Based on our department database,
we will present and illustrate the CT characteristics of smoking-related lung diseases.
COPD
COPD includes several distinct but overlapping syndromes,
including chronic bronchitis,
emphysema,
reversible and irreversible small airways disease.
CT findings of COPD include:
1. Emphysema:
1.1. Centrilobular emphysema (CLE):
- CLE is characterized by destruction of centrilobular alveolar walls with enlargement of respiratory bronchioles and associated alveoli.
- It is the most common type of smoking-related emphysema,
being usually upper lung predominant;
- CT imaging findings: small well-defined or poorly defined areas of low attenuation surrounded by normal lung parenchyma,
which may range from less than 1 mm to more than 3 cm in diameter; centrilobular pulmonary arteries or arterioles may be seen traversing the hypoattenuated areas.
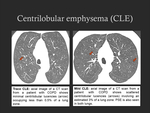
- A statement of the Fleischner Society has identified five visually defined phenotypes of CLE emphysematous destruction [3]: trace CLE,
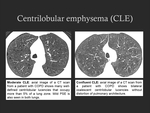
mild CLE,
moderate CLE,
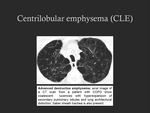
confluent CLE and advanced destructive emphysema (ADE) (Fig. 1,
Fig. 2,
Fig. 3).
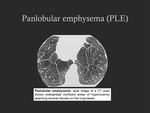
1.2. Panlobular emphysema (PLE):
- It corresponds to diffuse destruction across the whole secondary lobule;
- Linked to a genetic defect in the alpha 1-antitrypsin gene; however,
it may occur in patients without alpha 1-antitrypsin gene deficiency,
namely in smokers with advanced emphysema;
- In patients with alpha 1-antitrypsin gene deficiency,
it commonly presents a lower lobe predominant pattern;
- CT imaging findings: widespread areas of abnormally low attenuation; however,
in mild cases it may be subtle and difficult to identify (Fig. 4).
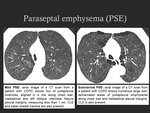
1.3. Paraseptal emphysema (PSE):
- It results from destruction of the distal acinus and presents a specific location,
near the pleural surface;
- Usually most marked in the upper and middle lung zones and along the mediastinum;
- CT imaging findings: subpleural areas of low attenuation with a well-defined wall; bullae (bulla is an airspace measuring over 1 cm in diameter) are common;
- A statement of the Fleischner Society has identified two visually defined phenotypes of PSE emphysematous destruction [3]: mild PSE and substantial PSE (Fig. 5).
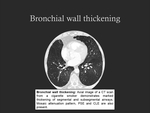
2. Bronchial wall thickening
- Characterized by thickening of the walls of segmental and subsegmental airways,
probably resulting from bronchial inflammation and remodeling;
- Frequently observed in heavy smokers,
especially in those with chronic bronchitis;
- CT imaging findings: relative increase in bronchial wall thickness compared with the bronchial lumen and with the diameter of the adjacent pulmonary artery (Fig. 6).
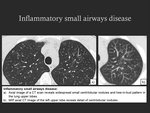
3. Small airways disease
- Inflammatory small airways disease results from inflammation in and around the small airways and can be identified on CT by the presence of peripheral centrilobular micronodular opacities (Fig. 7);
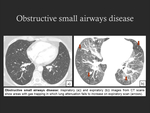
- Obstructive small airways disease can be identified by gas trapping on expiratory CT (Fig. 8) and/or by identifying physiologic obstruction,
in the absence of significant emphysema;
4. Other important CT features in COPD
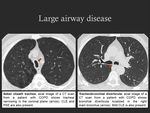
- Large airway disease (Fig. 9): tracheobronchomalacia (reduction in the tracheal luminal cross-sectional area by over 80% at dynamic expiratory imaging [3]),
saber sheath trachea (also known as keyhole trachea,
corresponding to tracheal narrowing in the coronal plane),
tracheobronchial diverticula.
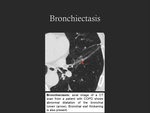
- Bronchiectasis: abnormal dilatation of the bronchial lumen; cylindrical type is the most common (Fig. 10).
- Pulmonary arterial enlargement: enlargement of the pulmonary artery,
suggesting pulmonary hypertension,
may occur in advanced COPD.
Lung cancer
Lung cancer can be divided into two categories: small cell lung cancer (SCLC) and non-small cell lung cancer (NSCLC).
NSCLC is further divided into three major subtypes: adenocarcinoma,
squamous cell carcinoma and large cell carcinoma.
Cigarette smoking is the most important single risk factor for lung cancer.
CT is the imaging modality of choice in lung cancer imaging: it can detect small lesions,
characterize and stage lung cancer,
define the disease extent and extrathoracic spread.
On imaging,
lung cancers can be divided in:
1. Peripheral tumors: tumors arising beyond the hilum/segmental bronchi
2. Central tumors: tumors arising at or close to the hilum/segmental bronchi
Lung cancer presents a wide spectrum of imaging appearances:
• Shape: variable; peripheral tumors are commonly spherical or oval; Pancoast tumors may resemble apical pleural thickening.
• Borders: tumors usually have lobular,
irregular or spiculated and well-defined borders,
but they may be ill-defined.
• Mucoid impaction: some tumors may present with mucoid impaction,
resembling bronchoceles,
due to bronchial stenosis.
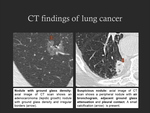
• Ground-glass density (Fig. 11): malignant nodules may present with ground-glass attenuation.
Ground-glass halo around a tumor may be due to adjacent inflammation,
hemorrhage,
edema or tumor lepidic growth (e.g.
adenocarcinoma in situ).
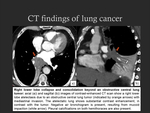
• Lung collapse and consolidation beyond an obstructive central lung tumor (Fig. 12): obstruction of a major bronchus by a central lung tumor can lead to atelectasis and retention of secretions with localized consolidation (which may become secondarily infected).
In these circumstances,
defining the presence and extent of the central tumor may be difficult,
but it is important for therapeutic planning.
The pattern of contrast enhancement may help us differentiate the tumor from the atelectatic lung - while tumors usually present slight enhancement,
atelectasis can show substantial enhancement.
When a central tumor is associated with lobar atelectasis,
golden S-sign may be present.
• Air bronchograms and cyst-like lucencies (Fig. 11): may occur in malignant tumors (e.g.: adenocarcinoma).
• Calcification: rare; most correspond to preexisting calcifications engulfed by the tumor; amorphous or cloudlike dystrophic calcifications may be seen.
• Cavitation: may be seen in tumors of any size; usually eccentric and with irregular walls of variable thickness; may present air and/ or liquid content.
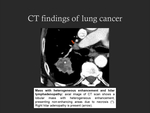
• Contrast enhancement: usually present; some may present heterogeneous enhancement due to the presence of necrotic regions which do not enhance (Fig. 13).
• Hilar enlargement: a common presenting feature; in central tumors,
it may result from the tumor itself,
from enlargement of metastatic hilar lymph nodes,
from consolidated lung or from a combination of the above.
Lung cancers may present associated lymphadenopathy (Fig. 13),
metastasis,
and they may cause bronchial,
vascular,
pleural,
pericardial,
mediastinal (Fig. 12),
neural (e.g.: phrenic nerve invasion,
brachial plexus invasion in Pancoast tumors),
vertebral,
diaphragmatic and/ or chest wall invasion.
These aspects are important for lung cancer staging and they influence the prognosis and treatment options of the patient.
However,
the staging of lung cancers is beyond the scope of this poster.
Smoking-related ILDs
Cigarette smoking is related to the development of several ILDs,
some of which may coexist in the same patient.
In smoking-related ILDs,
an integrated clinical,
radiologic and pathologic approach is recommended for accurate diagnosis [4].
Although the imaging and histologic features frequently overlap among these entities, distribution of the lesions,
particularly lung nodules and cysts,
on CT can help narrow the differential diagnosis of smoking-related ILDs.
● Respiratory bronchiolitis-interstitial lung disease (RB-ILD)
- Disease entity associated with the presence of symptoms (commonly mild cough and dyspnea),
abnormal pulmonary function test results and imaging abnormalities.
- Respiratory bronchiolitis is the histopathologic lesion found at lung biopsy (the same histopathologic lesion is also present in asymptomatic smoker patients with respiratory bronchiolitis).
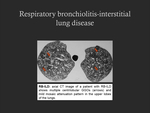
- CT imaging findings: centrilobular nodules and ground glass opacities (GGOs) with central lung region and upper lobe predominance,
mild mosaic attenuation/ air trapping (Fig. 14).
Other changes related to smoking,
like bronchial wall thickening and centrilobular emphysema may coexist.
● Desquamative interstitial pneumonitis (DIP)
- Rare disease,
strongly associated with cigarette smoking.
- Thought to represent the end stage of RB-ILD,
presenting similar histopathologic findings.
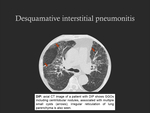
- CT imaging findings: GGOs with subpleural and basal predominance; small cysts or emphysema may be associated with the GGOs (Fig. 15); in a few patients,
fibrosis may develop in areas previously affected by GGOs,
manifested by irregular reticulation and traction bronchiectasis; honeycombing is rare.
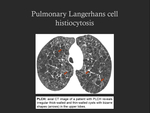
● Pulmonary Langerhans cell histiocytosis (PLCH)
- In adults,
PLCH occurs primarily in smokers and the symptoms are variable.
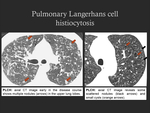
- CT imaging findings: combination of nodules and cysts with upper lobe predominance,
with sparing of costophrenic angles - early in the disease course,
small scattered nodules (usually with 1-5 mm) are typically seen; as the disease progresses the nodules may cavitate and irregular thick-walled cysts with bizarre shapes develop; later in the disease course,
the cysts become thin-walled (Fig. 16,
Fig. 17).
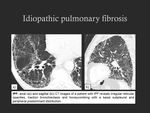
● Idiopathic pulmonary fibrosis (IPF)
- IPF is a distinctive pattern of chronic idiopathic interstitial pneumonia of unknown cause,
associated with the histopathological pattern of usual interstitial pneumonia (UIP).
- A relationship between cigarette smoking and IPF is recognized [4,5].
- CT imaging findings: irregular reticular opacities,
traction bronchiectasis and bronchiolectasis,
and honeycombing with a basal,
posterior and subpleural distribution (Fig. 18); GGOs may be seen in areas of fibrosis,
reflecting active inflammation.
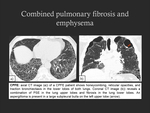
● Combined pulmonary fibrosis and emphysema (CPFE)
- Increasingly recognized as a distinct entity in smokers.
- Characterized by dyspnea,
pulmonary hypertension,
upper-lobe emphysema,
lower-lobe fibrosis and gas exchange abnormalities.
- CT imaging findings: combination of PSE and CLE in the upper lung lobes and fibrosis (with honeycombing,
reticular opacities,
and traction bronchiectasis) in the lower lung lobes (Fig. 19).
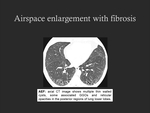
* Airspace enlargement with fibrosis (AEF)
- Identified pathologically as a smoking-related change [2].
- It could be included on the spectrum of smoking-related ILDs.
- Incidental CT and histologic findings in smokers,
not regarded as a distinct form of idiopathic interstitial pneumonia [6].
- The corresponding CT findings have not been well documented [6,7].
- CT imaging findings: multiple thin walled cysts and/or GGOs/ reticular opacities [8,9] (fig.
20).
It has been reported that the cysts are delineated by a wall with a thickness inferior to 1 mm,
they are not located in the lung base and present distant from the pleura (not abutting the pleura) [8].