Fontan procedure (Dr François Fontan,
1929-2018) reflects a spectrum of cardiothoracic surgeries when systemic venous return is diverted directly to the pulmonary arteries,
eliminating the ventricular component of the circulation chain.
Since the original surgery in 1971 (1),
the procedure has been modified several times and has resulted in prolonged survival of an important group in the population of congenital heart disease.
These surgeries have been performed in cases of functionally single ventricle: either only one anatomical ventricle or two that cannot be effectively separated.
The surgical approach is performed in series of procedures,
which gradually connect the single ventricle to the systemic and pulmonary resistances,
eliminating shunting and enabling full oxygenation of systemic arterial blood.
The patients now form a group of adult population,
who,
apart from being followed up routinely in specialised centres,
more frequently can be seen in general healthcare institutions.
Outline
- Pre-existing conditions
- Types of Fontan procedure
- Fontan haemodynamics in adults
- Imaging protocols
- Case-based review of imaging findings in adults with a focus on:
- satisfactory haemodynamical result
- spectrum of complications due to poor haemodynamics
Pre-existing conditions for Fontan surgery are severe forms of congenital heart disease which result in functionally single ventricle or in two ventricles which cannot be effectively separated surgically.
Common indications for Fontan procedure include:
- Double inlet left ventricle
- Tricuspid atresia
- Hypoplastic left heart syndrome
- Pulmonary atresia
Fontan procedure now combines a spectrum of cardiothoracic surgeries which eventually divert systemic venous flow directly into the pulmonary arteries,
bypassing the ventricular component.
This results in a virtually non-pulsatile flow to the caval veins and subsequently into the lungs.
Over the history of cardiothoracic surgery there have been many attempts of solving the issue of single ventricle until François Fontan and Eugene Baudet performed a surgery for tricuspid atresia (1).

Fig. 3: Video 1. Original Fontan procedure
References: Dr Monika Arzanauskaite
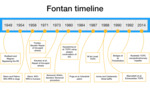
The surgery has been modified several times (see timeline in Fig. 1) and has resulted in prolonged survival of the patients who now can reach middle age.
A staged palliative surgery resulting in total cavopulmonary connection (TCPC) has become the preferred treatment option:
- In the neonatal period,
depending on the underlying anatomy,
unrestricted blood flow to the aorta (for example,
DKS in double inlet left ventricle,
Norwood procedure in hypoplastic left heart syndrome) and a balanced flow to the lungs (aortopulmonary shunt,
Blalock-Taussig shunt as in tricuspid atresia) must be achieved.
- The second stage typically is a Glenn- or hemi-Fontan operation,
performed by connecting the superior caval vein to the pulmonary arteries.
- TCPC (or Fontan circuit) is completed by connecting the inferior caval vein to the pulmonary artery using a fenestrated or non-fenestrated extracardiac conduit or an intra-atrial lateral tunnel (2).

Fig. 2: Figure 2. Still views of animations. Original Fontan procedure and common contemporary modifications.
References: Dr Monika Arzanauskaite
See illustrations in Fig. 2 ,
and corresponding animation in Video (Fig. 3) showing the common types of Fontan anatomy.
Imaging protocols
Cardiovascular magnetic resonance is the technique of choice to assess the ventricular size,
function and valve pathology in the setting of complex anatomy.
The modality is also very useful in evaluation of Fontan pathways for anastomotic stenosis,
residual intracardiac shunt and thrombus formation,
as well as in the assessment of thoracic and upper abdominal collateralisation.

Table 1: Table 1. Suggested MRI protocol
See Table 1 with a suggested protocol.
The study should include ECG-gating and breath-holding,
however,
the recent imaging advances have reduced the need of breath-holding in some sequences such as three dimensional acquisitions with diaphragmatic gating and free-breathing inversion recovery sequences for thrombus and scar assessment.
Some of the new high magnetic field scanners offer novel pre-sensing techniques,
reducing or eliminating the need of breath-holding in cine acquisitions.
These advances offer a more tolerable experience for patients.
Fontan pathway anatomy is best assessed by multiple cine and flow projections.
Additionally,
through plane flow measurements of IVC and SVC give additional or back up data for total systemic venous flow and shunt assessment,
particularly when in cases of challenging anatomy or significant regurgitation arterial flow measurements are unreliable.
Flow analysis is mandatory when assessing Fontan patients even though challenging due to altered anatomy and technical limitations such as the distance of the area of interest from the magnet iso-center and the angle from the transaxial plane.
Differential flow to the right and left lung as well as differential pulmonary venous return from the right and left lung can be calculated as well as the cardiac output (aortic flow).
The most useful sites of flow measurements are shown schematically in Fig. 4.

Fig. 4: Sites of flow measurements in Fontan circulation (Glenn procedure is shown as an example).
References: Dr Monika Arzanauskaite
The summed pulmonary venous flows should equal the summed pulmonary arterial flows as well as the forward aortic flow and the caval venous flow.
Any difference between the volume that returns to the systemic ventricle and the output volume from the aorta reflects a shunt either in the form of fenestrations/leaks/other anomalous intracardiac communications or in the form of collaterals. In particular the degree of volume load to the systemic circulation (veno-venous collaterals) or the pulmonary circulation (arterio-pulmonary collaterals) can be quantified with great accuracy by subtracting the caval venous flow from the aortic flow (QAo- (Qsvc+QIVC)) or by summing the difference of pulmonary venous flow to and pulmonary arterial flow from either lung ((QRPV-QRPA)+(QLPV-QLPA)),
respectively.
The important advantage of CMR imaging is that it allows flow measurements at any given site of interest allowing multiple calculations and internal validation.
Moreover,
the pulmonary arterial flows acquired by CMR can be used in conjuction with the invasively measured pressures for the accurate calculation of pulmonary arterial resistance (2)
Contrast angiography is very useful for smaller vessels; dynamic angiogram gives additional information about the anatomy of thoracic veins.
Free breathing three dimensional SSFP sequence is a relatively new technique which does not require breath-holding and provides a set of thin sliced images which can be later reconstructed in various planes in the same way as CT.
For thrombus formation,
the best approach is to use early gadolinium phase (within the first minute after contrast injection) inversion recovery sequence with high inversion time on pre-selected planes.
Late phase (15-20 minutes after contrast injection) is useful for assessment of ventricular or atrial scar formation.
Dedicated liver protocol (preferably with liver specific contrast agent) is used to assess the regenerative nodules,
if indicated.
Computed tomography in Fontan population plays a major role due increased risk of thromboembolism.
It is a good tool for the evaluation of anatomy.
Additionally,
cardiac function study can be performed if other techniques are inconclusive or not available.
The same acquisition can help to assess the lung parenchyma.
See Table 2 with common CT protocols.