Optimal imaging technique requires maximisation of sensitivity toward slow flow. The following parameters should be employed. High resolution, multifrequency transducer (7 MHz Doppler transmitting frequency), low pulse repetition frequency (750 KHz), low wall filter (50 Hz), high colour gain (immediately below artefact threshold).
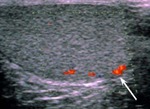
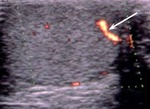
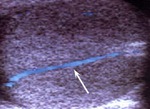
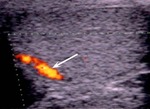
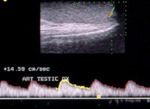
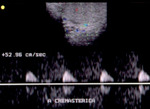
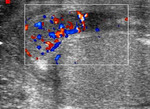
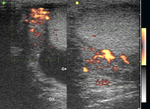
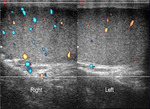
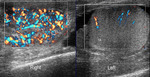
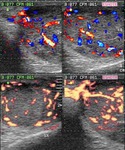
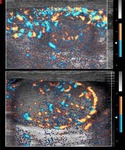
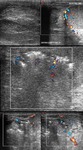
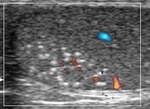
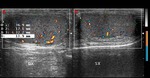
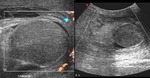
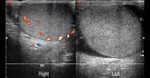
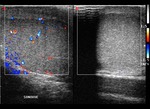
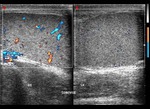
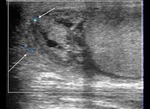
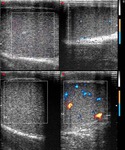
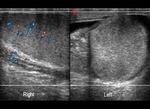
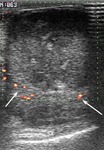
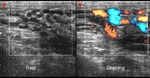
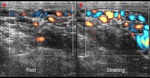
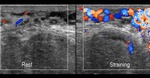
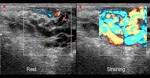
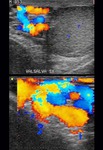
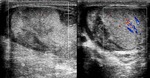
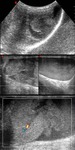
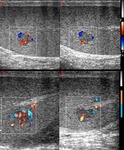
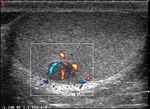
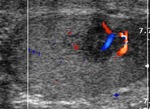
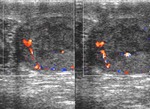
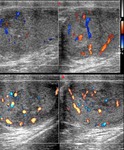
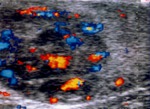
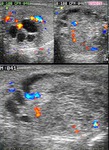
Normal vascular anatomy includes 1) testicular artery, arising from abdominal aorta and reaching the didimis (with capsular and centripetal branches) 2) cremasteric artery, arising from internal iliac artery and reaching funicle, epididymis, and sometime didimis lower pole 3) deferential artery, arising from internal pudendal artery and reaching scrotal sac. Half the subjects have a transmediastinal artery within testis (fig.1), (fig.2), (fig.3), (fig.4).
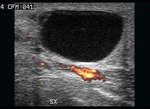
Spectral analysis shows low-resistance testicular arteries (0.48-0.75 resistive index) and high-resistance extratesticular arteries (0.63-0.9 resistive index) (fig.5), (fig.6).
Vascular signal from neonate or child testis is more difficult to be detected, because of small calibre and slow flow. Consequently, special attention should be paid before diagnosing increased, decreased, or absent testis perfusion.
Acute inflammatory process may mainly involve the epididymis, the didimis, or both (fig.7 ), (fig.8 ), (fig.9), (fig.10), (fig.11), (fig.12). Doppler techniques demonstrate intense hypervascularisation of involved structures with reduction in flow resistance. In subtle cases comparison with contralateral testis is mandatory.
In case of abscesualisation, colour-Doppler shows absent flow within necrotic and liquefied areas. Gas bubbles main cause reverberation twinkling artefact, not to misinterpret as flow persistence (fig.13 ).
Testicular microlithiasis is associated with bilateral calcifications possibly determining twinkling artefact on colour-Doppler scans (not to misinterpret as vascular signal) (fig. 14 ).
Testis atrophy may be associated with increased or with decreased vascular signal (fig. 15 ).
Testicular ischemia may be due to extrinsic compression (hematoma, abscess, solid mass) (fig. 16) but is commonly due to severe torsion of spermatic funicle. Funicle (testicular) torsion is a surgical emergency requiring prompt recognition and treatment to avoid testis damage. In early stage gray scale fails to show any abnormality and only colour-Doppler can recognise absent perfusion in both epididymis and didimis (fig.17), (fig.18), (fig.19), (fig.20), (fig.21). Marked asymmetry in vascularity between symptomatic and asymptomatic testis should also be regarded with suspicion. Very early phase torsion, incomplete torsion, spontaneously disappeared torsion, and paediatric torsion may determine colour-Doppler misdiagnosis. In advanced stages extratesticular increased perfusion and testis echotexture changes become evident (fig. 22), (fig.23).
Varicocele is evaluated at different levels, both at rest and during dynamic manoeuvres (fig.24), (fig.25), (fig.26), (fig.27), (fig.28). Pulsed and colour-Doppler analysis is mandatory for varicocele grading.
In traumatic injuries colour-Doppler may help defining traumatised and disruption areas (fig.29), (fig.30). Posttraumatic changes, such as didimis hematoma or scarring are differentiated from tumours because of absent vascularisation.
Cystic lesions are avascular both internally and along their wall (fig.31).
Testicular tumours show variable amount of vascularisation, unrelated to histology, malignancy, or (partially) size. Consequently, colour-Doppler assessment has a limited value in their assessment (fig.32), (fig.33), (fig.34), (fig.35), (fig.36), (fig.37), (fig.38). Nevertheless, differential diagnosis with infarction and focal chronic, inflammatory and granulomatous processes is boosted by colour-Doppler addition (because of usual absence of vascularisation in nontumoral disorders). Diffuse, infiltrating tumour processes, such as those related to haematological malignancies are associated with diffuse hypervascularisation (to be differentiated from acute inflammation).