Learning objectives
To review and distinguish the imagiological findings of external,
internal,
and diaphragmatic hernias on the basis of their localization,
with special focus on their atypical and less common appearances.
To describe the potential mimickers and complications of the abdominal hernias.
To review potential postoperative complications and failure of surgical repair of abdominal hernias.
Background
Abdominal hernias are among the most common surgical problems,
and a leading cause of abdominal pain and intestinal obstruction.
The main types of abdominal hernias are external hernias,
which involve protrusion of abdominal contents through a defect in the abdominal wall; internal hernias,
with protrusion of viscera through the peritoneum,
mesentery or a compartment in the abdominal cavity; and diaphragmatic hernias,
involving protrusion of abdominal contents into the chest.
Findings and procedure details
ABDOMINAL WALL HERNIAS
Umbilical Hernias
Umbilical hernias are the most common type of ventral hernias and are usually asymptomatic.
They are habitually congenital,
resulting from incomplete closure of the abdominal wall after ligation of the umbilical cord.
In adults they appear generally in context of multiple pregnancies,
ascites,
obesity,
abdominal masses or chronic increased abdominal pressure.
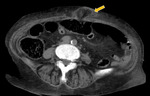
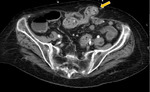
The herniated sac usually contains the greater omentum or bowel loops,
that can be incarcerated,
causing symptoms of intestinal obstruction and local tenderness (Fig.1).
Paraumbilical Hernias
Paraumbilical hernias arise...
Conclusion
Abdominal hernias are a common clinical problem.
Familiarity with the appearances of various types of abdominal hernias allows confident diagnosis of these entities and their complications.
References
Aguirre DA,
Casola Giovanna,
Sirlin Claude.
Abdominal Wall Hernias: MCDT Findings.
AJR:183,
September 2004.
Aguirre D,
Santosa A,
Casola G,
Sirlin C.
Abdominal Wall Hernias: Imaging.
Features,
Complications,
and Diagnostic Pitfalls at Multi-Detector Row CT.
RadioGraphics.
2005;25:1501-1520.
Ulloa L,
Camargo C,
Carrillo J,
Luna D,
et al.
Evaluación tomográfica de las hernias de la pared abdominal.
Rev Colomb Radiol.
2008; 19(2):2387-96.
Stabile Ianora AA,
Midiri M,
Vinci R,
et al.
Abdominal wall hernias: imaging with spiral CT.
Eur Radiol 2000;10:914–919.
Diego A et al.
Abdominal...