Learning objectives
To present a series of challenging cases of gallbladder and biliary tract disease from our institution.
To discuss the pathophysiology,
key imaging findings and main treatment of these conditions.
Background
The gallbladder and the biliary tract are subject to a wide variety of pathologies secondary to congenital,
calculous,
infectious,
inflammatory,
traumatic,
neoplastic and iatrogenic causes.
Most patients will have a similar clinical presentation that consists mainly of abdominal pain,
jaundice and fever.
The overlap of signs and symptoms can lead to a delayed in diagnosis and treatment,
increasing the incidence of complications.
To evaluate such pathologies,
we often require a multimodality imaging approach.
Abdominal ultrasound (US) is often the first used imaging study due to...
Findings and procedure details
CASE 1.
A 43-year-old female presents with right upper abdominal pain for the past 2 months.
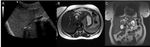
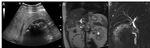
The patient underwent abdominal US and MRCP,
Fig. 1.
What are the main findings? What is your differential diagnosis?
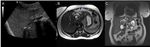
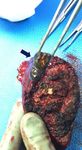
Answer: Fig. 2,
Fig. 3.
Recurrent pyogenic cholangitis,
also known as oriental cholangiohepatitis,
is characterized by multiple episodes of cholangitis with the formation of intrahepatic pigmented stones.
The etiology is poorly understood but is commonly attributed to parasitic infection by Clonorchis sinensis in endemic areas such as East Asia,
or...
Conclusion
There are many unusual conditions of the gallbladder and biliary tract that may have a similar clinical presentation but differ significantly in etiology and treatment.
Imaging plays a key role in the diagnosis and treatment planning.
MRCP has been proposed as the most accurate non-invasive imaging tool to evaluate the biliary system.
It is imperative for every radiologist to be familiar with these pathologies in order to make the correct diagnosis and facilitate the adequate treatment.
References
1.
Bali MA,
Pezzullo M,
Pace E,
Morone M.
Benign biliary diseases.
Eur J Radiol.
2017 Aug;93:217-228.
2.
Furlan A,
Ferris JV,
Hosseinzadeh K,
Borhani AA.
Gallbladder carcinoma update: multimodality imaging evaluation,
staging,
and treatment options.
AJR Am J Roentgenol.
2008 Nov;191(5):1440-7.
3.
Levy AD,
Murakata LA,
Abbott RM,
Rohrmann CA Jr.
From the archives of the AFIP.
Benign tumors and tumorlike lesions of the gallbladder and extrahepatic bile ducts: radiologic-pathologic correlation.
Armed Forces Institute of Pathology.
Radiographics.
2002 Mar-Apr;22(2):387-413.
4.
Luu MB,
Deziel DJ....