Technique:
While the concept of tomosynthesis in radiology is not new by any means,
its first application to breast imaging came in the 1990s6.
In DBT image acquisition the x-ray tube performs a series of low-dose exposures as it moves over an arc of variable range.
The acquired images are converted into a stack of thin slices using a variety of reconstruction algorithms including back projection,
filtered back projection and maximum likelihood algorithms7.
A detailed discussion of reconstruction techniques is beyond the scope of this presentation.
Different manufacturers have different specifications for acquisition time,
angluar range and tube motion.

Fig. 3: *Newer systems like the MAMMOMAT Revelation provide up to 50 degrees angular range. A detailed discussion of the technical differences between systems is beyond the scope of this exhibit.
References: Author's own table with information from manufacturers.
The 3D reconstructed mammograms are traditionally obtained in medio-lateral oblique (MLO) and cranio-caudal (CC) views similar to standard 2D mammography8.

Fig. 4: Image courtesy of Dr. Mark A Helvie, University of Michigan Department of Radiology.
References: Radiologic Clinics of North America
The low dose exposures for each DBT series can also be used to create a synthesized 2D image similar to standard mammography.
Data from the 3D acquisition is condensed into a single image using a similar technique to the Maximum Intensity Projection (MIP) used in CT.
While synthesized views are not yet true replacements for 2D mammography,
they can be useful as a 2D overview and correlate.
Radiation Dose:
Radiation dose to the breast is measured using mean glandular dose (MGD).
The MGD approximates the radiation delivered to the at-risk glandular tissue using a Monte-Carlo simulation derived conversion factor specific to the beam quality (the normalised glandular dose coefficient).
There is variation in this conversion factor based on density of the breast,
x-ray spectrum and breast size and thickness,
particularly in the MLO projection. Much like in standard mammography,
positioning and compression can thus have a significant effect on dose.
Standard DBT sequences result in an increased MGD when compared to standard 2D digital mammography (for the same compressed breast thickness and fibroglandular fraction).
The increase in a single view for DBT alone over standard digital 2D mammography is in the order of 0.5mGy to 1.2mGy.
DBT in addition to standard digital 2D mammography results in an average increase of 2mGy up to 2.5mGy.
It is still unclear what this increase means in terms of radiation risk and obviously the implications differ in the screening and diagnostic populations9.
One strategy to reduce this dose is the use of the previously mentioned synthesised 2D mammogram.
Modern DBT systems use tungsten targets with aluminium,
silver or rhodium filters and operate at higher kilovolt peaks than standard 2D digital mammography systems in part to reduce radiation dose.
Information Technology and PACS considerations:
DBT image files require much larger storage space compared to standard 2D mammography.
An uncompressed single view DBT may require 200-450 MB as compared to 8-24 MB for 2D mammography.
Storage of compressed files without information loss is recommended.
Furthermore,
DBT workstations require more random access memory to enable smooth scrolling of the image set.
Existing PACS systems require different hanging protocols,
image annotation tools and the ability to scroll through the stack of images10.
Current applications and use of DBT:
Screening:
The majority of evidence for DBT has come from large screening trials comparing DBT + 2D mammography to 2D mammography.
The main outcome measures in these trials are a reduction in recall rates and an increase in cancer detection rates10.
Further evaluation of resource utilization and cost-effectiveness is needed before DBT is truly validated in a screening setting. In Australia,
a pilot study [registered trial (ACTRN12617000947303)] at Maroondah BreastScreen,
Victoria is underway to assess the feasibility and the outcomes of using DBT for routine breast screening.
Several studies have also investigated the use of replacing standard mammography with synthesized views with the aim of reducing total examination dose.
Such studies have shown similar recall rates between synthesized view with DBT and 2D mammography with DBT.
In addition,
cancer detection rates were improved with use of synthesized views with DBT compared to 2D mammography and DBT11-13.
Early studies evaluating the use of single-view DBT in a screening setting have also shown promising results. The Malmö Breast Tomosynthesis Screening Trial assessed single-view DBT (MLO) and compared it with standard 2D mammography (MLO and CC).
The study showed a learning curve but with improvement in false positive recalls over time14.
Wallis et al.
showed similar classification accuracy between 2D mammography and single-view DBT15 while Waldher et al.
showed better sensitivity and negative predictive value in single-view DBT versus 2D mammography in both screening and diagnostic settings16.
Diagnostic work-up:
Several BreastScreen assessment clinics in Australia,
including our institution,
have adopted DBT for assessment of screening-recalled abnormalities.
In many cases DBT may obviate the need for work-up views and assessment ultrasound.
This correlates with the literature,
which has also described improved radiologist performance in the assessment clinic17.
For symptomatic women,
DBT provides better characterisation of indeterminate lesions compared to standard 2D mammography3.
In a follow-up of women with a history of breast cancer,
DBT has been used with 2D mammography in many radiology practices in Australia.
The role of DBT in this setting is yet to be proven in large cohorts.
Assessment of breast lesions:
Benign lesions:
Given the accuracy of DBT in reducing tissue overlap and summation,
overall detection of all types of lesions is generally improved.
Characteristics of cystic lesions are often depicted better on DBT (Fig. 6).

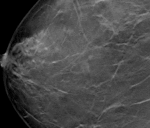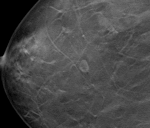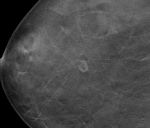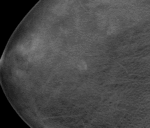
Fig. 5: Multiple cysts seen on standard digital 2D mammography. These were confirmed with ultrasound correlation and stable over time.
References: Breastscreen Victoria

Fig. 6: Selected tomosynthesis images from the same patient in Fig. 5 demonstrating the well defined margins and characteristic rounded shape of the benign cysts.
References: Breastscreen Victoria
Other benign lesions containing fat such as fibroadenolipomas/hamartomas (Fig. 7) will also show benign features on DBT.

Fig. 7: Selected tomosynthesis images from a patient with a biopsy confirmed fibroadenolipoma. Note the characteristic fat density within the lesion.
References: Breastscreen Victoria
In addition,
intramammary lymph nodes (Fig. 9),
dermal and subcutaneous lesions (Fig. 10,
Fig. 11) as well as vascular calcifications can be assessed on DBT,
often without the need for additional views.
However,
general benign features of shape and margins should not falsely reassure radiologists when a benign-looking lesion is new or shows interval growth.

Fig. 12: Biopsy proven mucinous (colloid) carcinoma of the breast. Note the well defined, regular margins suggestive of benign aetiology.
References: Breastscreen Victoria
Well-circumscribed lesions close to the nipple require careful assessment and often still require adjunct evaluation with ultrasound and biopsy.

Fig. 13: Subtle solid lesion behind the nipple on these selected DBT images represented a papillary carcinoma on biopsy.
References: Breastscreen Victoria
Malignant lesions:
DBT has been shown to have a higher detection rate in a screening setting with increased sensitivity for small lesions.
In addition,
subtle architectural distortion or fine spiculations can be more evident on DBT than standard 2D mammography (Fig. 2).
A two-view DBT allows assessment of multifocal lesions within the same breast doing away with the need for multiple spot compression/magnification views

Fig. 14: A spiculated lesion in the outer breast was found on screening mammography.
References: Breastscreen Victoria

Fig. 15: Selected DBT images from the same patient from Fig 14 demonstrate a second solid lesion anterior to the spiculated lesion picked up on screening.
References: Breastscreen Victoria
Architectural distortion:
Recall rates are generally reduced for DBT compared to 2D mammography alone due to a marked reduction in asymmetric densities.
However,
assessment with DBT may lead to more recalls for AD18.
Areas of surgical scarring can reveal significant distortion and interval change may require further assessment with ultrasound or biopsy.

Fig. 16: A solid lesion at the deepest aspect of the inferior surgical scar was initially picked up on tomosynthesis. US guided biopsy demonstrated recurrent ductal carcinoma.
References: Breastscreen Victoria
Dense breasts:
The use of DBT in women with dense breasts has shown promising results.
In a screening study of patients with dense breasts and mammography-negative lesions,
DBT detected more than 50% of the additional breast cancers that were detected with adjunct breast ultrasound19.
There is some evidence suggesting limitations in the setting of extremely dense breasts however20.
Overall,
cancer detection rates in women with dense breasts seem improved with the use of DBT21.
DBT-guided biopsy:
Lesions identified on DBT that cannot be identified on 2D mammography,
spot compression/magnification views and/or ultrasound are rarely encountered.
However,
such lesions may require further assessment with magnetic resonance imaging or biopsy under DBT guidance.
Pitfalls:
Calcifications:
DBT appears to have significant limitations when it comes to the assessment of microcalcifications.
A multicentre study showed an estimated sensitivity and specificity,
respectively of 100% and 94.6% for 2D mammography and 91.1% and 100% for DBT22.
One explanation is that microcalcifications are not well visualised on DBT due to their location in different planes. At our institution,
assessment of microcalcifications still requires magnification views in CC and lateral projections.
Synthesised views:
The synthesised view is a useful tool that can provide a quick overview as well as a stand-in for conventional 2D mammography.
Occassionally the synthesised view can reduce the conspicuity of lesions.

Fig. 17: A standard 2D mammography projection demonstrates a spiculated mass.
References: Breastscreen Victoria

Fig. 18: On the synthesised view created from the DBT set of the patient in Fig 17. the lesion is less conspicuous.
References: Breastscreen Victoria
Another potential pitfall is pseudo-calcifications which may appear in synthesized 2D images.
These pseudo-calcifications arise from ligaments or vessels and should not be visible on two planes23.
Out-of-plane artefact:
This is also known as zipper or slinky artefact which results in replications of high of high-density objects such as surgical clips24.

Fig. 19: Classic "zipper" artefact seen in relation to surgical clips.
References: Breastscreen Victoria
High density artefact:
Much like in other forms of radiography, photon depletion causes areas of low density around a high-density object24.
This results from strong attenuation and while it commonly occurs in relation to surgical clips and other metal objects it can also be seen adjacent to dense calcification.

Fig. 20: Popcorn calcification in a fibroadenoma, note the photon starvation artefact at the margins of the dense calcification.
References: Breastscreen Victoria
Lesion localization and breast positioning:
DBT image sets are provided as a stack of slices.
A scroll bar is noted indicating the number of slices and the position of the slice in the stack.
However,
care should be taken when breast positioning is not optimal and the middle slice should not be assumed to represent the centre of the breast.
The position of the nipple in relation to the stack is often a better indicator for lesion localization.
When the breast is rolled more than expected,
false localization of lesions in upper versus lower breast may occur.

Fig. 21: In this particular DBT series the nipple had rolled under the breast and was present on the last image of the set making lesion localisation more complicated than usual.
References: Breastscreen Victoria