TYPES OF ARTEFACTS:
Chemical shift phenomenon; artefacts due to intrinsic signal of imaged structures
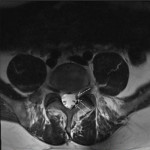
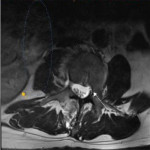
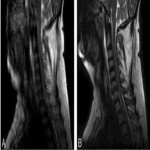
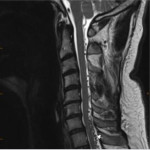
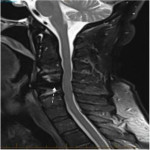
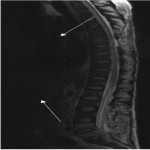
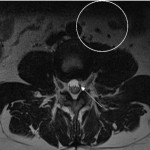
The chemical shift phenomenon is also known as “misregistration” or “mismapping”. It occurs due to the slower resonating frequency of protons in fat compared to water which results in an artefactual shift in signal intensity along the fat-water interfaces [2]. This is more prominent with at higher magnetic field strength and narrower bandwidth [3]. In spinal MRI, this can be seen as alternating bright and dark outlines at the sides of vertebral bodies. These artefacts can also be seen around lipomatous and cystic lesions in the spine, such as a lipoma [2, 3]. These may mimic disc bulge, as shown in Figure 1, and can exaggerate foraminal narrowing as the discovertebral junction is a fat-water interface. The India ink artefact is a type of chemical shift phenomenon seen on gradient echo sequences. It manifests as a black boundary at the fat-water interface (seen in Figure 2) [4]. Chemical shift artefact can be eliminated by using a fat-suppressed sequences. A smaller field of view and wider bandwidth can also reduce this artefact [3], but this comes at the cost of image resolution (Figure 3).
Artefacts due to motion
Motion artefacts can occur due to the patient changing position during scan acquisition. In addition, “ghost” artefacts can occur from periodic motion such as blood flow, cerebrospinal fluid (CSF) pulsation and swallowing [5].
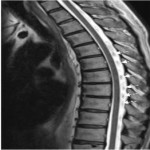
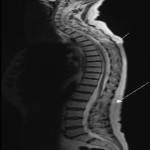
Artefacts due to patient movement (Figures 4-6) occur in the phase-encoding direction as this step usually take the longest and is acquired line by line, and can lead to blurring or ghosting of structures [5].
The signal of the structure is displayed over its range of motion, resulting in blurring and decreased edge definition [5]. The study may be rendered non-diagnostic (Figure 4).
Artefacts due to flowing blood are most commonly seen as a loss of signal in the blood vessels (flow voids) that occur due to the blood moving out of the imaged volume before scan acquisition (shown in Figure 5) [2, 5].
When flow voids are present in the spinal canal, it may denote the presence of high-flow within the spinal canal, such as in vascular tumours or malformations such as arteriovenous fistulas.
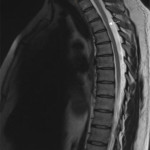
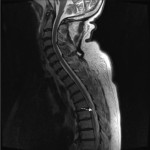
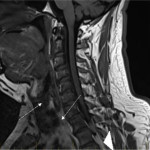
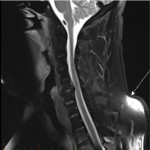
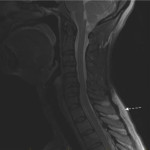
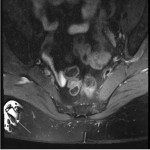
Artefacts due to CSF pulsation are more often seen in the cervical and thoracic spine compared to the lumbar spine. These artefacts appear as signal heterogeneity within the thecal sac voids, with focal areas of signal loss in the CSF (shown in Figure 7). This can be mistaken for a dural arteriovenous fistula, although the latter has a characteristic serpiginous appearance (Figure 8) [6]. This is a useful artefact as its absence in the context of spinal cord deviation can indicate an arachnoid cyst (Figure 9) [5]. On the contrary, if there is cord deviation with preserved CSF pulsation artefact, ventral dural herniation or arachnoid web will be more likely (shown in Figure 10).
Artefacts due to swallowing (Figure 11) or similar movements involving the cervical spine can cause a series of ghost images that can obscure the spinal cord and possibly diminish its size. Repeating the study and applying a presaturation pulse will reduce this artefact [2].
Artefacts due to a non-uniform magnetic field
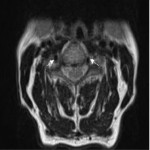
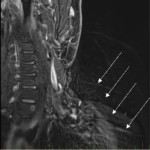
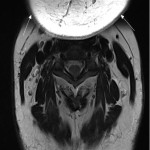
Failure of fat suppression artefacts (Figures 12 and 13) commonly occur. Frequency-selective presaturation is the most common method of eliminating unwanted signal from fat. Inhomogeneity in the static magnetic field can cause this to fail, usually occurring when there is a large field of view [2, 7]. In this situation, the fat in vertebrae may not be suppressed at the edge of the scan field, leading to abnormal bright signal in areas where fat should have been saturated and fat signal nulled. In this area, water may be saturated instead of fat, causing signal loss from the spinal cord which can simulate or obscure pathology [2, 8]. This artefact is particularly severe at the back of the neck, especially at the cervicothoracic junction, due to the geometry of the fat-air interface at this site [2].
Metallic susceptibility artefacts are caused by the large magnetic susceptibility of various para- or ferro- material. These usually present as a signal void associated with peripheral signal hyperintensity (Figure 14). Ferromagnetic artefact is greater with gradient echo imaging than it is with both conventional and fast spin echo imaging. It is worse with reduced bandwidth, large voxel sizes and high field strength magnets [8]. Metal artefacts may be misinterpreted as hypertrophic bone formation or spinal stenosis because both bone and metal have low signal intensity with all MR imaging sequences [9, 10]. Common devices that can produce magnetic susceptibility artefacts are spinal fixation rods, shrapnel or inferior vena cava filters [8]. Nonmagnetic stainless steel can also cause artefacts on MR images because the material has residual paramagnetic properties [11]. Titanium implants are associated with less surrounding tissue distortion artefacts compared to stainless steel [12].
Artefacts due to scanning parameters
The shading artefact (Figure 15) is due to a nonuniform radiofrequency field produced by a surface coil, and this causes the signal intensity of the image to be uneven, with loss of signal intensity in parts of the image further from the surface coil, which can potentially render the study non-diagnostic [2].
Saturation artefact (Cross talk/coherence) may occur when angled axial images of the lumbar spine are obtained simultaneously. A band of signal loss will be present where they overlap due to signal interference. This is represented as a series of linear areas of decreased signal intensity overlying the paraspinal soft tissues, which can potentially obscure intraspinal lesions [5, 8].
Wrap-around artefact (aliasing) (Figures 16 and 17) results when signal from tissue outside the field of view is mapped [13]. The signal received is misplaced onto the opposite side of the image. This can potentially obscure lesions of the spine and adjacent tissues [2, 5, 8].
Truncation artefact (Gibbs Phenomenon) (shown in Figure 2) occurs due to the inability of Fourier transformation to reproduce signal intensity changes at high contrast interfaces accurately, for example at the discovertebral junction and CSF-cord interface. This artefact appears as a series of parallel lines that propagate from both sides of a high-contrast interface and diminish in amplitude with increasing distance from the interface. Truncation artefact can be mistaken for several pathologies, including a dilated central canal, syrinx, arteriovenous malformation or myelitis. Truncation artefact may also make areas of very high or low signal intensity appear larger than they actually are. Thus, areas of CSF or bone may appear enlarged and this can be misinterpreted as pathological change such as cord atrophy [2, 5, 8].
Partial volume averaging occurs when structures with different signal intensities are included within the same voxel, leading to an averaging of signal intensity within the voxel (Fig 11). This is more prominent with thick sections and/or small structures. If there is a large difference in signal strength between tissues in adjacent voxels, areas of high signal intensity can “bleed” into areas of low signals. This makes bright structures appear larger [2, 5, 8].
The dielectric effect (Figures 18 and 19) is seen when using higher magnetic field strengths, typically 3T or more, and occurs when the radiofrequency wavelength is of similar magnitude or smaller than the patient’s cross-sectional diameter, leading to constructive and destructive interference patterns and hence, areas of increased or decreased signal intensity. At a field strength of 3T, the radiofrequency wavelength is 26 centimetres which may be smaller than the abdominal diameter, particularly in patients with obesity, ascites or pregnancy. Central decreased intensity can obscure pathology [14].