Keywords:
Lung, CT-Quantitative, Radiation therapy / Oncology, Radiotherapy techniques
Authors:
Q. Van Den Blink1, P. Ramachandran1, R. Ladwa1, A. Bernard2, M. Lehman1; 1Woolloongabba, QLD/AU, 2St Lucia, QLD/AU
DOI:
10.26044/ranzcr2021/R-0485
Methods and materials
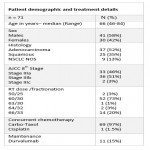
The pre-therapeutic diagnostic CT images of patients with Stage III NSCLC treated with definitive chemo-radiotherapy +/- maintenance immunotherapy were identified. The tumour volume was manually delineated as a region of interest (ROI), this included the gross tumour volume (GTV) of the primary (T) and nodal disease (N). Radiomics features such as first order, gray-level-co-occurrence matrix (GLCM), gray-level run-length matrix (GLRLM), gray-level size zone matrix (GLSZM) and neighbourhood gray-tone difference matrix (NGTDM) were extracted from the ROI. Primary outcome was any recurrence defined as local (within the ROI), nodal or distant. Secondary outcome was overall survival, analysed from the start of radiotherapy to last follow-up or death.
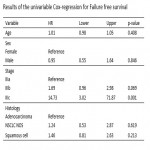
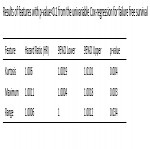
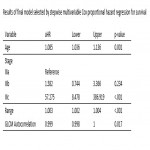
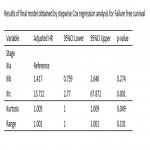
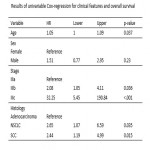
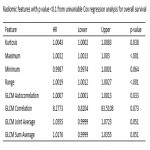
Univariate Cox Proportional hazard regression analysis was performed to identify clinical and radiomic features associated with failure and survival time. Variables with p-value<0.1 in univariable analysis were included in a stepwise multivariable Cox Proportional hazard regression analysis. Highly correlated features (correlation>0.8) were removed from the model to avoid multicollinearity.
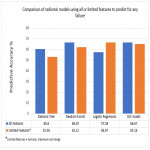
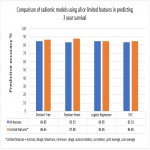
Four machine learning models were produced using all radiomics features (total of 141) and the leave-one-out cross-validation method was used to assess the predictive power of each model for failure free and 3-year survival. A comparison of the machine learning models using all features and using only features with p-value<0.1 from the univariate analysis was done to investigate whether using limited features increased the predictive accuracy of the models.