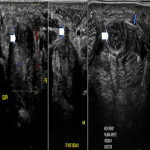
On ultrasound, nerves are more echogenic than muscles and less echogenic than tendons [3, 4]. Along a nerve’s short axis, hyperechoic connective tissue surrounds hypoechoic fascicles, giving a honeycomb appearance [4]. When entrapped, the nerve enlarges proximally to the pathology and becomes thickened and hypoechoic. There may be an ultrasonographic Tinel’s sign, i.e. paraesthesia caused by the transducer compressing the nerve. Neuropathic muscular changes may not be evident acutely; increasing muscle echogenicity may be seen within the first two weeks, with atrophy over the longer term [4].
On MRI, nerves are hypointense on T1-weighted images and isointense to hyperintense on fluid-sensitive sequences [1]. In entrapment neuropathy, the nerve enlarges proximally to the site of compression, with swelling and increased T2 signal [1]. There is abrupt flattening of the nerve’s contour at the site of entrapment [5]. Muscle changes are more easily appreciated on MRI than ultrasound, with denervation oedema seen within 48 hours and atrophy occurring over months [2]. Increased T2 signal alone may be due to the magic angle artefact, which may be avoided by positioning the extremity at less than 30° relative to B0 [6].
Overview of upper limb nerves and their entrapment syndromes:
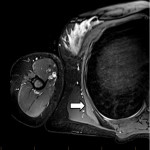
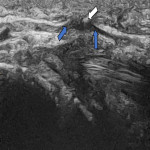
The long thoracic nerve arises from C5-C7 and runs anteriorly to the posterior scalene muscle. It then courses laterally deep to the clavicle and superficial to the first two ribs, continuing along the midaxillary line to lie on the superficial surface of the serratus anterior muscle, which it innervates [7]. Neuropathy leads to medial winging of the scapula as a result of serratus anterior weakness and unopposed rhomboid action [7]. Denervation oedema of this muscle may be noted on imaging (Figure 1). Entrapment can occur at the middle or posterior scalene muscles, second rib, or fascial sheath [7].
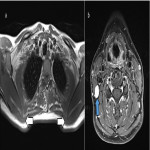
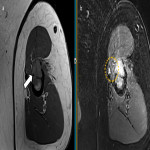
The spinal accessory nerve arises from C1-C6 and runs through the foramen magnum and across the posterior cranial fossa, before exiting the skull through the jugular foramen. It descends near the jugular vein towards the sternocleidomastoid which it innervates, and then enters the posterior triangle of the neck to supply the trapezius [8]. Entrapment can occur because of jugular foramen or posterior triangle pathology and this causes lateral scapular winging [8]. Figure 2 illustrates an example of spinal accessory nerve entrapment.
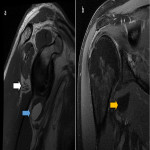
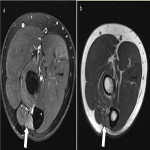
The axillary nerve arises from the posterior cord of the brachial plexus, with roots C5-C6. It exits the axilla via the quadrilateral space and gives off three branches. The anterior branch supplies the anterior portion of the deltoid. The posterior branch supplies the teres minor and posterior deltoid before continuing as the upper lateral cutaneous nerve of the arm. The articular branch supplies the anteroinferior glenohumeral joint [9]. The axillary nerve is commonly compressed in the quadrilateral space (Figure 3) [9].
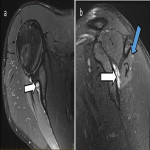
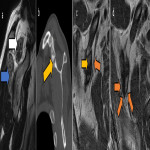
The suprascapular nerve arises in the upper trunk of the brachial plexus, with roots C5-C6. It passes through the posterior triangle of the neck and traverses the suprascapular notch to enter the supraspinous fossa where it innervates the supraspinatus muscle. It then continues through the spinoglenoid notch to the infraspinous fossa, terminating in the infraspinatus muscle which it supplies. It also provides sensory supply to the glenohumeral and acromioclavicular joints [10]. The suprascapular notch and spinoglenoid notch are common sites of entrapment [10]. Figures 4 and 5 illustrate cases of suprascapular neuropathy.
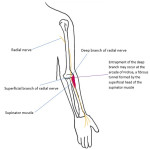
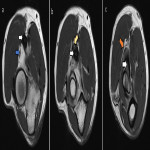
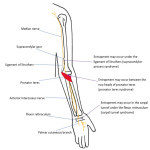
The radial nerve arises from the posterior cord of the brachial plexus, with roots C5-T1. It exits the axilla via the triangular interval and travels along the radial groove of the humerus. In the arm, the radial nerve supplies motor branches to the triceps brachii, anconeus and brachioradialis and gives three sensory branches (the posterior cutaneous nerve of the arm, the lower lateral cutaneous nerve of the arm and the posterior cutaneous nerve of the forearm). After entering the forearm through the cubital fossa, it divides into a deep motor branch and a superficial sensory branch. The deep motor branch descends in the posterior forearm and pierces the supinator to become the posterior interosseous nerve (PIN) which gives motor supply to the posterior forearm compartment muscles [11]. Entrapment commonly involves the PIN. This is most common at the arcade of Frohse (the course of the radial nerve through the arcade of Frohse is shown in Figure 6) [12]. Figures 7 and 8 illustrate different entrapment syndromes of the radial nerve. Figure 9 illustrates denervation oedema of the anconeus which indicates radial nerve pathology proximal to the bifurcation.
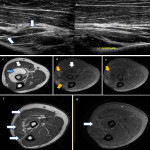
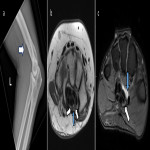
The median nerve arises from the medial and lateral cords of the brachial plexus, with roots C6-T1. It descends laterally to the brachial artery, then crosses it to sit medially halfway down the arm. It exits the cubital fossa to enter the forearm, where it travels between the flexor digitorum profundus and superficialis muscles, giving off two branches: the anterior interosseous nerve (AIN) which supplies the muscles in the deep anterior compartment, and the palmar cutaneous nerve which provides sensory innervation to the lateral palm. The median nerve then continues through the carpal tunnel and divides into the recurrent branch which supplies the thenar muscles, and the digital cutaneous branches which provide sensory supply to the lateral three-and-a-half digits on the palmar surface and motor supply to the lateral two lumbricals [13]. Common entrapment sites are the flexor retinaculum (carpal tunnel syndrome), the ligament of Struthers, and between the heads of the pronator teres (Figure 10) [14]. The AIN branch can become entrapped at the deep head of pronator teres, the fibrous arch of flexor digitorum superficialis and by muscular abnormalities (e.g. Gantzer’s muscle) [14]. Pronator quadratus oedema is considered a key feature of AIN pathology, although this can also be an idiopathic finding [15]. Cases of median nerve pathology are shown in Figures 11-13.
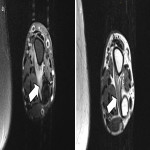
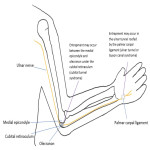
The ulnar nerve arises from the medial cord of the brachial plexus, with roots C8-T1. It enters the posterior compartment of the arm and passes through the cubital tunnel between the medial epicondyle and olecranon. In the forearm, it pierces the flexor carpi ulnaris, giving off a muscular branch (innervates the flexor carpi ulnaris and medial half of flexor digitorum profundus), palmar cutaneous branch and dorsal cutaneous branch. The ulnar nerve enters the hand via the ulnar canal (Guyon's canal), terminating in a superficial branch and deep branch (which supplies intrinsic hand muscles) [16]. Common sites of entrapment are at the cubital tunnel and ulnar canal (Figure 14). Figures 15 and 16 illustrate cases of ulnar nerve entrapment seen on MRI.
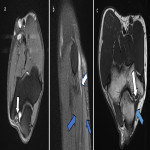
Digital nerves arise from the radial, median and ulnar nerves and may be affected by trauma (including surgical as shown in Figure 17), inflammation, vascular malformations and neoplasms [17].
The musculocutaneous nerve arises from the lateral cord of the brachial plexus, with roots C5-C7. It exits the axilla and pierces the coracobrachialis muscle, which it supplies, before descending the flexor compartment of the upper arm superficial to the brachialis and deep to the biceps brachii, innervating these muscles. It then pierces the deep fascia and courses laterally to the biceps tendon and brachioradialis, continuing into the forearm as the lateral cutaneous nerve of the forearm, which gives sensory supply to the anterolateral forearm [18]. Common sites of entrapment include the coracobrachialis muscle (Figure 18) and between the bicipital aponeurosis and brachialis fascia for the lateral cutaneous nerve of the forearm [2, 18].