Conventional SIRT
Infusion of radioactive substances, typically 90Y resin or glass microspheres, into the hepatic artery to selectively target liver tumours forms the basis of radioembolisation.
The 3 landmark RCTs based on 90Y resin spheres mainly used an older dosimetry technique:
- SARAH - Body Surface Area (BSA) dosimetry method and both lobar and segmental delivery [8].
- SIRveNIB - Mix of BSA and partition dosimetry [9].
- SORAMIC - BSA and lobar delivery [10].
- Another older dosimetry approach is the Medical Internal Radiation Dosimetry (MIRD) method for glass microspheres [11].
- There has been a more recent shift towards personalised dosimetry based on partition dosimetry whereby treatment dosimetry is based on the tumour to normal liver (T:N) ratio, determined from a Technetium-99m (99mTc) macroaggregated albumin (MAA) SPECT-CT mapping and planning study which is performed prior to SIRT treatment [12]. Tracer distribution and hepatopulmonary shunting are also assessed as excessive lung shunting or extrahepatic uptake are relative contraindications to SIRT [13].
- Although dosimetry is individualised to the patient (therapeutic or palliative treatment), the aim is to deliver the maximum safe dose to the tumour whilst sparing the lung (<30 Gy) and normal liver parenchyma (<70Gy) [14].
There are two main technical approaches to radioembolisation:
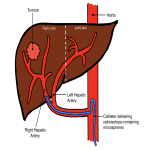
- Lobar infusion of the tumouricidal dose [Fig 1]
Advantages: Suitable for multiple tumours in one lobe and is a technically simpler procedure, not requiring superselective arterial catherterisation.
Disadvantages: Tumour dose is constrained by dose to non-tumour liver and/or lung shunt, may or may not reach tumouricidal dose.
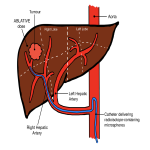
- Segmental infusion of the tumouricidal dose [Fig 2]
Technical Refinements
Recent refinements in radioembolisation technique and patient selection have allowed more ‘ablative’ level radiation delivery via radiation lobectomy (RL) and radiation segmentectomy (RS) in addition to personalised dosimetry, allowing delivery of higher radiation doses (eg. ≥205Gy) to tumour(s).
Radiation Lobectomy
- Modification of lobar approach using an ablative dose (induces liver injury to the normal liver parenchyma), and has been used as a definitive treatment in large, unresectable tumours or as a surgical neoadjuvant to permit[15-17]:
1) Bridging to liver resection or transplant.
2) A biologic test of time (particularly for candidates being downstaged to transplant).
3) Induction of future liver remnant hypertrophy to permit safe liver resection.
Radiation Segmentectomy
- RS SIRT utilises the single-vessel perfusion of the eight portal Couinaud segments to selectively deliver the radioisotope, enabling the delivery of an ablative 90Y dose to an individual liver segment as definitive treatment for unsuitable surgical candidates [18-20].
Efficacy
Early-stage HCC
- Despite the initial landmark trials (SARAH, SIRveNIB and SORAMIC [8-10]) failing to demonstrate survival benefit with SIRT for HCC treatment compared with sorafenib, there was a clear and profound benefit in secondary analysis for the SARAH subgroup receiving tumour dose >100Gy showing that tumour dose delivery is crucial [21].
- Furthermore, subgroup analysis of the SORAMIC trial found the importance of focusing on treatment of patients at earlier Child-Pugh scores with limitation of liver dysfunction demonstrating survival gains [22].
- The retrospective, single-arm, LEGACY study included patients with a solitary lesion <8cm treated with glass microspheres and reported an objective response rate (ORR) of 88.3% with median overall survival (OS) of 57.9 months [23].
- A durable response rate was seen with 62.2% exhibiting a duration of response (DoR) ≥6 months [23].
- 61.7% of tumours treated were under 3cm and only 5.6% were between 5-8cm, response rates or survival outcomes in relation to tumour size were not reported [23].
Ablative SIRT and personalised dosimetry
- Prospective evaluation of refined dosimetry carried out in the multicentre DOSISPHERE-01 trial identified improved OS rates when compared to earlier trial data especially within the personalised dosimetry arm: Median OS 26.6 months (Personalised: ≥205Gy to the tumour) vs 10.7 months (Standard: 120±20Gy to the affected lobe) [24].
- Similarly, median PFS almost doubled in the personalised dosimetry arm: PFS 6 months (Personalised) vs 3.4 months (Standard) [24].
- This survival benefit is in keeping with the significantly improved overall response rate (ORR) of 79% with ≥205Gy dose delivery to the index lesion [24].
- The TARGET study confirmed these findings, reporting an increase in median OS with higher radiation dose delivery: Median OS 36.7 months (≥300Gy), 25.1 months (≥200 to <300Gy), 16.1 months (<200Gy) [25].