Keywords:
Cardiac, Echocardiography, CT-Angiography, MR, Contrast agent-intravenous, Diagnostic procedure, Congenital, Tissue characterisation, Image verification
Authors:
V. Barskiy, V. Sinitsyn, L. A. Yurpolskaya, E. Basargina, Y. Shmeleva, I. Filinov, A. Sugak, I. Silnova, M. umarova; Moscow/RU
Results
Poster presents a spectrum of clinical cases with true LVNC and cases when hypertrabeculations have secondary or incidental origin,
being combined with other cardiac diseases.
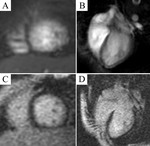
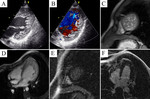
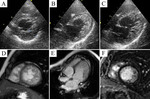
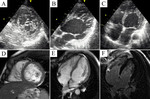
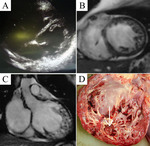
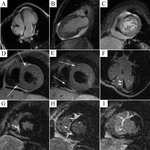
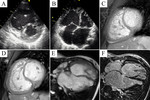
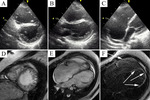
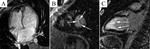
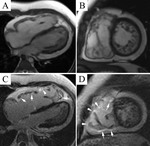
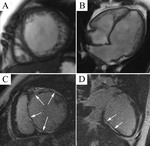
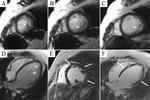
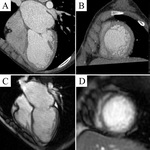
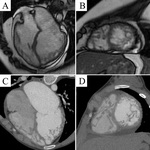
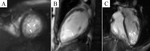
Typical cases of LV non-compaction are shown on Fig.
1-4.
These patients were asymptomatic but they had typical signs of LVNC by echocardiography and MRI.
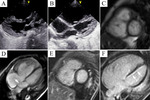
One more patient with LVNC had died from fatal pulmonary thromboembolism (Fig.
5).
A patient with a large atrial septal defect,
RV dilation and trabecular layer on top of the LV,
also had MR images, suggestive of LVNC,
but most probably in this case hypetrabelculation of LV had secondary origin (Fig.
6).
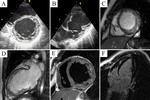
Fig.
7 shows advantages of MRI over echocardiography in vizualisation of non-compacted myocardium.
Fig.
8 demonstrate a rare case of congenital aneurysm of LV combined with LV non-compaction (an attempt of surgical correction of the aneurysm had been done).
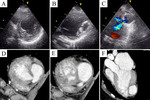
Case 9 demonstrates combination of LV hypetrabeculations with fibrosis of IVS from the right side of unknown origin.
Existence of right-sided NC has been discussed in the literature,
but such cases are difficult to discriminate from ARVC.
Such case is shown on fig.10.
Secondary hypertrabeculation of LV in patient with chronic myocarditis and cardiomegaly is depicted on fig.11.
In some patients with LVNC LGE MRI shows hyperenhancement of non-compact layer due to fibrotic changes (fig.
12).
A patient with severe ARVC also had typical manifestations of LVNC (fig.13) and it stayed unclear – was it a case of one single cardiomyopathy or two different ones.
Case 14 shows a case of chronic myocarditis with LV dilatation with marked fibrotic changes in the myocardium,
where non-compaction was probably seen due to thinning of the LV myocardium with preservation of trabeculations.
Last 4 cases show combination of LV non-compaction (of secondary origin) with primary and secondary cardiomyopathies.
Fig.15 demonstrates LV secondary hypertrabeculation of LV in patient with dilative cardiomyopathy (DCM).
Fig.16 and 17 demostrate LV hypertrabeculation (not fulfilling criteria for LVNC) in patients with (probably) restrictive cardiomyopathies.
Last case (fig.18) shows LV hypertrabeculation in in 8-year-old patient with mitochondrial encephalomyopathy.
At the age of 1.5 years he suffered from an ischemic stroke.
The cause of stroke could not be established.
Dilatation of LV with boundary hypertrabeculations in combination with decreased EF could be a risk factor for thrombi formation and cerebral embolism.