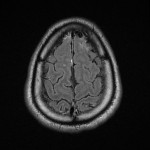
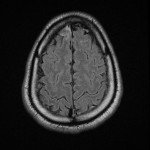
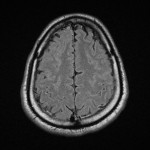
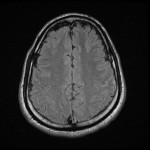
MRI findings in neurobrucellosis are broad and non-specific however, due to the nature of symptoms some patients will get an MRI of the head and spine prior to investigations for brucellosis are even considered and thus findings on MRI are important to understand. Three main articles stood out in the literature that helped classify MRI findings in neurobrucellosis.
The Istanbul-3 study (1) looked at cranial imaging findings of 263 patients in 2016. Of the 263, 143 had normal imaging. Of those who had abnormal imaging, their findings were grouped into four subcategories; a) inflammatory findings: which could include leptomeningeal involvement, basal meningeal enhancement, cranial nerve involvement, spinal nerve roots enhancement, brain abscesses, granulomas and arachnoiditis; b) White Matter involvement: with or without demyelinating lesions; c) Vascular involvement: mostly with cerebral ischaemic changes; d) Hydrocephalus/cerebral oedema. The study also noted that high levels of protein and low levels of glucose were associated with inflammatory findings on imaging analyses.
Another paper by Jiang et al. in 2018 titled ‘MRI features and categories of neurobrucellosis: A pooled review’(2) 95 cases were reviewed from 21 articles. They grouped the MRI findings into 5 categories 1) Meningitis 2) Meningoencephalitis 3) Demyelinating type 4) cases of abscess and 5) causes of pseudotumor but noted the difficulty of diagnosing neurobrucellosis on MRI findings alone.
Finally, a 2004 study by Al-Sous et al, titled ‘Neurobrucellosis: clinical and neuroimaging correlation’(3) reviewed 23 MRI images (including 17 brain and 6 spine MRI’s) and found 10 of 23 MR studies were normal (eight brain, one thoracic and one lumbar) and of those that were abnormal basal meningeal enhancement (3), lumbar nerve root enhancement (3), granuloma of the suprasellar region (1), diffuse white matter changes (7) and spinal cord atrophy (1).
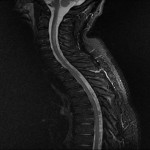
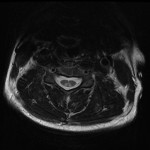
With regards to the patient reviewed in our case report, his MRI of the brain showed subtle leptomeningeal hyperintense FLAIR and T2 signal hyperintensity in the parenchyma of the left anterior temporal pole, which suggested meningoencephalitis which is in keeping with the research above, however the findings in the cervical spine are not considered a typical manifestation of neurobrucellosis. Other differentials for this are seen in HIV myelopathy and subacute combined degeneration of the spinal cord(4) with the main causes of this being Vitamin B12 deficiency, Vitamin E deficiency and copper deficiency. This patient was HIV negative and was tested twice during admission, he also did not have pernicious anaemia, his copper level was 19.1 umol/L, his Vitamin E level was 50 umol/L, his Vitamin B12 level was 281 pmol/L and his Folate level was 13.9nmol/L which were all within normal limits. These findings may also be seen in neurosyphilis, however again the patient was tested negative for syphilis and there was no abnormal enhancement of the vestibulocochlear nerves, cochlea or vestibular apparatus to further support the diagnosis of otosyphilis. On further review of the literature, a case study on brucellosis causing longitudinally extensive myelitis in the C-spine was noted from 2019(5), and again they noted that vitamin, bacterial screening, vasculitis panel, viral and tuberculosis screening were all negative, raising suspicion that this may be a new finding on MRI for neurobrucellosis.