- Being aware of the existence of artifactual filing defects that simulate IVC thrombosis, and knowing how to overtake these technical difficulties, is very useful to prevent misdiagnosis and unnecessary investigations.
- It is of utmost importance to be familiarized with the possible causes of IVC thrombosis, so the radiologist may look for them and give the necessary information to the management of the patient.
How to detect and avoid artifactual filling defects
Flow artifacts:
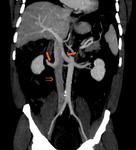
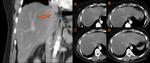
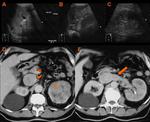
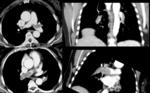
Ø The most common filling defect is due to an artifactual incident caused by the mixture of unopacified blood from the lower extremity with enhanced blood from the renal veins. This pseudothrombosis phenomenon usually occurs in the CT venous phase, which is a CT sequence commonly used for others purposes. (Fig 1)
- ü The use of a delayed phase, in which adequate time has passed for homogeneous venous opacification, is needed when venous thrombosis is suspected. Some authors recommend a scanning delay of 70-90 seconds and others a 180 s. The delay phase will most of the times clarify the artifactual nature of this finding.
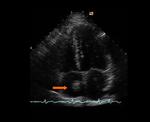
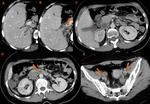
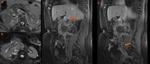
Ø Right heart failure or rapid contrast injection rate may promote a laminar reflux of the opacified blood from the right atrium into the IVC and hepatic veins, resulting in the same pseudothrombosis appearance. (Fig 2).
Ø In MRI, flow artifacts also occur. Gradient echo images are acquired more rapidly, allowing shorter examination times, and for this reason, is the preferred noncontrast technique. However, at the confluence of the vessels, like the confluence of the renal veins, turbulent flow may loose signal intensity, giving a false thrombus appearance. A sub-acute thrombus can be hyperintense, therefore being confused with normal flow. In spin-echo images, slow flow may also acquire intraluminal signal that can mimic a thrombus.
- üA combination of spin-echo and gradient echo images increase the diagnostic accuracy, helping to determine whether ambiguous patterns of intravascular signal intensity represent a patent or thrombosed vessel. Additionally, the administration of an intravenous contrast (gadolinium chelate) may also be a useful tool.
Pseudolipoma of the IVC:
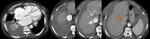
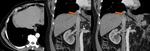
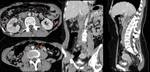
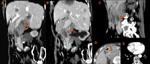
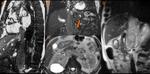
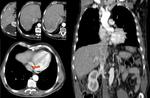
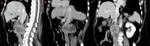
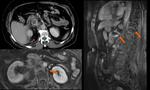
Ø Pericaval fat collections are typically observed medially and adjacent to the hepatic portion of the IVC, near the hepatic venous confluence. In the axial plane, this fat collection may mimic an intracaval lesion (pseudolipoma). It has been described that it occurs in 0,5% of adults undergoing to abdominal CT. This pseudolesion occurs due to a partial volume artifact, giving the false impression of being endoluminal.
Ø An acute angulation and narrowing of the subdiaphragmatic IVC, and chronic liver disease (due to the shrunken right hepatic lobe tilting the IVC), have been described as possible related factors to the existence of these pericaval fat deposits.
- ü Coronal reformatted CT images may clarify the extra-luminal nature of the lesion. (Fig 3 and Fig 4)
Ø In this location, the major differential diagnose of a fat mass is with an extension of a renal angiomyolipoma.
Causes of IVC thrombosis Table1
A - Non tumoral causes
- This type of causes represent the majority of the cases.
A.1. Bland thrombus
Ø It can be related to hypercoaguble state, venous stasis, vessel injury or foreign body.
Ø Usually it is a filling defect that can slightly augment the lumen vessel but it doesn’t affect much its normal morphology.
- The patient history may give important clues (immobilization, etc). It results more often from spread of deep venous thrombosis from lower extremities. Other causes should be looked for and, when possible, excluded.
Ø The expansion of endovascular technology has led to increase recognition of iatrogenic IVC thrombosis. Interventional procedures more related with IVC thrombosis are hepatic transplantation, dialysis access, femoral venous catheters, pacemaker wires and IVC filters.
Ø Case 1:
- We report a case of a 38 year old female patient, without relevant medical history, only medicated with oral contraceptive. She started with lumbar pain and some days after with bilateral lower extremity swelling.
- A CT scan was made and revealed an extensive IVC thrombosis associated with right supra-hepatic vein and left renal vein thrombosis. The prothrombotic and immunological studies were negative. The patient was treated with anticoagulant therapy. (Fig 5 and Fig 6)
A.2. Extrinsic compression
Ø Many conditions may be responsible for extrinsic compression of the IVC that generates turbulent flow and venous stasis, facilitating thrombus formation.
- Retroperitoneal lymphadenopathies are the most common cause (metastatic disease, lymphoma or granulomatous disease).
- Hepatic, renal, adrenal or pancreatic masses can also diminish IVC lumen and also desmoplastic reaction.
- Other causes are: hepatomegaly; hepatic abscesses; polycystic renal disease; aortic abdominal aneurysm; retroperitoneal fibrosis, hematomas or neoplasm.
Ø Case 2:
- To document this group of causes we chose a case of a woman with 63 years old with a history of cecum carcinoma with pulmonary, hepatic and retroperitoneal lymph node metastases.
- The multiple retroperitoneal lymphadenopathies diminished and laminated the IVC lumen. A thrombus in the middle IVC segment was visualized and concomitant pulmonary thromboembolism was also detected although the patient was asymptomatic. (Fig 7)
A.3. Congenital anomalies
Ø Congenital anomalies of the IVC (double IVC, left IVC, interrupted IVC with azygos/hemiazygos continuation, and others) have been associated with thrombosis of the inferior vena cava, specifically in young patients with bilateral deep venous thrombosis.
A.4. Obliterative Hepatocavopathy
(Membranous obstruction of the IVC)
Ø In this entity, the hepatic segment of the IVC is obstructed with a fibrous membrane or maybe replaced by a cordlike structure. This is a common cause of chronic Budd-Chiari syndrome in Asia and South Africa. It’s pathogenesis had been thought to be congenital, however many authors suggest that this “membrane” may be an outcome of recurrent thrombosis.
B - Tumoral causes
- Unless the patient is surgical treatable and the resection is performed, a tumoral thrombus is a severe medical condition with poor prognosis. It may be a primary (intrinsic) or secondary tumoral thrombus.
B.1. Secondary tumoral extension/invasion of the IVC
B.1.1. Renal cell carcinoma
Ø Tumoral extension of the IVC is usually related with renal cell carcinoma, so the kidneys should always be carefully observed.
Ø Spread of the tumor into the IVC is found in 4-10% of patients and is more common with right-sided lesions. The extension into the renal vein alone occurs in 23% of the patients. Direct continuity of the thrombus with the renal tumor is highly suggestive of tumoral extension. Kallman et all, describe that the extension of the renal cell carcinoma to or beyond the distal renal vein was not seen in tumors smaller than 4,5 cm.
Ø If tumoral spread within the IVC is identified, precise delineation of the superior extension of the thrombus is essential to plan the optimal surgical strategy for thrombectomy and minimize the risk of intraoperative tumoral embolism.
- Infra-hepatic level → abdominal incision.
- Retro-hepatic level → right toraco-abdominal approach.
- Supra-diaphragmatic level or right atrium → requires cardiopulmonary bypass.
Ø MDCT has an accuracy rate of 78-93% in predicting the superior extension of the tumoral thrombus, in patients with renal cell carcinoma. Echocardiography, particulary by transesophageal approach, is also of great value for detection of right atrium extension and also as an intra-operative tool.
Ø Usually the tumoral thrombus is intra-luminal and show little tendency to infiltrate the venous wall, and so, it is justified the surgical resection with curative intent.
- For Yoshihiko Tsuji et all, the surgical prognosis in patients with renal cell carcinoma extending into the vena cava was determined by the staging of the tumor, especially lymph node status, and not by the level of tumor thrombus. Others consider the prognostic significance of the level of the tumor thrombus a controversial item and that supradiaphragmatic IVC or right atrium tumor extension is associated with increased morbidity and mortality.
B.1.2. Other malignances may extend directly into the IVC:
Ø Hepatocellular carcinoma typically invades the portal veins, although in some cases may invade the hepatic veins and spread into the IVC (less than 2%).
Ø Adrenal cortical carcinoma, germ cell testicular tumor, retroperitoneal tumors (including leiomyosarcoma), pancreatic carcinoma and Wilms´ tumor in children are others cancers that may spread to the IVC.
Ø Case 3:
- We report a case of an asymptomatic 72 year old man that during a routine transtoracic echocardiogram a cardiac mass in the right atrium was identified (Fig 8 and Fig 9). Transesophageal echocardiogram was also performed (Fig 10). The extension of the cardiac mass into the IVC was also detected. The clinical suspicion of a renal tumor was promptly taken in consideration and the additional investigation was performed. Some days after, the patient started with hematuria. A left renal tumor was diagnosed with left renal vein, IVC and right atrium involvement explaining the echocardiographic finding. (Fig 11 and Fig 12)
- The patient was submitted left nephrectomy with splenectomy and removal right atrium and IVC thrombi. Segmental recession of the IVC was also performed. The presence of a renal tumor was confirmed (clear cell carcinoma), as well as the tumoral nature of the thrombus. A CT follow-up exam showed progression of the disease. (Fig 13)
B.2. Primary tumors of the IVC
- Primary IVC tumors are exceedingly rare. They can be divided in Leiomyoma, leiomyosarcoma or endothelioma.
B.2.1. Leiomyosarcoma
Ø Leiomyosarcoma is the most common primary malignancy in the IVC and has a poor prognosis, compared with the leiomyosarcomas of other locations. A review of the world literature in 1996 revealed 218 cases.
Ø Leiomyosarcoma affects more females (80%), in their fifth and sixth decades of life. Typically it remains asymptomatic until the tumor becomes a large mass, that can have heterogeneous enhancement and may be lobulated and with cystic areas.
Ø According to it’s location, it can be divided into 3 Segments.
- Segment I refers to the level below the renal veins.
- Segment II is between the renal veins and the level of the hepatic veins – tumors affecting this segment are more frequent and are associated with a slightly better prognosis.
- Segment III is above the hepatic veins and may extend to the right atrium.
Ø Tumors can be classified with predominantly intraluminal or extraluminal growth (two thirds of the cases).
- The origin of large tumors with dominant extraluminal growth may be difficult to ascertain. Percutaneous biopsy may be of some value, with the identification of the histological subtype of tumor, but the organ of origin cannot be determined.
Ø Radical resection, when feasible, is the best form of treatment. The 5-year survival with curative treatment is only 28%.
Ø Case 4:
- To illustrate the most IVC intrinsic tumor we present a case of a 59 year old woman that started with lumbar pain with progressive intensity. Three weeks later, she felt a sudden worsening of the lumbar pain associated with dyspnea and retrosternal discomfort and she lost consciousness.
- A CT examination was performed. A large IVC mass and an extensive pulmonary thromboembolism were detected. (Fig 14 and Fig 15). A MRI study was also performed. (Fig 16). Collateral circulation was documented (Fig 17).
- CT guided biopsy was performed and the histological exam showed necrotic tissue and some isolated cells that revealed a mesenchymal tumor origin, compatible with a sarcoma. The patient wasn't submitted to surgery. Once the mass is centred in the IVC we considered that the present case is a vascular leiomyosarcoma from the IVC and not a retroperitoneal sarcoma invading the IVC.