Type:
Educational Exhibit
Keywords:
Anatomy, Head and neck, CT, MR, Biopsy, Radiation therapy / Oncology, Surgery, Education and training
Authors:
A. Abeysekera, J. Gillespie
DOI:
10.26044/ranzcr2022/R-0189
Imaging findings OR Procedure details
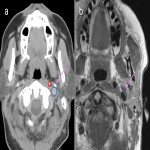
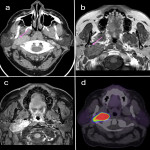
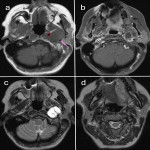
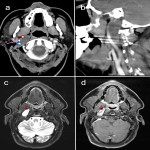
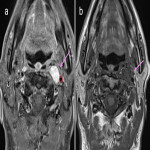
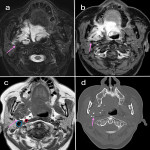
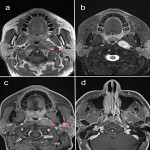
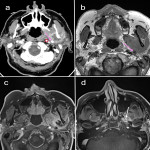
When reporting on a lesion in the suprahyoid neck, it is important to determine the space of origin. This helps to narrow the possible differential diagnosis depending on the structures present within that space (3). The displacement of the parapharyngeal fat space is one well described method used to do this. However, the effect of the lesion on the styloid process and carotid sheath vessels are other helpful clues to look for. The styloid process is a therefore a useful landmark to review.
The styloid process and musculature are easily demonstrated on CT but may be somewhat difficult to localise on MRI. It is often easiest to find the stylomastoid foramen and then follow the styloid process and muscles inferiorly from here. On MRI the cortex of the styloid process will be low signal intensity on both T1 and T2. Depending on the amount of bone marrow within the styloid, it may demonstrate central T1 hyperintensity.
The stylomandibular tunnel is the space between the ramus of the mandible anteriorly and the styloid process and ligament posteriorly. Lesions arising from the parotid space often widen the stylomandibular tunnel (4). Whereas lesions arising from the carotid (post-styloid PPS) may cause narrowing of the tunnel as the styloid process is displaced anteriorly.
The true PPS (pre-styloid) contains fat and the ascending pharyngeal neurovascular bundle with potential minor salivary glands. The mandibular branch of the trigeminal nerve (V3) is positioned medially within the masticator space but is an important relation. Inferiorly, the PPS is contiguous with the submandibular space. Lesions arising from this space include salivary gland neoplasms, developmental lesions (such as venolymphatic malformations) and lymphadenopathy. Often pathologies will arise from another space and extend into the PPS. Lesions in the PPS tend to displace the internal carotid artery (ICA) and internal jugular vein (IJV) posteriorly.
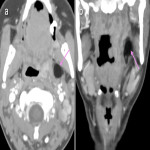
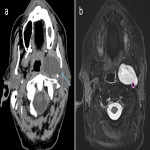
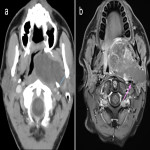
The post-styloid PPS (carotid space) contains lymph nodes, sympathetic ganglia, cranial nerves IX-XII, ICA and IJV. Lesions arising in this space include lymphadenopathy, nerve sheath tumours, paragangliomas and vascular lesions. In the carotid space, the direction of vascular displacement may assist with tumour localisation. The vagus nerve is positioned between the ICA and IJV and therefore tumours arising from the vagus nerve may cause splaying of the vessels (5). The hypoglossal nerve is more posteriorly located and therefore may cause anterior displacement of the ICA. The sympathetic chain is medially located and does not tend to cause splaying of the vessels. However, lesions arising from the sympathetic chain may cause anterior displacement of the ICA. The retropharyngeal space is just medial to the carotid space and therefore a retropharyngeal lymph node may be mistaken as arising from the carotid space. The presence of fat between the ICA and retropharyngeal node is a clue.
Figures 1-11 demonstrate a series of lesions in and around the post-styloid parapharyngeal space and the clues to determine the space of origin of the lesion.