Aims and objectives
Radiological investigations have become an essential part of clinical medicine,
resulting in a substantial increase in the use of modalities that utilise ionising radiation.
In 2017,
4.6 million CT scans were performed in England; an increase of 3 million compared to 1996 [1].
Exposure to ionising radiation,
especially cumulatively,
is associated with an increased lifetime risk of developing cancer [2].
This can be explained by the stochastic effect,
in which the probability of developing cancer is proportional to the dose of ionising radiation.
However,
the...
Methods and materials
An online survey was distributed to all junior doctors including Foundation year 1 (FY1) and Foundation year 2 (FY2) and General Practitioner trainees (GPST1-GPST3) at Whipps Cross University Hospital (part of Barts Health NHS Trust).
Participants were given three months to complete the survey with tri-weekly reminders.
Foundation training refers to a two-year mandatory training programme (FY1 and FY2) for doctors who have completed their five-year undergraduate medical degree in the UK.
General Practitioner training is a three-year programme (GPST1-GPST3) that can be completed following...
Results
Of the 171 surveys sent,
a total of 50 doctors completed the survey (response rate 29%).
There were 24 FY1 doctors,
16 FY2 doctors and 10 GP trainees.
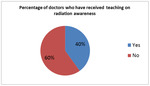
Theme 1: Formal teaching on radiation awareness
A total of 20 out of 50 doctors (FY1 n=8,
FY2 n=7 and GPST n=5) had received some form of formal teaching on radiation awareness,
and 60% had never received any teaching on radiation awareness whatsoever Fig. 2.
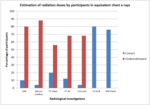
Theme 2: Estimation of the radiation dose in common radiological investigations
Doctors...
Conclusion
There appears to be a significant deficiency in radiation awareness amongst junior doctors.
Despite more years of medical experience,
there seems to be no overall difference in radiation awareness.
The majority of participants underestimated the radiation doses and the associated lifetime cancer risk for most radiological investigations.
This may result in patients undergoing an increasing number of radiological investigations,
and hence an overexposure to ionizing radiation.
Furthermore,
it is essential for referrers to inquire about pregnancy to avoid unnecessary foetal exposure to ionising radiation.
Although...
References
Dixon,
S.
(2017) Diagnostic Imaging Dataset Statistical Release.
England,
UK: NHS England.
Available at: https://www.england.nhs.uk/statistics/statistical-work-areas/diagnostic-imaging-dataset/ (Accessed December 01,
2018).
Berrington de Gonzalez,
A.
and Darby,
S.
(2004) 'Risk of cancer from diagnostic X-rays: estimates for the UK and 14 other countries',
Lancet, 363(9406),
pp.
345-51.
Thomas,
G.
and Symonds,
P.
(2016) 'Radiation Exposure and Health Effects – is it Time to Reassess the Real Consequences?',
Clinical Oncology journal, 28(4),
pp.
231-6.
Shaw,
P.,
Duncan,
A.,
Vouyouka,
A.
and Ozsvath,
K.
(2011) 'Radiation exposure and pregnancy',...


![Table 1: This table demonstrates typical effective doses of the radiological investigations, in mSv and equivalent number of chest x-rays [6]. References: Y. Al-Obudi, R. S. Malliwal; London/UK](https://epos.myesr.org/posterimage/esr/ecr2019/148101/media/800939?maxheight=150&maxwidth=150)