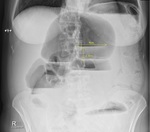
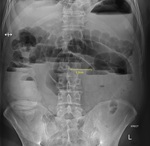
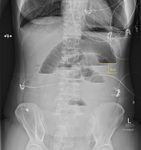
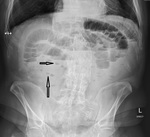
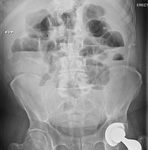
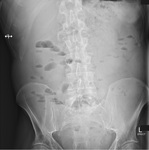
The results are shown on Table 3 .
The prevalence of small bowel obstruction in this study is 11.6% - 26 out of 225 patients.
1 case was confirmed in surgery where adhesions were found.
17 cases were diagnosed based on CT abdomen/pelvis findings and 8 were clinically diagnosed and conservatively managed.
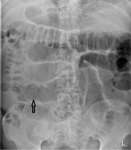
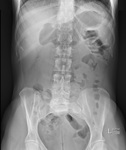
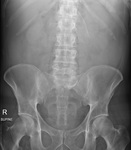
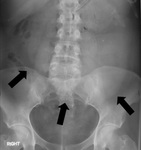
The sensitivity of supine abdominal radiographs Fig. 2 Fig. 3 Fig. 4 Fig. 5 was 88.5% (23/26) whilst the sensitivity of erect abdominal radiographs Fig. 6 Fig. 7 Fig. 8 Fig. 9 was 84.6% (22/26).
However,
of the 3 false negative cases on supine abdominal radiography,
2 cases were identified to be positive for small bowel obstruction on erect abdominal radiography so the sensitivity of a combination of both supine and erect abdominal radiographs is 96.2% (25/26).
The specificity of supine abdominal radiographs was also noted to be 95.0% (189/199) whilst the specificity of erect abdominal radiographs was 88.4% (176/199).
Discussion
Although CT abdomen and pelvis has a sensitivity and specificity of up to 96%8 and abdominal radiographs generally have low yield in positive diagnostic information10 - 10% to 38% of patients with abdominal pain in the Emergency Department have abnormalities on abdominal radiographs11,
conventional abdominal radiography remains the most valuable initial tool in the diagnosis of small bowel obstruction9 – to decide if further imaging,
conservative treatment or emergency surgery is required.6
The greatest limiting factor in conventional radiography’s diagnostic role is that the intestinal gas pattern which interpretation of radiographs is based on varies with severity,
level and duration of the obstruction.5 False negative findings on plain abdominal radiography may also be secondary to the absence of gas in the bowel which may still be distended but is fluid filled7 – making it difficult to detect the bowel distension.
Lappas et al (2001)5 suggested that the 2 most significantly predictive radiographic findings for small bowel obstruction are found on erect abdominal radiographs: 1.
presence of differential air-fluid levels and 2.
width of air fluid levels measuring ≥25mm.
The presence or absence of both of these signs is a strong (86%) positive or strong (83%) negative indicator for small bowel obstruction.
Therefore,
the use of erect radiographs in combination with supine radiographs is recommended even though erect radiographs do not have a high sensitivity on their own.
However,
the limitation or elimination of erect radiographs has been recommended in other studies11,13 which have shown that erect images do not lead to any significant increase in diagnostic information but poor quality of erect images have led to more repeat studies,
increased cost,
inefficient use of the radiographer’s time and increased patient radiation exposure.
In our study,
the sensitivity of erect radiographs (84.6%) is lower than that of the supine radiographs (88.5%) but the addition of erect abdominal radiography to the supine abdominal radiographic examinations led to a 7.7% improvement in sensitivity in the diagnosis of small bowel obstruction.
However,
the low specificity of erect abdominal radiographs (88.4%) compared to supine radiographs (95%) is also noted.
Previous studies from as early as 195813 which have shown that the presence of multiple air-fluid levels on erect abdominal radiographs is not pathognomic of small bowel obstruction and can be observed in other conditions like gastroenteritis,
bowel ischaemia,
ascites or may be drug induced.
In our study,
erect radiographic signs like multiple air fluid levels as well as a maximum width of greater than 2.5cm Fig. 10 and a positive “string of beads” sign Fig. 11 have been demonstrated on erect abdominal radiographs of patients who did not have small bowel obstruction on CT abdomen/pelvis or clinically.
Our findings are similar to that of Simpson et al.
(1985)13 where a slight increase in sensitivity of approximately 5% is noted with the addition of erect abdominal radiographs,
but is thought to likely be reduced with a good clinical history and physical examination findings.
As abdominal radiography is more frequently used as a screening tool to reassure clinicians of their patients’ normality11,14,
the low specificity of erect radiographic findings is of significant importance.
Limitations
There were several limitations in our study.
Firstly,
it is a retrospect study which led to a selection bias.
Systemically unwell patients or those with severe undifferentiated abdominal pain in the Emergency Department generally undergo a CT Abdomen/Pelvis examination in the first instance,
which excludes them from this study.
Conventional abdominal radiography is generally the imaging modality of choice if the patient has mild to moderate undifferentiated abdominal pain,
is systemically well or has a history of recurrent small bowel obstruction requiring conservative treatment.
Secondly,
there is no clear protocol regarding the use of erect abdominal radiography in patients with suspected small bowel obstruction and that decision is usually made by the radiographer.
It is dependent on the clinician’s request – where some may have requested for specific projections.
If there is no specific clinician request,
it is dependent on the radiographer – some first obtain a supine abdominal radiograph and if there are abnormal findings,
an erect abdominal radiograph is then acquired.
This process relies on the level of expertise of the radiographer and also meant that small bowel obstruction undetected on supine abdominal radiographs but may have been detected on erect radiographs would potentially have also been excluded in this study.
Thirdly,
surgical confirmation is only obtained in 1 case and we relied on clinical diagnosis and findings from CT abdomen/pelvis,
which has a very high but not 100% sensitivity or specificity,
for the remainder of the final diagnoses.
However,
this is in keeping with the management of the majority of cases of small bowel obstruction.