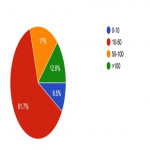
There were 47 responses from ROs in Australia (36), NZ (10) and Singapore (1) across 32 centres. 90% worked in public centres, with over a third working at centres operating 2-3 Linacs (36%). 61.7% of the ROs treated 10-50 patients with BM annually.
57% of responders had SRS and/or stereotactic radiotherapy (SRT) capabilities across 20 centres including 1 Cyber Knife, 2 Gamma Knife and 43 linac-based platforms. Various combinations of technologies were used, including mirco MLCs, robotic couches and cones. The majority of responders used CBCT for IGRT, followed by ExacTrac and then by Vision RT.
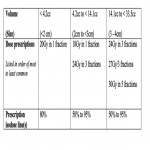
SRS was considered by 25% of ROs for less than 10 BM and or less than 15cc total volume of BM whilst 50% of ROs selected WBRT instead for more than 4-6 BM. Total number and patient’s age were ranked equally (38%) in deciding between fractionations. MRI is the commonest surveillance investigation performed three monthly by the majority of ROs (78%).
For SRS, GTV to PTV margins were between 0-3mm (5 x 0mm, 11 x 1mm, 8 x 2mm, 3 x 3mm). 40% of ROs left this question unanswered. Three to seven days (range: same day to more than 2 weeks) was the commonest interval between day of simulation and delivery. Large volume of oedema influenced the use of prophylactic dexamethasone in asymptomatic patients. There was a broad range of minimum BM size (range: 1-15mm) for which SRS would be offered with a median size of 5mm .
Following BM surgery, approximately half of ROs would treat the surgical cavity alone following a complete macroscopic resection and 24Gy in 3# was the most common SRS dose-fractionation (38%).
Role of WBRT
For WBRT, 30Gy in 10 fractions was the most commonly prescribed dose-fractionation in good performance status patients (76%). Hippocampal-sparing WBRT utilisation in select cases (< 25% cases) by 51% of ROs, keeping in mind this survey was conducted prior to publication of the results from the NRG Oncology CC001 Phase III randomised trial.2
Systemic treatment and sequencing of WBRT
There was a great divide amongst ROs regarding the preferred duration of time to withold EGFR TKIs, BRAF/MEK and ALK inhibitors prior to delivering WBRT.
Well over half of respondents felt comfortable administering Herceptin (59.1%) concurrently with WBRT, under half (42.2%) would deliver WBRT concurrently with immunotherapy. More than two-thirds of ROs would allow more than 72 hours following chemotherapy to deliver WBRT.
Systemic treatment and sequencing of SRS/SRT
There was also a great range of preferred duration of withholding EGFR TKIs, BRAF/MEK and ALK inhibitors prior to delivering SRS/SRT. The majority of ROs would withhold these agents at a minimum of 24 hours to more than 72 hours.
Again, the majority, three-quarters of respondents, felt comfortable administering Herceptin (74%) concurrent with SRS/SRT, just under half (44%) would deliver SRS/SRT with immunotherapy. More than two-thirds (70%) would allow greater than 72 hours between chemotherapy and SRT/SRS delivery.
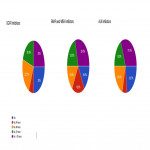
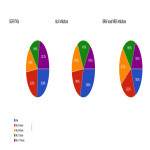
Commonly selected doses for various volumes in Non-eloquent and Eloquent BM locations
Patient Scenarios
ROs were asked to select when they would recommend firstly delivering SRS/SRT prior to commencing targetted therapies, in patients with controlled extracranial disease in various scenarios e.g. in patients with symptomatic vs. asymptomatic BM at presentation and BM in eloquent vs non-eloquent loaction(s).
For patients with symptomatic BRAF mutant melanomas BM, an SRS approach was chosen to be delivered upfront prior to commencing BRAFi/MEKi regardless of number of brain metastases. This was also the case where BM were located in eloquent locations
Again for patients with EGFR/ALK mutant non-small cell lung caner (NSCLC) SRS was selected in those with symptomatic BM in preference over EGFRi/ALKi regardless of number of brain metastases and also if the BM were in eloquent locations.
As to be expected, across both patient cohorts, SRS/SRT was not as strongly favoured to be commenced upfront over targetted therapies in patients with > 5-10 BM compared to those cases of 1-3 BM.
Decision making factors
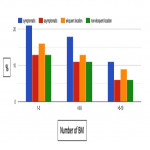
In patients with excellent performance status (ECOG 0-1) with 1-5 brain metastases 30-40% of ROs would treat these with SRS/SRT over WBRT alone. When the number of BM exceeds > 10 and or the volume >15cc ROs preferred WBRT over SRS/SRT. Whilst patients with poor PS (ECOG 3) would be often managed with best supportive care, WBRT and SRS.
The most common factors which influenced the ROs decision to recommend WBRT over SRS include listed in decreasing frequency:
- number of BM
- patient’s performance status
- extent and control of extra-cranial disease
- previous SRS/SRT
- size of BM
- previous WBRT
- total volume BM
- systemic treatment options available
- location of BM
- patient age
- neurological deficits
- response to steroids
Follow-up for treated brain metastases
MRI was the commonest surveillance investigation performed following SRS with a three monthly interval for surveillance (83%). Following WBRT imaging was performed in the setting of symptoms.