Fig.
1
ACUTE CHOLECYSTITIS
Acute cholecystitis is acute inflammation of the gallbladder and is often caused by gallstones,
leading to outflow obstruction[1,
2].
It has a mortality rate of 4%[5].
Plain abdominal radiographs are of limited value as only 20% of gallstones are radio-opaque[3] and gallbladder inflammation cannot be visualised.
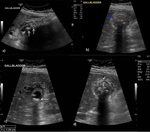
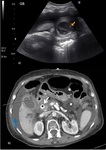
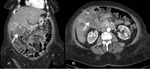
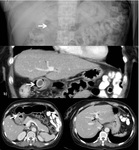
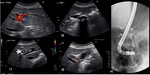
US is the imaging modality of choice and findings include the following with the first two being the most specific ( Fig. 1 )[2]:
- Gallstones which appear as mobile and highly reflective echoes with posterior acoustic shadowing
- Sonographic Murphy’s sign: painful replication of biliary colic by probe pressure on the gallbladder in real time
- Gallbladder distention
- Wall thickening greater than 3 mm.
However this feature may also be associated with chronic inflammation,
ascites,
hypoalbuminaemia,
congestive cardiac failure and sepsis
- Pericholecystic fluid
CT,
although not first-line imaging,
may be performed if the diagnosis is not suspected or uncertain and is a useful adjunct to US when findings are equivocal or if a complication is suspected.
CT findings are similar to US with pericholecystic stranding being the most specific.
However,
it has a sensitivity of 75% for gallstones as some calculi are difficult to detect as they may be isoattenuating to the surrounding bile[6].
MRI is performed when other imaging findings are equivocal or if the clinical picture is uncertain.
The excellent soft tissue contrast provides better detail of the biliary tract and allows identification of inflammatory changes.
On non-contrast T2-weighted imaging,
gallstones appear as signal voids in the high-signal-intensity bile[2] and pericholecystic free fluid appears as high signal intensity around the gallbladder.
Post-contrast T1 imaging demonstrates gallbladder wall thickening.
ACUTE ACALCULOUS CHOLECYSTITIS (AAC)
AAC is an acute necro-inflammatory disease in the absence of gallstones and accounts for approximately 10% of all cases of acute cholecystitis.
It usually occurs in critically ill patients post trauma,
surgery,
burns or those with shock,
sepsis,
on total parenteral nutrition or prolonged fasting.
AAC has higher complication rates including gangrene,
perforation and empyema which occur in 40% of cases resulting in a higher mortality rate of 30%.
The diagnosis is often difficult as there are no specific findings and patients are usually critically ill with no ability to corroborate findings whilst intubated or sedated.
Although no specific clinical factor will lead to the diagnosis,
there should be high clinical suspicion for AAC in critically ill patients for whom no etiology for their condition is found.
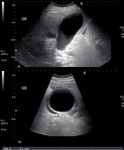
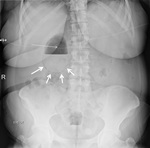
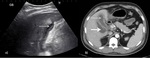
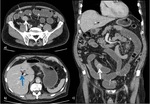
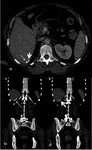
The sensitivity and specificity of US ranges widely from 30-100% ( Fig. 2 ).
CT may be a useful adjunct for establishing the diagnosis.
Major and minor diagnostic criteria have been described as follows with the diagnosis requiring 2 major or 1 major and 2 minor criteria[7].
Major criteria
- 3.5 – 4 mm (or more) thick wall (if at least 5 cm distended longitudinally with no ascites or hypoalbuminemia)
- Pericholecystic fluid (halo)/subserosal oedema
- Intramural gas
- Sloughed mucosal membrane
Minor criteria
- Echogenic bile (sludge)
- Hydrops distension greater than 8 cm longitudinally or 5 cm transversely
COMPLICATED ACUTE CHOLECYSTITIS
Gangrenous cholecystitis
Severe form of acute cholecystitis associated with vascular compromise,
intramural haemorrhage,
necrosis and abscess formation.
The incidence ranges from 2 – 30% with higher incidence in males,
the elderly and those with cardiovascular diseases.
This condition is often caused by stone impaction in the cystic duct leading to progressive gallbladder distension and ultimately ischaemic necrosis of the wall[1,
2].
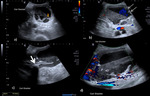
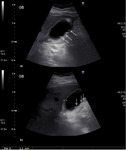
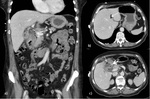
US features include heterogenous striated thickening and irregularity of the gallbladder wall and intraluminal membranes from ulceration,
haemorrhage,
necrosis or microabscess formation.
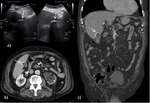
Other signs include pericholecystic fluid collection,
liver or pericholecystic abscess following perforation ( Fig. 3 )[8].
The sonographic Murphy’s sign may be absent secondary to denervation of the gallbladder wall[2].
CT findings are similar to US but an additional finding on contrast-enhanced CT is irregular or absent gallbladder wall enhancement[9].
Haemorrhagic cholecystitis
This is an uncommon complication of acute cholecystitis with a high mortality rate.
It usually occurs in cases of cholelithiasis and gangrenous cholecystitis where transmural inflammation causes mural necrosis and ulceration,
resulting in haemorrhage into the gallbladder lumen.
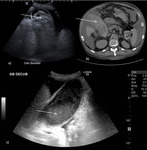
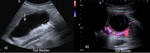
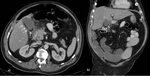
On US,
blood in the gallbladder lumen appears hyperechoic and is generally more hyperechoic than biliary sludge ( Fig. 4 ).
However,
clotted blood may appear as heterogenous echogenic material adherent to the gallbladder wall and may simulate a mass.
A fluid-fluid level with a high attenuation-dependent component may be observed on CT[10].
Perforated cholecystitis
Perforated cholecystitis is a potentially life-threatening condition often as a complication in 0.8 – 3.2 % of cases of acute cholecystitis or trauma.
Gallstone impaction within the cystic duct leads to obstruction and bile accumulation within the gallbladder causing distension.
Progressive distension causes vascular compromise leading to perforation.
Gallbladder perforation can be classified into 3 types:
- Type 1: acute free perforation of the gallbladder into the peritoneal cavity without protective adhesions (highest mortality)
- Type 2: subacute perforation surrounded by a pericholecystic abscess walled off by adhesions (most common)
- Type 3: chronic perforation with presence of a fistulous communication between the gallbladder and a viscus
Imaging plays a vital role as symptoms are non-specific and urgent cholecystectomy is needed.
The “sonographic-hole” sign which is the direct visualization of a gallbladder wall defect on US,
CT or MRI is very specific but not always visualized ( Fig. 5 ).
Other signs include identification of gallstones outside the gallbladder in the correct clinical setting,
focal gallbladder wall bulge,
pericholecystic abscesses and cholecystoenteric fistula in chronic cases[11].
Emphysematous cholecystitis
Emphysematous cholecystitis is a complication of acute cholecystitis characterised by gas within the gallbladder wall or lumen in the absence of an abnormal biliary-enteric communication.
Cystic artery compromise leads to proliferation of gas-producing organisms such as C.
perfringens,
E.
coli and Klebsiella species causing local ischaemia.
It is more common in males,
many of whom have diabetes mellitus.
The mortality rate of 15-20% is reduced by broad-spectrum antibiotics and early emergency cholecystectomy[12].
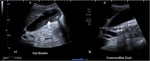
US findings depend on the amount and location of gas.
Small amounts of gas appear as echogenic foci with posterior acoustic shadowing or a posterior ring-down artefact ( Fig. 6 ,
Fig. 7 ).
Large amounts of gas appear as a wide band of acoustic shadowing.
However,
it may be difficult to differentiate emphysematous cholecystitis from porcelain gallbladder or a highly contracted gallbladder filled with gallstones[13].
CT is more sensitive than US and findings include intraluminal or intramural gallbladder gas and complications such as pericholecystic inflammatory changes,
abscess formation or perforation[14].
Gallbladder empyema
Gallbladder empyema ( Fig. 8 ,
Fig. 9 ) is an uncommon but serious complication,
usually seen in adults with diabetes.
It occurs when pus accumulates within an obstructed gallbladder.
Initial symptoms as similar to cholecystitis but high fevers develop as the disease progresses.
It can lead to perforation and sepsis if not promptly treated.
US is the modality of choice but pus within the gallbladder may resemble sludge.
However,
intraluminal gas suggests empyema rather than simple cholecystitis.
CT plays a complementary role by providing more anatomical detail and gas within the empyema.
Percutaneous cholecystostomy are often performed rather than cholecystectomy as these patients are too unwell to tolerate a general anaesthetic.
Aspiration of pus during the procedure also allows the establishment of the definite diagnosis[15].
Acute cholecystitis with hepatic abscess
A hepatic abscess is a localized collection of purulent material within the liver with associated destruction of hepatic parenchyma and stroma with pyogenic ones being the most common in developed countries.
This could be secondary to ascending cholangitis from biliary obstruction,
direct or haematogenous spread[16].
On US,
pyogenic abscesses appear hypoechoic or echogenic,
poorly defined with irregular walls,
demonstrate posterior acoustic enhancement and contain fluid-debris levels ( Fig. 10 ).
However,
appearances are variable and diffusely echogenic abscesses with little posterior enhancement may mimic solid lesions[16].
As necrosis and liquefaction occurs,
the abscess becomes increasingly cystic with septations,
internal echoes and debris.
Doppler may show surrounding hyperaemia[2].
On post-contract CT,
abscesses appear as low-density lesions with thick enhancing rims[2].
Septations may also be seen.
OTHER ASSOCIATED CONDITIONS
Choledocholithiasis
Biliary calculi that form de novo within the biliary tree are referred to as primary stones whilst those that migrate through the cystic duct or a cholecystocholedochal fistula are referred to as secondary stones,
which form the majority.
Impacted stones within the common bile duct may lead to potentially life-threatening suppurative cholangitis and necrotizing pancreatitis[17].
Although the normal common bile duct calibre is slightly increased in the elderly,
a diameter greater than 8 mm raises the concern of ductal obstruction[3].
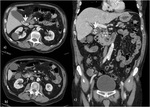
US ( Fig. 11 ) has a sensitivity ranging from 22 – 75%,
limited by the ability to visualize the entire common bile duct,
especially the distal part which may be obscured by bowel gas[18].
Unenhanced helical CT ( Fig. 12 ) has a sensitivity of 88%[18] with 4 criteria described[2]:
- Target sign: central density within the bile duct (calculus) with surrounding low density (bile or mucosa)
- Rim sign: refers to the calculus outlined by a rim of increased density
- Crescent sign: bile eccentrically outlining the calculus,
creating a low attenuation crescent
- Indirect signs: include abrupt termination of the dilated distal common bile duct without visible surrounding mass or biliary dilatation
CT Cholangiography with intravenous iodinated cholangiographic agents have a higher sensitivity of 85-89%[18].
Intraductal calculus appear as filling defects within the biliary tree which has been opacified by contrast.
Magnetic Resonance Cholangiopancreatography (MRCP) is a non-invasive and low-risk technique with sensitivities higher than US and CT and almost equal to that of Endoscopic Retrograde Cholangiopancreatography (ERCP) at 88%–95% and 89%–96% respectively[18].
MRCP include heavily T2 weighted sequences.
Stones generally appear as well circumscribed low signal intensity filling defects within the biliary tract.
MR is also helpful for differentiation of non-calcified stone from a soft tissue mass[2].
ERCP is highly sensitive and specific for choledocholiathiasis and allow therapeutic intervention but carries a 4% complication risk including pancreatitis,
haemorrhage and death.
Therefore,
it is generally reserved for those who require stone removal[19] such as those with cholangitis or biliary obstruction.
Gallstone ileus
Gallstone ileus results from chronic cholelithiasis causing gallbladder perforation and cholecystoenteric fistula formation with the duodenum being the most common,
followed by the colon and stomach[18].
If the migrated gallstone is larger than 2.5 cm,
it usually lodges within the lumen of the small bowel causing mechanical bowel obstruction.
The most common site is the narrow ileocaecal junction and it accounts for 1% of all small bowel obstructions.
Bouveret syndrome ( Fig. 13 ) occurs when an obstructing gallstone within the duodenum causes gastric outlet obstruction[3].
On plain radiographs,
the Rigler’s triad of the obstructing gallstone,
pneumobilia and small bowel obstruction may be seen but CT ( Fig. 14 ) is superior as it allows identification of the location of the obstructing calculus and choledochoenteric fistula ( Fig. 15 ,
Fig. 16 )[20].
Mirizzi syndrome
Mirizzi syndrome is partial obstruction of the common hepatic duct secondary to calculus impaction causing chronic inflammation in the adjacent Hartmann’s pouch[3].
It is an uncommon complication and occurs in 0.05 – 2.7% of patients with longstanding cholelithiasis[21].
Preoperative diagnosis is important as it leads to an increased risks of bile duct injury (up to 22%) and conversion to open cholecystectomy[3].
Diagnosis may be made by US,
CT or MRI with the hallmark being intrahepatic and common hepatic duct dilatation to the level of the porta hepatis with normal distal common bile duct calibre.
A stone may be identified in the gallbladder neck or cystic duct.
Multiplanar imaging with CT or MRI may be helpful in differentiating the extrinsic nature of the obstruction ( Fig. 17 )[2].
Dropped gallstones
Spillage of gallstones occur in 2.3% – 40 % of cholecystectomies,
with 1 – 40% of them retrieved.
Microscopic evaluation of stones confirmed the presence of viable bacteria in pigmented stones which may lead to abscesses.
Due to the indolent nature of inflammation secondary to these spilled gallstones,
complications may occur from the immediate post-operative period to an interval of 20 years.
In laparoscopic cholecystectomy,
creation of pneumoperitoneum and irrigation of the peritoneal cavity can disperse the spilled gallstones to the subhepatic space,
right subphrenic space,
port sites,
right flank,
retroperitoneum,
pelvis or thorax.
US and CT are the modalities of choice.
In CT,
gallstones may appear as hypoattenuating or hyperattenuating nodules resembling peritoneal seeding with the perihepatic area being the most common location ( Fig. 18 ).
Imaging-guided percutaneous drainage and antibiotics are customary management options if there is abscess formation but definitive recovery of stones is often better[22].
CHRONIC CHOLECYSTITIS
Chronic cholecystitis involves an evolving inflammatory process occurring with repeated episodes of gallbladder obstruction leading to focal ulceration and/or necrosis of the mucosa.
88% of cases are associated with gallstones but other causes include tumour,
fibrosis or external cystic duct compression[3].
US findings include gallstones,
thickened gallbladder wall and gallbladder contraction persisting with fasting.
CT findings include dystrophic calcification and pericholecystic inflammatory change[2,
3].
Porcelain gallbladder
Porcelain gallbladder is a rare condition characterized by gallbladder wall calcification found in 0.06 – 0.08% of autopsies.
It is associated with increased risk of gallbladder malignancy of 5 – 12% and cholecystectomy should be considered[23].
However,
more recent studies are questioning this association[24].
On plain radiograph,
the calcifications appear as linear or curvilinear in the right upper quadrant or mid abdomen in the shape of the gallbladder.
On US,
the calcifications are curvilinear and echogenic with posterior acoustic shadowing in the gallbladder fossa.
Other conditions that may appear similar include emphysematous cholecystitis and the wall-echo-shadow complex in cholelithiasis in a collapsed gallbladder.
CT is the most sensitive for identification of gallbladder wall calcification ( Fig. 19 )[24].