Type:
Educational Exhibit
Keywords:
Breast, Ultrasound
Authors:
O. Bueno Zamora, F. J. Olcoz Monreal, E. GarcĂa Laborda, ďż˝. Lancharro Zapata, A. Paniagua Bravo; Madrid/ES
DOI:
10.1594/ecr2010/C-0424
Background
Despite efforts to increase the rate of conservative breast surgery, modified radical mastectomy is still considered to be the primary surgical treatment method in patients who have multicentric tumors or extensive ductal carcinoma in situ, for those in whom tumor-free margins cannot be achieved with lumpectomy alone or when there are contraindications to radiation therapy. The procedure involves removal of the breast and the pectoralis minor muscle but preservation of the pectoralis major muscle.
The reported local failure following mastectomy ranges from 5% to 27%. Around 30% of local recurrences occur within the first 5 years, and 25-35% cause significant morbidity. Early diagnosis is important for prognosis since only 30% of local recurrences have distant metastasis at the time of diagnosis [1].Prognostic factors appearing to affect the survival of patients with local recurrence include T status of the primary tumor, presence of axillary node involvement and the location, size and number of the recurrent tumors [2].
Follow-up procedures after mastectomy include yearly mammogram of the contralateral residual breast and periodic physical examination at the surgical site [3]. Imaging procedures in asymptomatic patients are not recommended. However, physical examination is relatively weak in the early diagnosis of local recurrence in deeply located lesions [4], and US has demonstrated to be more sensitive than palpation and mammography for the detection of local recurrence at the mastectomy site [1,5,6]. US is also ideally suited for multiplannar scannining in difficult anatomic landmarks such as the thoracic and the axillary scars.
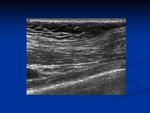
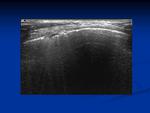
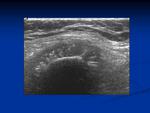
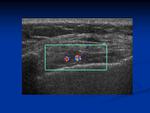
Normal anatomic thoracic structures following mastectomy include skin, subcutaneous fatty tissue, pectoral and intercostal muscles, ribs and costal cartilages (Figs. 1-4). The pleura and internal mammary vessels can also be readily identified (Fig. 5). The axilla, paraesternal and supraclavicular areas should also be routinely scrutinized when lymph node involvement is suspected.