposure of patients,
improve efficiency of the healthcare system and ultimately,
patient outcomes.
Lateral decubitus views may also be acquired in plain abdominal radiography but will not be examined in this study.