Case/Imaging Findings:
The included case example pertains to a 16-year-old female presenting with acute haemorrhage into a congenital duodenal duplication cyst within the second part of the duodenum (D2) following minor trauma. She presented with mild right sided abdominal pain, nausea but was afebrile without features of peritonism. Initial workup included a white blood cell count of 7.2 x109/L (normal range 4.5 x109/L to 13.0 x109/L), lipase of 93 U/L (normal range <90 U/L), haemoglobin of 102g/L (normal range 120g/L to 160g/L), total bilirubin of 25 umol/L (normal range <20 umol/L). Management was initially conservative followed by interval resection of the duplication cyst, allowing histological confirmation of the diagnosis.
Multiple imaging modalities were utilised as part of the diagnostic work-up and intra-operative management of this case. Key imaging findings across the various modalities are described below.
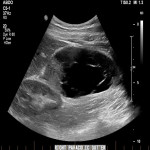
Image 1:
Ultrasound demonstrates a complex cystic structure with internal septations in the right upper quadrant between the inferior hepatic margin and the right kidney. Posterior acoustic enhancement confirms internal fluid content, consistent with a cystic structure.
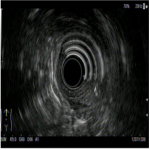
Image 2:
Endoscopic ultrasound demonstrating a collapsed cystic structure with duplicated layers of duodenal wall showcasing the classical ‘gut signature’ of a duodenal duplication cyst. Gut signature refers to the layered pattern of the wall, with the hyperechoic inner layer representing the submucosa and the hypoechoic outer layer representing the smooth muscle(3)
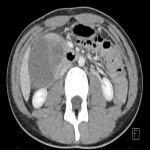
Image 3:
Axial contrast enhanced CT in the portal venous phase of enhancement demonstrates a large complex cystic mass extending from the lateral border of the D2 segment of the duodenum. The mass contains heterogenous attenuation material consistent with a mixture of cystic fluid and blood products.
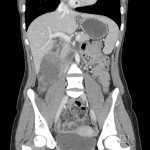
Image 4:
Coronal CT demonstrates a large cystic structure in the right upper quadrant indistinguishable from duodenum and distal common bile duct, containing predominantly fluid attenuation material, with some suspected internal haemorrhage. There is no internal gas to suggest direct communication with the duodenal lumen. Fluid distension of the stomach is suggestive of a degree of associated gastric outlet obstruction.
Image 5:
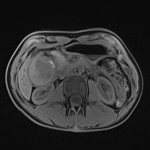
MRI axial T1-weighted Dixon fat saturated image demonstrates a large cystic mass compressing and medially displacing the D2 segment of the duodenum. Foci of high T1 signal on the anteromedial aspect are consistent with blood products.
Image 6:
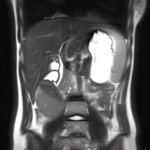
Coronal T2-weighted HASTE image demonstrates heterogeneous signal material within the cystic lesion, with a thick peripheral capsule. More complex T2 hypointense material at the superior medial aspect of the lesion is suggest of blood products. Proximal to the lesion, there is distension of the second part of the duodenum and borderline common bile duct dilatation secondary to extrinsic compression at the ampulla of Vater.
Image 7:
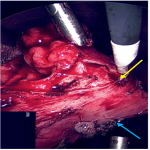
Intraoperative photograph of the D2 duplication cyst highlighting the duplicate cyst layer. The duplicate cyst layer was visualised upon opening the duodenal serosa. The cyst cavity can be seen between the outer serosal layer (being incised with the diathermy hook) and inner mucosal layer (adjacent to the suction tip).