Aims and objectives
The Human Papilloma Virus (HPV) is currently responsible for an increasing number of head and neck cancers,
regardless of exposure to smoking and drinking [1,2].
The oropharynx is the most affected site because the virus replicates in the lymphoepithelial tissue of the palatine and lingual tonsil [3].
HPV-positive(HPV+) squamous cell carcinomas of the oropharynx (OPSCC) have a better prognosis than their HPV-negative (HPV-) counterparts and respond better to chemo and radiotherapy [4].
In fact,
the latest edition of the AJCC has separated the squamous cell...
Methods and materials
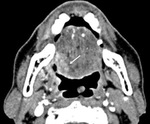
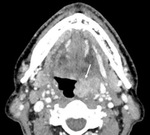
We retrospectively evaluated patients diagnosed with OPSCC(palatine tonsils and tongue base).
81 patients were recruited regardless of tumour staging; of these,
12 were excluded because they had not undergone contrast-enhanced staging CT in our hospital and 7 were excluded due to important artefacts from metal implants or dental amalgam (Fig. 3).
62 patients were finally included,
44 men and 18 women,
the age ranged from 42 to 81 years.
HPV status was established by evaluating overexpression of p16 protein by immunohistochemistry.
CT scans were evaluated...
Results
33 patients were HPV-positive and 29 HPV-negative.
Eight patients had no identifiable primary lesion: 5 were HPV+ and 3 HPV- and were excluded from the assessment of the primary lesion.
Nine patients had no lymph node metastases: 4 were HPV+ and 5 were HPV- and were excluded from the morphological evaluation of lymphadenopathy.
Exophytic growth pattern of primary tumour was found in 17/28 (61%)HPV+OPSCC and in 9/26 (35%) inHPV-OPSCC without statistically correlation,
although it was more frequent in theHPV+OPSCC (Fig. 9).
The tendency to invade...
Conclusion
Our case series shows a statistically significant correlation between:
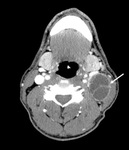
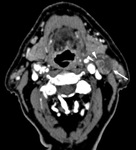
- the cystic changes of the lymphadenopathy and the presence of HPV+ status
- thedeep muscle invasion of the primary lesion and the HPV status
according to the literature [6-8] (Fig. 13).
The invasion of deep muscles and the more typically infiltrative aspect of HPV- OPSCC is correlated to a greater aggressiveness of these tumours given by numerous gene mutations induced by exposure to smoke and alcohol,
as opposed to HPV+ tumours that often arise in...
Personal information
Dr.
Giovanni Battista Verrone
Department of Radiology,
Careggi University Hospital,
Florence,
Italy.
[email protected]
References
Marur S,
D’Souza G,
Westra WH,
Forastiere AA (2010) HPV-associated head and neck cancer: A virus-related cancer epidemic.
Lancet Oncol 11:781–789.
doi: 10.1016/S1470-2045(10)70017-6
Castellsagué X,
Alemany L,
Quer M,
et al (2016) HPV Involvement in Head and Neck Cancers: Comprehensive Assessment of Biomarkers in 3680 Patients.
J Natl Cancer Inst 108:1–12.
doi: 10.1093/jnci/djv403
Abogunrin S,
Di Tanna GL,
Keeping S,
et al (2014) Prevalence of human papillomavirus in head and neck cancers in European populations: a meta-analysis.
BMC Cancer.
doi: 10.1186/1471-2407-14-968
O’Rorke MA,
Ellison M...