Type:
Educational Exhibit
Keywords:
Abdomen, Genital / Reproductive system male, Ultrasound, Ultrasound-Colour Doppler, Other, Inflammation
Authors:
A. Lanyon, B. Di Muzio, N. Khominsky
DOI:
10.26044/ranzcr2023/C-280
Imaging findings OR Procedure details
Epididymo-orchitis (EO) is the most common cause of acute scrotal pain (1). The incidence of EO in the United kingdom outpatient population is approximately 2.45 per 1000 men (2). Testicular infarction following EO is known albeit rare complication, with only a handful of case reports available. One centre in the USA reported a prevalence of 1.3% (6/462) over a 10 year period. Non-resolving infection despite appropriate antibiotic therapy, worsening of acute scrotal pain, recurrent EO, and abscess development likely contribute to a poorer prognosis (3). In our cases, the average duration of symptoms before infarction ranged between 4 and 19 days(19, 8, 4).
Pathophysiology behind testicular infarct as a result of EO remains unclear. Theories suggest epididymal oedema may compress testicular veins resulting in venous congestion with the addition of bacterial endotoxins promoting a venous thrombosis (4).
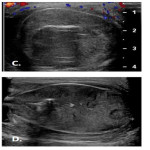
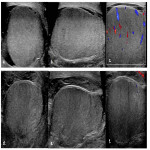
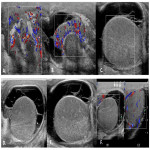
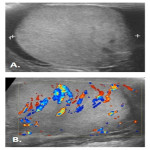
Doppler US of the scrotum is the gold standard for diagnosing acute testicular infarct and distinguishing it from other acute scrotal pathologies including non-complicated EO, torsion, and solid/cystic scrotal masses. On greyscale imaging, homogeneous echotexture is less associated with a non-viable testis than a heterogeneous testis. Colour doppler assesses for perfusion, with those with non-complicated EO demonstrating characteristic increased flow to epididymis and tests. When infarction occurs, it can manifest as focal wedge-shaped areas or, most commonly, as global swollen and avascular testis. Rarely a juxta-epididymal “string of beads” sign may be present indicating global testicular infarction .