Keywords:
Bones, Musculoskeletal bone, Neuroradiology brain, CT, Nuclear medicine conventional, Diagnostic procedure, Osteoporosis
Authors:
M. Macbain1, M. Kok2, G. Wiggins1, S. T. Lee1, E. Lau1, N. Kutaiba1; 1Heidelberg, VIC/AU, 2Box Hill, VIC/AU
DOI:
10.26044/ranzcr2021/R-0131
Results
Of the 327 subjects included, 206 were female and 121 were male. The mean age was 68.7 years (range 21–96 years) and the mean body mass index was 28.5. No significant difference was demonstrated between the Austin and Eastern cohorts in terms of skull density, age or BMI, however, there was a significant difference in femoral neck T-score between the two cohorts (-1.566 vs -1.107, p=0.001).
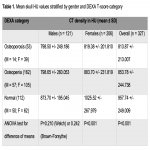
There was a statistically significant difference between the mean skull density (HU) of subjects with normal bone mineral density, osteopenia and osteoporosis across the whole cohort (p<0.001). This difference was also seen in female subjects (p<0.001) but not males (p=0.210) (Table 1).
There was a statistically significant correlation between skull density on CT and femoral neck T-score for the overall cohort (r=0.282, p<0.001) and for females (r=0.406, p<0.001), but not amongst males (r=0.138, p=0.131)(Fig. 2).
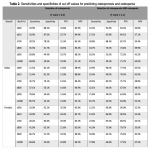
Multiple skull density thresholds were tested for utility in diagnosing osteoporosis and osteopenia (Table 2). The area under receiver operator curve (AUC) for the whole cohort was 0.598 (95% CI 0.519–0.677); the AUC for females was 0.626 (95% CI 0.533-0.719); the AUC for males is 0.566 (95% CI 0.411-0.721)(Fig. 3).
While the threshold used in a prior study3, 610 HU, proves to be quite a specific predictor of osteoporosis, it is very insensitive in our cohort (specificity 87.6%, sensitivity 18.9% for the overall cohort). In our study, sensitivity for detecting osteoporosis increases as the skull density threshold increases, but specificity reduces, such that a clinically useful threshold is not determined.
The results of this study are significant, but with a smaller AUC than demonstrated by Na et al3. This may be because of the difference in skull density measurement technique; our study used a region of interest tool which is likely affected by cortical bone in subjects with narrow medullary cavity, whereas Na et al. used a linear histogram tool which can be better centred between the inner and outer table of the bone. Our results are more significant for frontal bone density than those demonstrated by Amin et al.4, which likely relates to our larger sample size.