Aims and objectives
This is a systematic review of minimally invasive thermal ablative techniques aimedto provide pain relief to patients with bone metastases.
We reviewed efficacy,
duration of pain relief and complications of themajor ablation techniques: radiofrequency (RFA),
microwave (MWA),
cryoablation (CA) and MR-guided focused ultrasound (MRgFUS).
The primary endpoint was to determine the variation of referred pain after treatment at different time points; the secondary endpoint was toassess procedural complication rates for each technique.
Methods and materials
We searched MEDLINE/Pubmed,
MEDLINE In-Process,
EMBASE,
the Cochrane database using the keywords “ablation”,
“painful”,
“bone”,
“metastases” combined in multiple algorithms.
Inclusion criteria were: 1) original clinical studies published between 2001 and 2016 2) RFA,
MWA,
CA or MRgFUS 3) quantitative pain assessment before and after thermal ablation of bone metastasis.
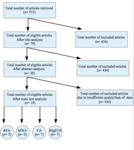
Exclusion criteria were: a) patient population n<5 b) lack of pain assessment at 1 and 3 months after the procedure.
Pain scales used were converted to a ten-point scale to be compared.
Out of a...
Results
100% of technical success with effective pain reduction up to 6-month follow-up was reported.
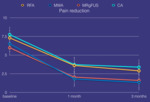
Pre-procedural mean pain score was 7.03±1.08.
At 1 month patients experienced a mean pain relief of 3.71±0.77 points after RFA,
5.33±0.25 after MWA,
3.68±1.34 after CA and 3.94±0.92 after MRgFUS.
At 3 months pain relief further increased (4.40±1.24 for RFA,
5.18±0.04 for MWA,
4.4±0.92 for MRgFUS,
4.98±0.61 for CA).
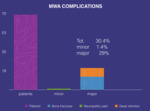
MRgFUS treatments caused no complications (0%) whereas MWA was associated with the highest complication rate (30%).
Pain relief curves are shown in...
Conclusion
All techniques offered significant pain relief after 1 and 3 months confirming the role of thermal ablation in palliation of bone metastases.
At 3 months observed painreduction rates were: RFA = 44%,
MWA = 52%,
MRgFUS = 44%.
CA = 50% .
MRgFUS has shown negligible complications rate,
whereas MWA had a noteworthy rate of adverse events.
A standardized pain reporting should be adopted in future studies for meta-analysis.
References
1.
Nielsen OS,
Munro AJ,
Tannock IF (1991) Bone metastases: pathophysiology and management policy.
J Clin Oncol 9:509–524.
doi: 10.1200/jco.1991.9.3.509
2.
Kurup AN,
Callstrom MR (2010) Image-guided percutaneous ablation of bone and soft tissue tumors.
Semin Intervent Radiol 27:276–284.
doi: 10.1055/s-0030-1261786
3.
Moher D,
Liberati A,
Tetzlaff J,
et al.
(2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement.
PLoS Med 6:e1000097.
doi: 10.1371/journal.pmed.1000097
4.
Wells GA,
Shea B,
O’Connell D,
et al.
The Newcastle-Ottawa Scale (NOS) for assessing the quality of...