Keywords:
Interventional non-vascular, Oncology, Urinary Tract / Bladder, CT, MR, Dosimetry, Radiation therapy / Oncology, VMAT and Tomotherapy, Dosimetric comparison, Radiotherapy techniques
Authors:
M. Chao1, D. Lim Joon2, Y. Chan2, A. Tan3, M. Cokelek1, H. Ho1, P. Manohar4, M. Tacey2, K. McMillan5, T. Pham4, G. Koufogiannis6, M. Guerrieri1; 1Ringwood East, VIC/AU, 2Heidelberg, VIC/AU, 3Mornington, VIC/AU, 4Clayton, VIC/AU, 5Box Hill, VIC/AU, 6Knox, VIC/AU
DOI:
10.26044/ranzcr2021/R-0436
Purpose
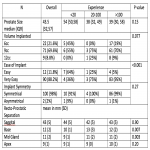
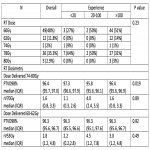
The use of rectal spacing in prostate cancer has been shown to safe and effective. The pivotal hydrogel study (1) randomised patients to rectal spacing or control achieving a mean recto-prostatic separation of 12mm versus 2mm respectively in the midplane and substantially decreasing the mean rectal volume receiving 70Gy (rV70) by 73%. This in turn significantly reduced the risk of late rectal toxicity from 9.2% to 2% (p<0.05), improving bowel quality of life at 3 years (p<0.05), reducing late grade 1 urinary incontinence from 15% to 4% (p<0.05) and almost doubling the rates of potency from 38% to 67% (p<0.05).
In this study we report the use of hyaluronic acid [HA, (Barrigel®)] as an alternative rectal spacer in patients undergoing definitive prostate cancer radiation therapy (RT). HA was in fact the first material used in rectal spacing for prostate cancer RT (2). HA has been used in cosmetic medicine over decades and has been shown to be safe. It has a simple assembly process, is highly visible on transrectal ultrasound, does not require hydrodissection, does not polymerise therefore there is no time constraint with the implant (enabling personalised sculpting of the rectal spacing to reduce the chances of asymmetrical implants at the midplane and apex of prostate) and can be reversed with hyaluronidase. These are significant advantages that make HA more user friendly and will shorten the learning curve for a new user.
In this study, we will report the feasibility, post-operative complications, recto-prostatic separation and rectal volume receiving 70Gy (rv70 if receiving 74-80Gy in 37-40 fractions) or 53Gy (rV53 if receiving 60-62Gy in 20 fractions) achieved with Barrigel® inserted into the perirectal fat before definitive prostate cancer RT. We will also compare the recto-prostatic separation and rectal volume dosimetry achieved in cohorts of patients implanted by new, competent and experienced users.