Keywords:
Breast, Oncology, Mammography, MR, Screening, Cancer, Outcomes, Pathology
Authors:
K. Gladysz, L. Borella; Sydney, NSW/AU
DOI:
10.26044/ranzcr2021/R-0201
Results
Data collection and evaluation was performed on 200 patients consisting of 199 females (99.5%) and 1 male (0.5%). Patients were aged between 18-85 years [Mean age of 53 years with a SD ± 12.5).
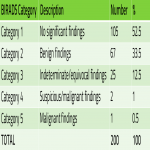
Most patients, 172 (86%) were classified as BIRADS 1 and 2, with the remaining 28 (14%) being classified as BIRADS 3-5.
Based on the BIRADS category:
- 155 patients were recommended to return to routine screening.
- 28 patients identified as BIRADS ≥ 3 were recommended for further investigations (Figure 2).
45 patients subsequently underwent further investigation. The disparity in numbers for further investigation was attributed to patients seeking additional investigations through General Practitioners (GP’s) or other specialist referrals post AB-MR results. These investigations were not recommended in the MRI reports.
There was no significant difference between breast density groups with mild, moderate and marked density percentages of 33.5%, 32% and 34.5% respectively.
Background enhancement demonstrated greater variability with mild, moderate and marked categories being 66.5%, 24% and 9.5% respectively.
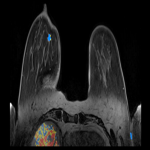
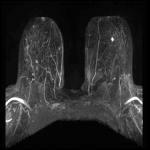
Nine breast cancers were identified in eight patients from the 200 screening AB-MRs performed, giving a cancer detection rate of 9/200 (4.5%) with a recall rate of 9% and PPV greater than screening mammography of 44% (Figures 4-6).
The 9 cancers yielded were all in the group of patients recommended for further investigations by the radiologists (28 patients), with no cancers yielded in the remaining 17 patients who underwent further investigations with their GP’s/other specialist referrals.
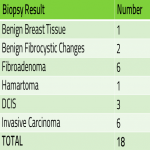
Final diagnoses were obtained from the surgical reports and are shown in Figure 3.
In the cancer group there were 7 females and 1 male with a mean age of 60 years. A family history of breast cancer was indicated in 3 of 8 patients and no patients with a family history of ovarian cancer.
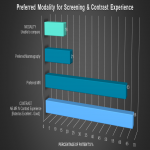
Patient satisfaction survey results indicated an overall patient preference for AB-MR (75%) as compared to mammography screening (25%) in those who could make the comparison. Intravenous contrast administration was well tolerated (rated as excellent/good experience in 68%).