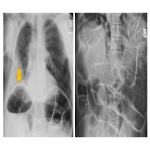
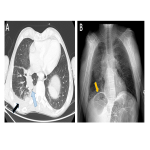
24 hours after admission the patient developed increasingly severe right upper quadrant pain, associated with nausea and vomiting. Examination findings included abdominal distension and reduced bowel sounds. Chest and abdominal x-rays at this time (Day 3) demonstrated extensive dilated small bowel, with relative paucity of colonic gas suggestive of small bowel obstruction.
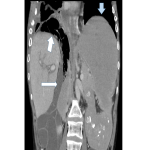
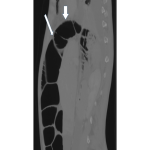
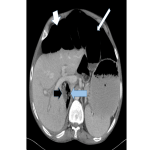
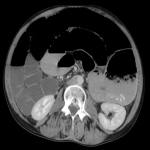
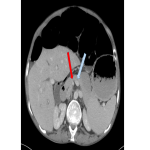
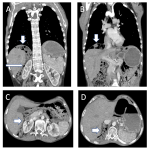
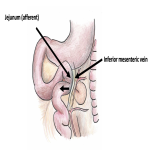
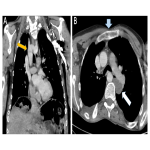
Subsequent CT abdomen and pelvis post IV contrast later that day demonstrated distended oesophagus and stomach, and dilated jejunum and ileum. The cause of the small bowel obstruction was confirmed to be unusual herniation of ileocaecum into a potential space posterosuperior to the liver, limited superiorly by the right hemi-diaphragm and anteriorly by the coronary ligament.
The aperture through which the hernia occurred was lateral to the compressed hepatic segment of the inferior vena cava and second part of the duodenum, anterior to the right adrenal gland and kidney, and posterior to the small caudate lobe and portal vein.
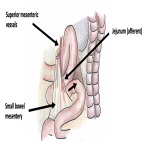
There were no specific features of intestinal ischaemia. The extraperitoneal bare area of the liver appeared small, with inferior liver visceroptosis and laxity of coronary suspensory ligaments. Additionally, there was abnormal rotation of the small bowel mesentery, with reversed relationship of the superior mesenteric vein to artery.
The patient was successfully managed with non-operative supportive measures. CT abdomen and pelvis prior to discharge (Day 10) demonstrated resolution of the hernia; the caecum subhepatic in location. Progress imaging at 3 months again demonstrated interposition of ileocaecum between the liver and right hemidiaphragm via the same internal hernial orifice, this time without evidence of bowel obstruction.
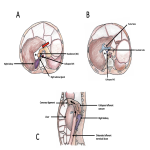
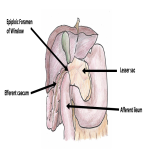
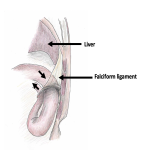
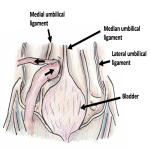
This hernia is unique in that it featured an intraperitoneal space with extension into the location of the (normally present) bare area of the liver, limited anteriorly by the superior and inferior leaves of the coronary ligament (reflections of peritoneum from the diaphragm onto the posterosuperior surface of the liver, normally forming the boundaries of the bare area). In this case the bare area was likely rudimentary, due to thinning and distensibility of the coronary ligaments.
Hypotonic visceroptosis was likely also a potential factor. Visceroptosis is sinking of abdominal organs below their normal anatomical position, associated with connective tissue disorders including Ehlers-Danlos syndrome and commonly thought secondary to relaxation of visceral ligaments [8]. Visceroptosis (specifically liver) is a known clinical manifestation of SGBS [3].
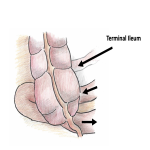
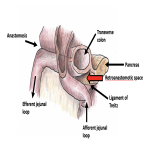
In addition to distensibility of the coronary ligament, there was persistence of a right mesocolon, caused by embryological failure of fusion of the mesocolon to the peritoneum of the posterior abdominal wall. Persistence of long congenital right mesocolon has an incidence of 4% and can predispose to Foramen of Winslow hernia [9]. We postulate that persistent right mesocolon in this case allowed the mobile caecum to flip superiorly within the abdominal cavity to pass though the right paracaval hernial orifice. The abnormal rotation of the small bowel mesentery likely also contributed to ileocaecal mobility. 'Caecal bascule’ describes the anterior and superomedial folding of the caecum with absence of an axial ‘twisting’ component [10]. This term however is usually reserved for cases of caecal volvulus, and although the caecum underwent this displacement, the obstuction (evidenced by ileocaecal closed loop calibre transition) was due to constriction at the internal opening of the paracaval hernia, rather than the effect of folding or twisting.
This hernia can be distinguished from Foramen of Winslow Hernia in its relation to the portal vein - in this case ileocaecum passed posterolateral to the portal vein rather than posteromedial, and remained right lateral to the IVC and duodenum.
This hernia shares similarities with a case described in the ultrasound literature of ileocaecal herniation through a defect above the superior pole of the right kidney within Morison’s pouch [11], however in the case we describe, the ileocaecum continued to pass more cranially, to the subdiaphragmatic blind end of the pouch posterosuperior to the liver.