Learning objectives
We designed a quality improvement project to assess the identification and reporting of osteoarthritis (OA) and cartilage abnormalities on knee MRI scans performed at our institution,
a district general hospital in Devon,
UK.
Background
•OA is the most prevalentform of arthritis
•Big impact on individual health and quality of life and public health in general
•Patients with meniscal tears who also have OA probably do not benefit from arthroscopic surgery [1],
therefore it is important to correctly identify and highlight OA changes on the MRI scans
•There are several established plain film grading systems for osteoarthritis,
we used a simple adaptation for MRI findings:
Mild: mild cartilage thinning,
small osteophytes
Moderate: near full thickness cartilage loss,
mild bone marrow...
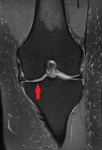
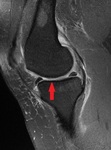
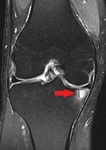
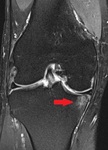
Imaging findings OR Procedure Details
Results:
Cartilage grading:
Initial report: cartilage grade provided in 19 reports (38%)
Of the 19: 13 numerical grading (a score based on the Outerbridge classification of patellar cartilage [2]),
6 written grading (mild / moderate / severe)
Musculoskeletal radiology review agreed with the cartilage grade provided in 63%
Overal there wasimprovedagreement with increasing severity of grade
Figure 8 is a pie chart showing the variation in grade of OA found at musculoskeletal review in the study population.
A description of the cartilage wasgiven in 14...
Conclusion
Discussion and Conclusions:
We found a significant variation in cartilage reporting / grading in MRI reports at our institution,
Numerical
Mild / moderate / severe
Descriptive
The cartilage was not mentioned at all in 22% of the knee MRI reports included in our study.
50% of the cases with bone marrow oedema and subchondral cysts,
important indicators of osteoarthritis,
were not reported as such.
Research groups have reported that bone marrow oedema correlates well with pain [3],
therefore it isessential to accurately identifiy this on...
References
[1] Siemieniuk R et al.
Arthroscopic surgery for degenerative knee arthritis and meniscal tears: a clinical practice guideline.
BMJ 2017;357:j1982.
[2] Outerbridge RE.
The etiology of chondromalacia patellae.J Bone Joint Surg Br.1961;43:752–757.
[3] Tanamas S et al.
Bone marrow lesions in people with knee osteoarthritis predict progression of disease and joint replacement: a longitudinal study.
Rheumatology,
Volume 49,
Issue 12,
December 2010,
2413-2419.