Keywords:
Genital / Reproductive system female, Oncology, CT-Quantitative, Radiation therapy / Oncology, Demineralisation-Bone, Toxicity
Authors:
C. Godber, C. Clark, T. Diamond, R. Rahbari
DOI:
10.26044/ranzcr2023/C-154
Purpose
Loss of bone mineral density (BMD) and pelvic insufficiency fractures (PIF) are well-documented complications of external beam radiotherapy for gynaecological malignancies and contribute to significant post-treatment morbidity and mortality1,2. Recent prospective studies and metanalyses report the prevalence of PIFs post radiotherapy as 7.8%-14% with most occurring within 2 years post treatment2–4. Currently no consensus guideline exists for the risk stratification of these patients and as such it remains an area in need of further research5. This study will aim to provide a preliminary understanding of the treatment factors related to this complication to guide further prospective research on the subject.
The underlying pathogenesis of radiation induced bone loss is likely due to multiple factors including microvascular occlusion and impaired osteoblast function6,7. It has been hypothesised that radiation decreases the number of active osteoblasts by arresting the cell cycle and sensitising them to apoptosis8. There are further studies suggesting radiotherapy may induce osteoclast activity but this remains debated and poorly understood8,9. Anti-resorptive therapy such as bisphosphonates has occasionally been used to prevent radiation induced bone loss however there is no definitive evidence of its efficacy 9. A Cochrane Review in 2018 investigated the evidence of pharmacological interventions preventing radiation induced bone loss and found that the evidence in this area was of low quality, highlighting the need for an improved understanding of this complication5.
While various patient related risk factors for radiation induced bone loss have been identified (age, pre-existing osteoporosis, menopausal status, smoking status etc.), there is limited evidence on the specific treatment related factors contributing to PIF risk and bone loss. Small studies have demonstrated increased rates of BMD loss and PIF in areas receiving higher radiotherapy doses10. Treatment volume and field size has generally been considered as a relevant treatment factor, however recent studies have suggested that BMD loss may be just as pronounced in regions immediately outside the treatment field where planned dose is zero or negligible11. Non-radiotherapy treatment related risk factors include concurrent or prior chemotherapy and high dose steroids, all of which have a direct impact on bone remodelling12.
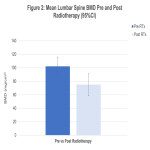
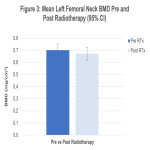
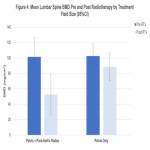
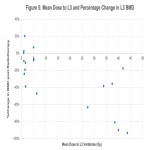
This retrospective study will aim to further understand the radiotherapy treatment related factors for bone loss in patients undergoing pelvic radiotherapy for gynaecological malignancies. The aims of this study are to evaluate whether there is bone loss associated with radiotherapy, whether the bone loss is most pronounced within the treatment field compared to outside the treatment field and whether the degree of bone loss is correlated with time from RT. This will guide further research in the area, ideally prospective studies or research investigating risk stratification and management of these patients.