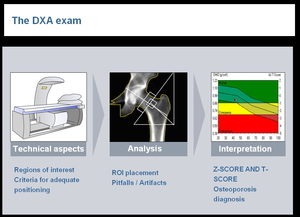
Fig.: DXA Exam steps
1. TECHNICAL ASPECTS
a. REGIONS OF INTEREST
Central DXA measurements should be performed on lumbar spine and proximal femur in all adult patients. Two regions should be analysed, so if one of those is not eligible the forearm is scanned.
The image obtained should include the area of interest, exceeding the superior and inferior limits, in order to be sure that the complete anatomical region is scanned.
i. LUMBAR SPINE
The AP lumbar spine includes vertebral bodies L1 through L4. Altered vertebrae should be excluded from the analysis, but if less than two vertebral bodies may be analysed, another region should be scanned (Figure 2).
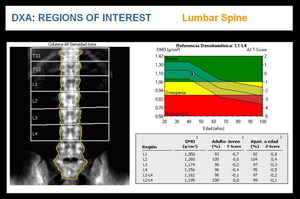
Fig.
ii. PROXIMAL FEMUR
Either hip may be used.
The most important regions are Total hip and Femoral neck. The lowest data of those areas is used for diagnosis (Figure 3)

Fig.
iii. FOREARM
It should be used when hip or spine cannot be measured or interpreted, and with hyperparathyroidism or very obese patients.
The distal one-third radius (33% radius) of the non-dominant forearm is the region of choice due to its active metabolic behaviour. BMD measurements can also be made in the ultradistal and distal areas of the radius (Figure 4).
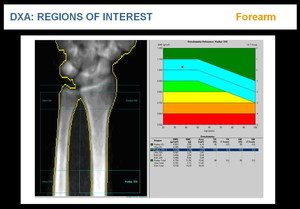
Fig.
b. CRITERIA FOR ADEQUATE POSITIONING
Careful patient positioning is essential in order to optimize BMD measurement.
i.LUMBAR SPINE
The patient is placed in supine position with hips and knees flexed over a support in order to reduce spine lordosis
Image should include D12 and ribs, L5 and iliac bone, and the spine should be straight and centred (Figure 5, Figure 6)

Fig.

Fig.
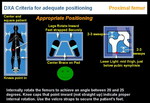
ii.PROXIMAL FEMUR
The patient is placed supine. The leg is internally rotated (15-30- degree rotation) and slightly abducted to keep the femur axis straight.
Image should include complete femoral head and at least one cetimeter under the lesser trochanter, which should not be seen. The femoral axis should be straight (Figure 7).

Fig.
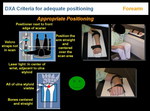
iii.FOREARM
The patient sits beside the exploration table, with the forearm resting on the table, pronated hand and usually with a restraining strap
Image should include 2 cm of diafisis over one-third of the forearm and part of the carpal bones. The axis should be straight and centred (Figure 8, Figure 9)

Fig.

Fig.
2. ANALYSIS
A detailed assessment should include correct placement of ROI and detection of pitfalls
a. ROI PLACEMENT.
ROIs should be placed in the correct area and images assessed for patient movement.
Sometimes plain radiographs are necessary to determine which are the vertebral bodies (Figure 10).

Fig.
Care should be taken in hip images to avoid including bones different from femur (such as ischion) in the ROI (Figure 11).

Fig.
b.PITFALLS
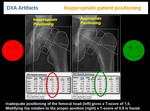
i. INADEQUATE PATIENT POSITIONING
The most important source of false BMD measurement and lack of reproducibility is inadequate patient positioning. (Figure 12).

Fig.
ii. ARTIFACTS
The image should be assessed in search of artifacts to avoid false interpretation, but also lesions previously not diagnosed may be found.
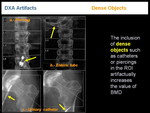
- DENSE OBJECTS
The inclusion of dense objects such as catheters or piercings in the ROI artifactually increases the value of BMD. They should be removed from the area to be scanned when it is possible, or if it is not possible, the area should be excluded from analysis (Figure 13).

Fig.
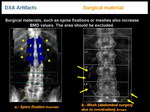
- SURGICAL MATERIAL
Surgical materials, such as spine fixations or meshes also increase BMD values. The area should be excluded (Figure 14).

Fig.
-CONTRAST MEDIA
Artifacts due to retained contrast agents from previous examinations may also appear. The patient should always be asked for barium examination in the previous days in order to postpone DXA. If it is performed, the scan should be repeated after elimination of the contrast agent or if that is not possible the area should be excluded from the analysis (Figure 15).
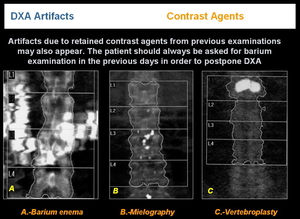
Fig.
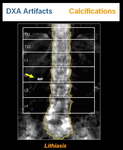
- CALCIFICATIONS
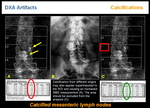
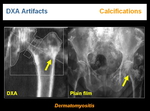
Calcified lesions may appear anywhere in the image, sometimes not affecting the analysis, such as myomas (Figure 16) or lithiasis (Figure 17). Calcification from different origins may also appear superimposed to the ROI and causing an increased BMD measurement. The area should be excluded from the analysis (Figure 18).

Fig.
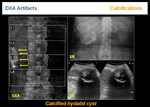
Hydatid cysts (Figure 19), lymph nodes (Figure 18)and dermatomyositis (Figure 20) are typical examples.
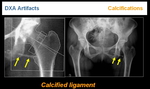
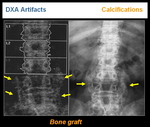
Other examples are calcified ligaments (Figure 21) or bone graft (Figure 22)
iii.DISORDERS
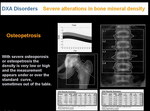
-SEVERE ALTERATIONS IN BONE MINERAL DENSITY
When severe osteoporosis is present DXA scan may mimic a lytic lesion (an area of “unseen” bone, or detect only the highest BMD area (Figure 23).

Fig.
With severe osteoporosis or osteopetrosis the density is very low or high and the measurement appears under or over the standard curve, sometimes out of the table (Figure 24).

Fig.
-OSTEOARTHROSIS
In elderly patients it is a frequent cause of artifactually increased BMD, specially in the spine. Osteoarthrosis is a degenerative entity which causes morphologic changes in the affected area. Osteophytes appear as bone growths and vertebral end-plate reaction to a degenerative disc may also be seen (Figure 25)
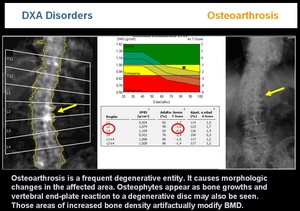
Fig.
-FRACTURES
Fractures cause an alteration in osseous structure which modifies bone mineral density measurement. Sometimes DXA scan allows detection of the fracture. Fractured vertebrae should be excluded from the analysis (Figura 26)
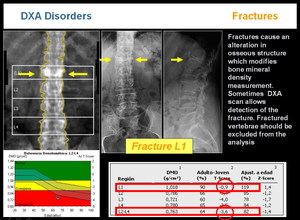
Fig.
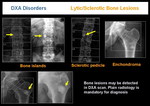
-LYTIC OR SCLEROTIC BONE LESIONS
Bone lesions may be detected in DXA scan. Plain radiology is mandatory for diagnosis. Metastasis, lymphoma, bone islands, Paget's disease, hemangiomas, may be found (Figure 27).

Fig.
- DIFFUSE DISEASES
Diffuse diseases modify osseous structure. The image on DXA scans resembles that seen on plain radiographs (Figure 28).

Fig.
3. INTERPRETATION
a. Z-SCORE AND T-SCORE.
Z-score is obtained comparing the patient´s BMD with healthy population of the same ethnicity, sex, and age
T-score is obtained comparing the patient´s BMD with young adults of the same ethnicity and age
b. DIAGNOSIS OF OSTEOPOROSIS
POSTMENOPAUSAL WOMEN AND MEN AGE 50 AND OLDER
The diagnosis of osteoporosis according to WHO (World Health Organization) is based on the number of SD (standard deviation) values that the patient´s BMD value differs from the mean BMD of a young-adult reference population (T-score) (Table 1 )
The WHO classification is used:
Normal=T-score -1,0 or above
Osteopenia= T-score between -1 and-2,5
Osteoporosis= T-score -2,5 or below

Fig.
PREMENOPAUSAL WOMEN AND MEN YOUNGER THAN 50
Z-scores should be used (comparing with the same age) and osteoporosis should not be diagnosed only with densitometric criteria.
With Z-score below -2 the diagnosis is “below the expected range for age”
CHILDREN AND TEENAGERS (UNDER 20 YR)
Z-scores should be used (comparing with the same age) and osteoporosis should not be diagnosed relying only on DXA criteria.
If the Z-score is below -2, the appropriate report is “low bone density for chronological age”