Keywords:
Interventional vascular, Fluoroscopy, Audit and standards, Venous access, Blood, Cancer
Authors:
B. Chan; Brisbane, QLD/AU
DOI:
10.26044/ranzcr2021/R-0043
Methods and materials
A Port-a-cath is a subcutaneously placed totally implantable device that allows long-term venous access. This is essential for many patients, especially those undergoing chemotherapy. It has almost completely replaced external catheters when ongoing intermittent venous access is required.
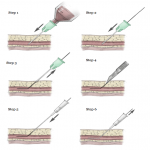
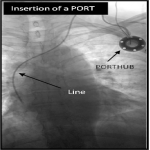
The procedure is usually performed under local anesthetics. Under ultrasound guidance, the internal jugular vein or subclavian vein is accessed using Seldinger technique - a needle guide wire is passed through, followed by a dilator sheath introduction over the guide wire (fig.1) [1,2,4,6,7]. A pocket large enough to accommodate the port chamber is created in the subcutaneous tissue below the clavicle. The catheter is then tunneled through subcutaneously from the pocket to next to the guide wire entrance (fig.2). The estimated distance from the entrance of the guidewire to the cavoatrial junction is measured before the guide wire is removed. The appropriate length of the catheter is determined, and excess catheter is cut away. The catheter is then threaded through the dilator sheath. The sheath is removed by splitting apart (fig.3). The appropriate position of the catheter tip at the cavoatrial junction should be confirmed with fluoroscopy (fig.4).
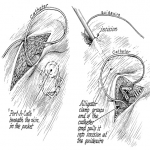
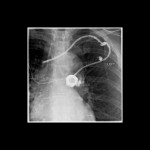
Complications of Port-a-cath insertion can be perioperative or late [3,5]. Perioperative complications include pneumothorax, haemorrhage, and catheter embolisation. Late complications include infection, thrombosis, extravasation (fig.5), port malposition, and catheter migration (fig.6). Discussion of these complications is beyond the scope of this audit. Some have described anchoring the port chamber in the pocket can avoid port malposition. This is done by suturing the port to the underlying fascia at its base. This theory remains controversial, and is not routinely performed among interventional radiologists [2,4].
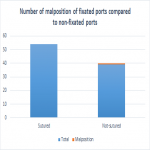
This audit aims to evaluate whether suture fixation of the port is correlated with a reduced incidence of port malposition. All Port-a-cath insertions performed between 01/01/2017 and 30/12/2019 by two interventional radiologists in the Redcliffe hospital were reviewed. One of whom uses the suture fixation technique, and the other does not. The number of patients whose port malpositioned within two months post-insertion were compared between the two groups. Those who did not have a subsequent imaging of the chest after two months to allow evaluation of port position were excluded in this audit. Malposition is defined as one that can no longer be accessed percutaneously, and thus requires removal and reinsertion. All data was collected via Synapse and The Viewer. Statistics were obtained by Medcalc statistical software.