Keywords:
Musculoskeletal spine, Neuroradiology brain, MR, Screening, Infection, Tropical diseases
Authors:
H. Yawary, R. Lee
DOI:
10.26044/ranzcr2022/R-0059
Methods and materials
A thirty-six-year-old male presented to an emergency department with headaches, abdominal pain, vomiting, right arm weakness and confusion. He stated he had a similar headache six months ago which resolved without intervention. His Glasgow Coma Scale (GCS) was fourteen (E4 V4 M6), but quickly deteriorated with worsening agitation to the point of requiring intubation. His inflammatory markers were normal and on initial examination he was afebrile with normal observations. He had not travelled outside of Australia in two years and had not been in contact with livestock.
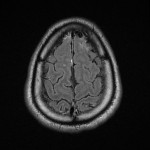
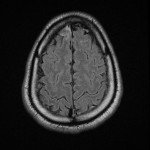
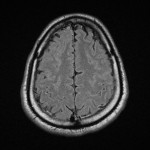
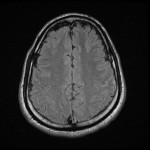
A Computerised Tomography (CT) scan of his head was done on presentation which was normal. Cerebrospinal fluid (CSF) examination showed CSF glucose 1.7 mmol/L (LOW) and Protein 3.86 g/L (HIGH). Total leucocytes 325 x 10E6/L CSF Cryptococcal Ag – negative and CSF culture and PCR showed no nuclei of bacterial or viral pathogens that commonly cause meningitis or encephalitis. He was put on broad spectrum antibiotics (Rifampicin, Isoniazid, Moxifloxacin, Pyrazinamide, Ampicillin and Pyridoxine) due to the low glucose and high protein count in the CSF being concerning for encephalitis, even without an organism being cultured. With these antibiotics he improved and was extubated, but still delirious. An MRI of the brain demonstrated subtle leptomeningeal hyperintense FLAIR and T2 signal hyperintensity in the parenchyma of the left anterior temporal pole which was suggestive of meningoencephalitis [Figure 1,2,3,4].
The patient then developed unilateral hearing loss on the left side and fevers. A repeat CSF sample confirmed brucellosis on PCR. Brucella Ab IgM and IgG returned positive in the blood samples. These findings, his clinical picture and the MRI confirming neurological involvement confirmed the diagnosis of neurobrucellosis.
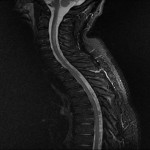
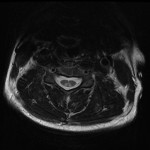
Due to the patient’s worsening symptoms, a repeat MRI brain and MRI of the spine was done. The MRI of the brain again demonstrated subtle leptomeningeal signal enhancement, but no further cause for the hearing loss was identified with his vestibules and cochlea bilaterally being normal. The MRI of the spine showed symmetrical hyperintense T2 signal bilaterally in the posterior columns of the cervical cord extending from C2-C7 [Figure 5,6]. This was noted by the consultant radiologist reporting the scan as unusual in the clinical context of neurobrucellosis. This prompted the medical team to do a full bacterial, viral, immunological, vasculitis and vitamin screen to look for possible causes beyond brucellosis which were all negative.
The patient was stepped down to oral rifampicin for 3 weeks andceftriaxone and oral doxycycline for 6 weeks. His mental state improved, however upon discharge he still had hearing loss in his left ear and a mild generalised headache. He had close follow-up arranged after discharge.