Aims and objectives
Lung involvement is common in connective tissue diseases (CTDs),
an heterogeneous group of systemic immunologically mediated inflammatory disorders.
[1]
As many as 25% of patients with features of a systemic autoimmune disease do not fulfill American College of Rheumatology (ACR) classification criteria for a defined CTD,
such as Systemic Sclerosis,
Systemic Lupus Erythematosus,
Sjogren’s Syndrome,
Polymyositis/Dermatomyositis and Rheumatoid Arthritis.
These patients are considered to have undifferentiated connective tissue disease (UCTD).
[2]
The natural history of UCTD still remains unknown and unpredictable.
Most of cases (65-94%)...
Methods and materials
Study population: In this retrospective descriptive study,
we reviewed CT scans obtained in 22 patients with a clinically and serologically diagnosis of UCTD who underwent a CT examination of the chest at Azienda Ospedaliero–Universitaria,
Policlinico di Modena,
Italy,
during a mean 5 year follow up period (range 3 to 7 years).
The diagnosis of UCTD was made according to Mosca et al.
[4] who proposed the following classification criteria: at least one clinical manifestation of CTDs without fulfilling the criteria of definite CTD,
positive ANA...
Results
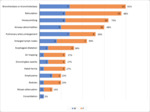
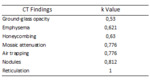
The most common CT features were those related to fibrosis: traction bronchiectasis [20 (91%) patients],
reticulations [19 (86%) patients] and honeycombing [16 (73%) patients].
Airways abnormalities (68%) were also frequently seen; nodules were observed in 5 (23%) patients.
All the thoracic findings found on HRCT scans ofour patients are summarized inFig.1 and Fig.2.
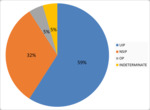
Interobserver agreement for the presence of HRCT features was mostly good (good to excellent agreement),
except for the evaluation of GGO (moderate agreement).(Fig.3)
Reticulations,
honeycombing and GGO were bilateral in most of...
Conclusion
We reviewed CT scans obtained in 22 patients with a clinically and serologically diagnosis of UCTD; they underwent an HRCT examination because of their respiratory symptoms and impairment of pulmonary function test results.
All of them showed a parenchymal lung involvement,
particularly the finding of interstitial lung disease with different patterns.
It is commonly known that the most of ILD associated with CTD is characterized by the radiologic and histopathologic pattern of NSIP,
especially in systemic sclerosis,
Sjӧgren’s syndrome and dermatomyositis/polymyositis.
Otherwise,
the UIP pattern...
Personal information
Stefania Ghinassi,
Dipartimento interaziendale di Diagnostica per Immagini,
Azienda Ospedaliero-Universitaria Policlinico di Modena (
[email protected])
Giovanni Della Casa,
Dipartimento interaziendale di Diagnostica per Immagini,
Azienda Ospedaliero-Universitaria Policlinico di Modena (
[email protected])
References
1.
Gutsche M,
Rosen GD,
Swigris JJ.
Connective Tissue Disease-associated Interstitial Lung Disease: A review.
Curr Respir Care Rep.
2012;1:224-232.
2.
Kinder BW,
Shariat C,
Collard HR,
et al.
Undifferentiated connective tissue disease-associated interstitial lung disease: changes in lung function.
Lung.
2010;188(2):143-9.
3.
Mosca M,
Tani C,
Vagnani S,
Carli L,
Bombardieri S.
The diagnosis and classification of undifferentiated connective tissue diseases.
J Autoimmun.
2014;48-49:50-2.
4.
Mosca M,
Neri R,
Bombardieri S.
Undifferentiated connective tissue diseases (UCTD): a review of the literature and a proposal...