Type:
Educational Exhibit
Keywords:
Musculoskeletal soft tissue, Oncology, MR, Imaging sequences, Neoplasia
Authors:
K. Motupally, K. Singh, P. Jeremic
DOI:
10.26044/ranzcr2022/R-0232
Learning objectives
We introduce two patients who share the common diagnosis of axillary musculoskeletal fibromatosis. We explore the initial presentation, circumstances leading to diagnosis, imaging characteristics and treatment options. Desmoid tumours are rare indolent proliferative masses which may initially appear as aggressive lesions. Multisequential MRI imaging plays a vital role in diagnosis. There is no current accepted clinical guideline for treatment [1, 6].
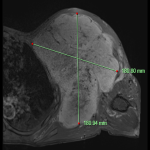
Patient One: A 33-year-old female was referred to the orthopaedic outpatient clinic after gradually increasing left shoulder pain, reduced strength, and function over 10 months. An x-ray and ultrasound of the affected joint demonstrated widening of the acromioclavicular joint and subdeltoid bursitis. MRI of the left shoulder showed a hypointense T1 and hyperintense T2 signal soft tissue lesion with diffuse contrast enhancement involving the bicipital groove and surrounding biceps tendon [Fig 1-6]. Biopsy of the left shoulder lesion had histopathological features of an extra-abdominal fibromatosis or desmoid tumour. This case was discussed at a multidisciplinary meeting where wide surgical excision was recommended. The patient declined this recommendation due to cost and the risk of affecting function or requiring a left upper limb amputation; they returned to their home country and received treatment regime including a tyrosine kinase inhibitor over 4 years which resulted in resolution of their symptoms. They were re-referred to the orthopaedic outpatient clinic by their general practitioner due to increasing pain in the left shoulder. Interval imaging four years later demonstrated two discrete foci with diffuse contrast enhancement affecting the proximal biceps brachii and the axillary region [Fig 7-12]. The lesion affecting the biceps brachii was stable in appearance. The axillary lesion encased the axillary neurovascular bundle with the lesion surrounding the biceps tendon no longer demonstrating post contrast enhancement indicating a treated quiescent disease [Fig 7]. Due to the risks of surgery and lack of clear treatment guidelines, and shared decision making, the patient opted for close monitoring with surveillance imaging. The most recent imaging shows a stable left axillary mass with the bulk of the mass showing fibrotic change in keeping with treatment response [Fig 13-18].
Patient Two: A 65 year old male was referred to the general surgical outpatient clinic for management of a left axillary swelling during routine surveillance of a left upper medial humeral growth present for 10 years. The patient had MRI imaging of the known humeral growth which was suspected to be a non-aggressive type periosteal chondroma or an atypical chondroma. Due to new asymptomatic but progressively increasing swelling in the left axilla an ultrasound was performed demonstrating a 3 x 2 x 1cm indeterminate vascular lesion. An ultrasound guided fine need aspirate was suggestive of a spindle cell neoplasm. A core biopsy was then performed with histopathology suggestive of fibromatosis. Initial MRI imaging showed a hypointense T1, hyperintense T2 and avid post-contrast 2.5 x 8cm (TS, CC) lesion in the medial left axilla with diffusion restriction [Fig 19-24]. Thereafter, the patient was discussed at a soft tissue multidisciplinary team meeting who recommended continued observation of the lesion. Interval MRI imaging one year later showed enlargement of the T1 isointense, T2 hyperintense lesion with avid enhancement, now measuring 7 x 5.5 x 13cm (TS, AP, CC) with ill-defined medial and posterior margins raising concern for malignant transformation. The patient had PET imaging demonstrating mild heterogenous FDG avidity [Fig 25]. He was trialled on tamoxifen and sulindac with no response as the patient declined surgery due to risk of loss of function. Subsequent CT imaging showed interval increase lesion displacing the axillary artery along the posterior lateral extent of the mass with no vascular involvement, no invasion of the left chest wall or into the left thorax prior and no enhancement with contrast [Fig 26]. Further soft tissue MDT discussion recommended resection and adjuvant radiotherapy. Pre-operative MRI showed interval change with the axillary lesion increasing in size and measuring 18 x 18 x 25 cm (TS, AP, CC). Although not visualised, it was presumed the lesion was likely encasing the brachial plexus and demonstrated to be partially encasing the axillary and subclavian vessels [Fig 27-29]. The patient underwent radical axillary dissection with some degree of tumour remaining in the brachial plexus and has planned to undergo radiation therapy [Fig 30].
Neither of these patients had syndromic association with desmoid tumour on further evaluation of clinical history and examination.

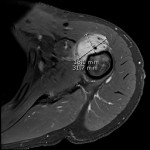
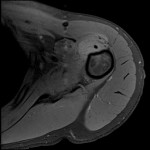
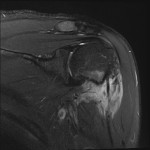
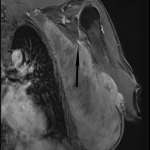
![Fig 7: Desmoid tumour with avid hyperintensity compared to muscle on axial T2 weighted Dixon imaging. It completely encases the axillary neurovascular bundle. The disease previously affecting biceps tendon [Fig 1-6] is present and demonstrates no post-contrast enhancement which is consistent with treated or quiescent disease.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921835?maxheight=150&maxwidth=150)
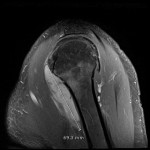
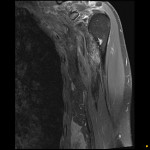
![Fig 8: Desmid tumour previously seen [Fig 7] with avid post contrast enhancement on sagittal T1 weighted Dixon imaging. It extends superiorly to involve the insertion of the pectoralis minor muscle.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921836?maxheight=150&maxwidth=150)
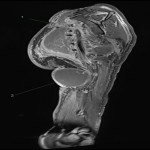
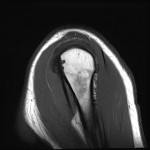
![Fig 9: Two discrete foci with avid post contrast enhancement affecting the axillary region and the proximal biceps brachii on coronal T1 fat suppressed imaging. The disease previously surrounding the biceps tendon [Fig 1-6] again demonstrates no post-contrast enhancement.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921837?maxheight=150&maxwidth=150)
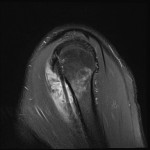
![Fig 10: Avid post contrast enhancement on axial T1 weighted Dixon imaging of the desmoid tumour. It encases the axillary neurovascular bundle. The disease previously surrounding the biceps tendon [Fig 1-6] demonstrates no post-contrast enhancement.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921838?maxheight=150&maxwidth=150)
![Fig 11: Two discrete isointense foci previously seen [Fig 9] in the axillary and proximal biceps region on coronal T1 imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921839?maxheight=150&maxwidth=150)
![Fig 12: Two discrete hyperintense foci previously seen [Fig 9] in the axillary and proximal biceps region on coronal T2 imaging. The disease previously surrounding the biceps tendon [Fig 1-6] is hypointense.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921840?maxheight=150&maxwidth=150)
![Fig 13: Axillary lesion as previously seen [Fig 7-12] encasing the axillary neurovascular bundle without post contrast enhancement on axial T1 fat suppressed imaging suggestive of treated or quiescent disease. The lesion demonstrates the ‘fascial tail sign’ (arrow) as it is medially bound by the lateral thoracic wall.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921841?maxheight=150&maxwidth=150)
![Fig 14: Hypointense axillary lesion as previously seen [Fig 7-12] encasing the axillary neurovascular bundle on axial T1 fat suppressed imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921842?maxheight=150&maxwidth=150)
![Fig 15: Hypointense axillary lesion as previously seen [Fig 7-12] encasing the axillary neurovascular bundle on axial T2 fat suppressed imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921843?maxheight=150&maxwidth=150)
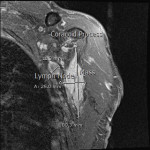
![Fig 17: Two hypointense foci (arrows) as previously seen [Fig 11] in comparison to muscle on coronal T1 imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921845?maxheight=150&maxwidth=150)
![Fig 18: Two hypointense foci (arrows) as previously seen [Fig 12] in comparison to muscle on coronal T2 imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921846?maxheight=150&maxwidth=150)
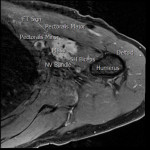
![Fig 21: Hyperintense mass on axial T2 weighted fat suppressed imaging. Surrounding structures as labelled. [SH Biceps = short head of biceps muscle] [NV bundle = neurovascular bundle]](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921858?maxheight=150&maxwidth=150)
![Fig 22: Hyperintense mass as previously seen [Fig 19] on coronal T2 weighted fat suppressed imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921859?maxheight=150&maxwidth=150)
![Fig 23: Isointense mass relative to surrounding skeletal muscle as previously seen [Fig 19] on T1 coronal imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921860?maxheight=150&maxwidth=150)
![Fig 24: Mass as previously seen [Fig 20-21] with diffusion restriction on axial DWI ADC imaging.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921861?maxheight=150&maxwidth=150)
![Fig 25: Mild heterogenous FDG-avid left subpectoral axillary mass as previously seen [Fig 19-24] on axial 18F-FDG PET-CT.](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921862?maxheight=150&maxwidth=150)
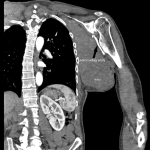
![Fig 27: Avid post contrast enhancement of known left axillary mass with interval increase in craniocaudal measurement now measuring 25cm on coronal T1 fat suppressed Dixon imaging in comparison to prior imaging [Fig 19]](https://epos.myesr.org/posterimage/ranzcr/ranzcr2022/161033/media/921865?maxheight=150&maxwidth=150)