Keywords:
Obstruction / Occlusion, Fistula, Arteriovenous malformations, Diagnostic procedure, CT-Angiography, CT, Thorax, Cardiovascular system, Cardiac
Authors:
M. Juarez García, G. Burcet Rodríguez, A. Roque, L. Dos, B. Miranda, M. Escobar, H. Cuéllar; Barcelona/ES
Results
The CTA report of eight patients (2%) met the previously described criteria: an abnormality in the drainage of a single PV without partial anomalous pulmonary venous return. Prior surgery for congenital heart disease repair had been performed in all patients (Full description of pathology and surgical technique in Table 1).
The abnormality of the PV was classified in three types:
-
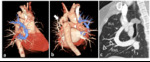
Agenesia: no vascular structure directly connecting the involved pulmonary lobe to the LA (2, 4). It was found in two patients (25%) with a history of surgically corrected aortic coarctation. Since the LA was not involved in the surgical procedure, we considered it as a congenital condition (Figure 1).
-
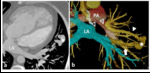
Occlusion: focal or segmental discontinuation of a vascular structure directly connecting the involved pulmonary lobe to a patent ostium at the LA (2). It was found in five patients (63%) (Figure 2) with a history of surgical repair in which the procedure involved the LA, therefore we considered it as an acquired condition.
-
Stenosis: Significant focal reduction of a vascular structure directly connecting the involved pulmonary lobe to a patent ostium at the LA (2, 9). We only identified one patient (12%) with PV stenosis in our series, which was also considered as acquired, since the reported surgical technique involved the LA.
In all cases the affected pulmonary lobe drained into the LA through a venovenous connection. With a careful re-analysis of the available images we divided these connections into two main types:
-
Meandering pulmonary vein (MPV) (n=4), defined as a single vein of significant caliber with an abnormal course that drains indirectly to the LA, through a connection to another PV. To our knowledge, this type of communications have been previously reported in the literature as congenital malformations associated with abnormal lungs. We only found a report where it was described as a postsurgical complication (3). In our series, all patients with MPV had undergone prior surgery for CHD. The MPV was considered as a congenital abnormality in two patients where the surgery did not involve the LA (aortic coarctation repair) (Figure 1). In the other two cases the MPV may have developed after PV obstruction during surgery with LA involvement (Figure 2). In all four cases the MPV crossed to the adjacent lobe through gaps in the mediastinal side of the fissure (Figure 1) (12), frequently close to branches of the pulmonary artery.
-
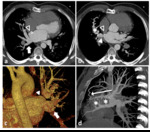
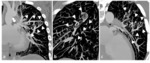
Multiple plexiform connections (MPC) (n=4), defined as a bunch of multiple small vessels communicating the peripheral venous branches of the impaired lobe with those of the adjacent lobe. We have not found any previous description in the literature of these small and multiple venovenous communications. In our series, all four patients with MPC had a history of surgery with potential LA involvement, so they may be an acquired condition secondary to PV obstruction. Collateral septal veins may develop when the lung drainage is impaired. In three patients the MPC were spread along the involved lung fissure and the vessels apparently pierced it (Figures 3 and 4). In the remaining case the obstructed superior segments of the left upper lobe drained through intralobar MPC to the vein of the lingular segments, which joined the left lower lobe vein.
The PV obstruction involved the upper lobes in 88% of cases, and the venous connections always drained to the adjacent lobe on the same side. Of note, the original description of the meandering vein was restricted to the right lung (9), but in our series PV abnormalities and typical MPV were left-sided in 75% and 60% of cases, respectively. Overall, the venous connections crossed a lung fissure in 88% of cases.
The venous abnormalities were correctly diagnosed for the first time by cardiac CTA, although all patients had been previously studied by other cardiac imaging techniques, including echocardiography and cardiac magnetic resonance. Three of the patients had been wrongly diagnosed as arteriovenous fistulas (2 cases) and a venous pulmonary varix (1 case).
Three patients were asymptomatic (38%), and four patients (50%) showed symptoms attributable to their main CHD. Only one case of atrial switch surgery with an occluded PV and a meandering vein presented clinically with hemoptysis, which was initially attributed to a misdiagnosed pulmonary arteriovenous fistula.