Purpose
Head and neck cancer is the 7th most common cancer in Australia,
with 4,956 cases predicted in 2017.
Curativetreatment of mucosal head and neck cancer typically consists of radical radiotherapy (with or without chemotherapy) or surgical resection (with or without adjuvant radiotherapy or chemoradiotherapy).
Such approaches yield a 5-year survival rate of around 69%,
with a significant burden of acute and late side effects.The Magnetic Resonance in Mucosal Primary Head and Neck Cancer (MRI in MPHNC) study aims to measure and track changes in functional...
Methods and materials
The study opened for recruitment in May 2016.
Patients receiving radical radiotherapy (with or without chemotherapy) are being prospectively recruited.
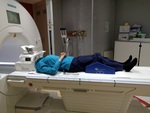
Scan setup is demonstrated in Fig. 1.
All patients are scanned on a 3 T wide bore scanner (Skyra,
Siemens,
Erlangen,
Germany) with standard anatomical imaging and functional studies as follows:
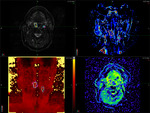
Diffusion weighted imaging (DWI) using RESOLVE sequences withb-values 50,
800 and calculated 1400 s mm-2
Dynamic contrast-enhanced imaging (DCE) using a TWIST sequence over 60 timepoints with temporal resolution of 5.64 s (Fig. 2)...
Results
Fifteen patients have been recruited and 53 scan sets have been carried out.
Early analysis of the data reveals results consistent with other published series.
DCE-MRI
Mean values of Ktransdid not exhibit any clear trend for either the primary lesion (Fig. 5) or the nodal disease (not shown)
BOLD-MRI
Mean values of R2* were reasonably consistent across the two measurements taken at each scan visit,
but did not show any clear trend for either the primary lesion (Fig. 6) or the nodal disease (not shown)...
Conclusion
Serial functional imaging including dynamic contrast-enhanced sequences is feasible in a prospective study of patients undergoing radiotherapy for mucosal primary head and neck cancer.
Initial analysis confirms previously observed trends in mean ADC values during radiotherapy.
Further images will be analysed for prognostic value as recruitment continues and mature outcome data become available.
More detailed analysis of the distribution of voxel values for the volumes imaged is planned and may provide more insights into patterns of change during treatment.
Personal information
Christopher Rumley is a Radiation Oncologist and Postgraduate Fellow at Liverpool Cancer Therapy Centre,
and a PhD candidate at the University of New South Wales.
References
Tyagi,
N.,
et al.
(2016).
"Weekly response assessment of involved lymph nodes to radiotherapy using diffusion-weighted MRI in oropharynx squamous cell carcinoma." Med Phys 43(1): 137-147.
Min,
M.,
et al.
(2016).
"Assessment of serial multi-parametric functional MRI (diffusion-weighted imaging and R2*) with (18)F-FDG-PET in patients with head and neck cancer treated with radiation therapy." Br J Radiol 89(1058): 20150530.
Shukla-Dave,
A.,
et al.
(2012).
"Dynamic contrast-enhanced magnetic resonance imaging as a predictor of outcome in head-and-neck squamous cell carcinoma patients with nodal metastases." Int J...