Table of content and key findings
1. Polyarteritis Nodosa
Aneurysms or occlusions of the visceral arteries (especially renal artery)
2. Microscopic Polyangiitis
MPO-ANCA, Necrotizing glomerulonephritis
3. Henoch–Schönlein purpura (anaphylactoid purpura)
Deposition of IgA antibody, Purpura
4. Takayasu arteritis
Granulomatous inflammation affecting the aorta and its major branches, pulseless disease
5. IgG4-related periaortitis
Idiopathic sclerosing lesion, Elevated serum IgG4 concentration
6. Collagen diseases (Behçet disease)
Vascular Behçet (vasculitis of the vasa vasorum of the large arteries)
1. Polyarteritis Nodosa
Definition
Polyarteritis nodosa (PAN) is a representative disease of abdominal vasculitis. Pathologically it is a fibrinoid necrotizing vasculitis that mainly involves small and medium-sized arteries such as main branches of abdominal aorta, especially small arteries in kidney. Multiple aneurysm formation and arterial stenosis/occlusion are characteristic findings in PAN. The classic pathological description of necrotizing arteritis was published by Kussmaul and Maier in 1866 (3). They reported the clinical and autopsy findings in a patient with numerous nodules in small- and medium-sized systemic arteries. Histological examination revealed inflammation and necrosis of muscular arteries at the sites of nodule formation. They called the disease "periarteritis nodosa." Afterward because its transmural rather than perivascular nature of the inflammatory lesions was revealed, the term of "polyarteritis nodosa" (PAN) has become currently used widely for these type of arteritis. Furthermore, the Chapel Hill consensus conference on the nomenclature of vasculitis in 1993 adopted the view that the PAN and "microscopic polyarteritis" were distinct categories of vasculitis. Therefore the “classic PAN” was defined as necrotizing inflammation of medium-sized or small arteries without glomerulonephritis or vasculitis in arterioles, capillaries or venules.
Symptoms
Patients usually present with vague signs and symptoms such as fever, weight loss, weakness, malaise, headache, arthralgia and myalgia. Specific complaints related to vascular involvement within particular organ systems include renal failure or hypertension in renal involvement and intestinal hemorrhage or necrosis in intestinal involvement. In other regions, peripheral polyneuropathy is frequently seen in more than half of the PAN patients. Cerebral infarctions also occur in 10-20% of the cases (4). Myocardial infarction or respiratory system involvement is rare.
Diagnosis and imaging findings
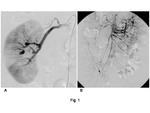
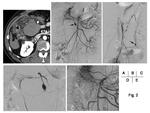
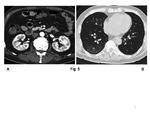
The diagnosis of PAN is made on the basis of clinical findings, histological and angiographic findings (Table 2). Therefore it is important to diagnose by angiographic findings such as multiple small aneurysms up to 1 cm in diameter, multiple steno-occlusive change, or irregularity within the renal and mesenteric vasculature (Fig. 1) (5). Several reports demonstrated the usefulness of CT angiography or MR angiography for detecting the PAN lesions (6, 7). However, on the other hand, there is a report suggesting the difficulty on differentiation between PAN and pyelonephritis on CT and MR imaging (8). Therefore, when PAN is suspected, angiography should be performed to make a correct diagnosis at present. Differential diagnosis on angiography includes the septic emboli and the mycotic aneurysms associated with infectious endocarditis and the segmental arterial mediolysis (SAM) which shows multiple small aneurysm or steno-occlusive change (Fig. 2) (9). Angiographic finding is not always pathognomonic for PAN, therefore, a comprehensive evaluation of radiologic findings, clinical symptoms, and pathologic findings (fibrinoid necrotizing vasculitis) are often required for diagnosis.
Treatment
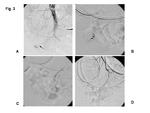
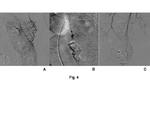
If the patient is left untreated, the disease is fatal in most instances in association with renal failure, gastrointestinal complications such as bowel infarction or perforation, or cardiovascular causes. The primary treatment of PAN is systemic therapy with corticosteroids and immunosuppressive agent. Although PAN is usually associated with multiple aneurysms in visceral artery, transarterial embolization is not indicated unless they rupture. Intestinal hemorrhage or peritoneal or retroperitoneal hemorrhage should be treated by embolization. The embolization using liquid materials like n-butyl-2-cyanoacrylate (NBCA) has been recently presented, in addition to classical techniques including hemostasis by intraarterial injection of vasoconstrictor of vasopressin, the embolization using gelatin sponge or polyvinyl alcohol particles, and coils (10.11) (Fig. 3, Fig.4). Intraarterial injection of vasoconstrictor is rarely applied now because recent advances with microcatheter or micro guidewire have enabled us superselective embolization at the hemorrhagic point.
It is important to know the size and angioarchitecture of the injured artery for selection of an adequate technique of embolization of a visceral pseudoaneurysm in PAN. Since gastrointestinal bleedings usually occur from microaneurysms of vasa recta which is terminal artery of intestine, for getting sure hemostasis it is necessary to occlude the artery completely. d'Othee et al reported 19 patients with acute lower GI bleeding which was treated by microcoil embolization. According to their report, technical success was obtained in 17 patients (89%) and clinical success was complete in 13 patients (68%), and two patients experienced colonic ischemia (11%) required colectomy (12). No late rebleeding in embolized area was presented. On the other hand, Loffroy et al reported that the procedural success rate was 95% and the clinical success rate was 77.2% without any major procedure-related complications. Two factors were independent predictors of embolization failure: coagulation disorders and the use of coils as the only embolic agent (13). Although it cannot be generalized because the embolization methods are different according to the institutions or the case itself, coil embolization at the proximal site of the marginal artery can have a risk to of rebleeding. NBCA would be a useful embolic agent because which can achieve vascular occlusion instantly regardless of coagulability of the patients (11). However, regional embolization including plural marginal arteries from the proximal side with NBCA has a higher risk of bowel necrosis; therefore it should be done with supposing the later urgent intestinal resection. Rupture of the aneurysm located proximal to the marginal artery causes mesenteric and/or intraperitoneal hemorrhage. The standard treatment strategy of these aneurysms is to occlude both proximal and distal side of the aneurysm (trapping). It is mostly recommended to introduce a microcatheter to the distal side of the aneurysm and embolizing with coils from the distal to the proximal side. When a microcatheter is difficultly advanced beyond the aneurysm safely, embolization with NBCA can be applied for complete occlusion of the aneurysm. Though, its indication should be carefully considered due to intestinal necrosis as described above. In addition, vasculitis is often accompanied with multiple vasoconstriction / occlusion as well as the aneurysms, and these stenoocclusive changes of the collateral arteries after embolization can increase the risk of postoperative intestinal ischemia. Therefore, stenoocclusive changes of the potential collateral pathway of the targeted artery should be also taken into a consideration on choosing the embolization techniques (Fig. 2). Because the collateral supply will not develop after the embolization in the peripheral renal artery distal than the segmental branches, it is assumed that even proximal embolization is enough in the case of the hemorrhage from the renal aneurysms at the peripheral branches.
2. Microscopic Polyangiitis
Definition
As described in the previous section, microscopic polyangiitis (MPA) which was separated from classic PAN is a necrotizing vasculitis affecting small vessels (i.e., capillaries, venules, or arterioles). Rapidly progressive glomerulonephritis (seen in 90% of cases) and pulmonary capillaritis are particularly common in MPA. MPA is one of the ANCA-associated disease as well as Wegener granulomatosis and Churg-Strauss syndrome. Especially myeloperoxidase-specific ANCA (MPO-ANCA) is highly present in the majority of cases.
Symptoms
Clinical manifestations include fever, general fatigue, weight loss and purpura. Numbness or dyskinesia is sometimes presented, which is caused by the polyneuritis. Renal lesions such as proteinuria, acute renal dysfunction, and hypertension often occur. Pulmonary manifestations include alveolar hemorrhage and interstitial pneumonia caused by capillaritis. Some reports demonstrate intestinal edema, ulcer, and cholecystitis.
Diagnosis and imaging findings
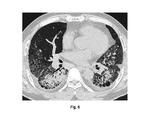
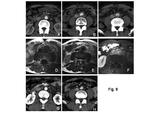
Clinical manifestations (especially lung and kidney involvement), histological findings such as necrotizing vasculitis affecting small vessels and necrotizing crescentic glomerulonephritis of kidney, and positive MPO-ANCA are important findings for definite diagnosis of MPA. Necrotizing glomerulonephritis is the major characteristic of the disease which rarely demonstrates abnormal findings on abdominal CT or MRI. In case of the disease affecting medium-sized arteries, contrast defects at peripheral renal cortex or microaneurysms may be observed (Fig. 5) (14). Pulmonary features of the disease usually demonstrate the imaging findings of idiopathic interstitial fibrosis (IPF). When the pulmonary hemorrhage occurs, CT and chest radiograph show ground glass opacity or infiltration (Fig. 6) (15, 16). Although imaging findings of the MPA cannot be a conclusive factor like PAN, the MPA should be considered as one of the differential diagnosis when radiologists find the IPF with renal dysfunction.
Treatment
It is rare but there are a few cases presenting renal or intestinal hemorrhage which needs to be treated by interventional techniques (14). Other ANCA-associated vasculitis such as Wegener granulomatosis and Churg-Strauss syndrome occasionally cause abdominal vasculitis.
3. Henoch–Schönlein purpura (anaphylactoid purpura)
Definition
Henoch–Schönlein purpura (HSP) is a nonthrombocytopenic purpura which occurs mainly in children under 10 years of age, and is characterized by deposition of immune complexes containing the antibody IgA. Purpura, arthritis and abdominal pain are known as the classic triad of HSP. Of half of affected patients, HSP usually follows an upper respiratory tract infection. Histologically, the features are the infiltration of the inflammatory cells around small vessels and the deposition of IgA antibodies in the wall of blood vessels.
Symtoms
Gastrointestinal symptoms include intestinal edema, abdominal pain, and gastrointestinal hemorrhage. About 10-50 percent of the patients have evidence of renal involvement. Adults are more likely than children to develop advanced kidney disease which lead to renal failure. Majority of cases are self-limiting and require no treatment. Severe pulmonary involvement such as pulmonary hemorrhage or pulmonary edema was rare, however, it was reported to be fatal complication of HSP (17).
Imaging findings
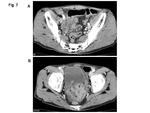
The gastrointestinal manifestations are thought to be related to edema and intramural hemorrhage. Because the imaging findings of HSP demonstrate non-specific enteritis such as bowel wall thickening or ascites, general symptoms and clinical history of the patients are essential in establishing a diagnosis (Fig. 7) (5).
4. Takayasu arteritis
Definition
Takayasu arteritis is a form of granulomatous inflammation affecting the aorta and its major branches which usually occurs in patients younger than 50. It is also known as "pulseless disease" because of marked weakening of the pulses in the upper extremities. It is also associated with fibrous thickening of the aortic arch with narrowing or virtual obliteration of the origins of the great vessels arising in the arch.
Symptoms
Generalized signs and symptoms include malaise, fever, night sweats, arthralgia, and weight loss. Pulses are commonly absent in the involved vessels, particularly the subclavian artery. The diagnosis is confirmed by a characteristic arteriographic pattern that includes irregular vessel walls, stenosis, poststenotic dilatation, aneurysm formation, occlusion, and evidence of increased collateral circulation (5).
Treatment
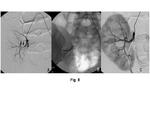
Percutaneous transluminal angioplasty (PTA) for renal artery stenosis caused by Takayasu arteritis is usually performed when the pathological stage of the disease demonstrates fibrous thickening. Generally the criteria for selections of patients for angioplasty are severe hypertension uncontrolled by single-drug therapy in addition to angiographic evidence of at least 70% stenosis of the renal artery with a pressure gradient of more than 20 mmHg. Sharma et al reported their results of balloon PTA in treating 33 stenoses in 20 patients (18). The procedure was technically successful in 85% and clinical cure was achieved in 82 % of these patients. Restenosis was observed in 21 % at follow up (mean 8 months after treatment). They also described the cases which showed severe and tight stenosis at the proximal of the renal artery, making the entry of the balloon catheter extremely difficult. Tyagi et al attempted PTA for renovascular hypertension in 35 children including 31 cases of Takayasu arteritis. They reported technical success rate was shown in 91.5%, and restenosis was in 25.8 % at 4 to 72 months (mean 23.1 months) follow-up (19). Technical success rate has been improved by recent advances of the catheter or guide wire. Especially PTA using stent placement has achieved high technical success rate. However, the problem of restenosis still remains. The cases which cannot get effective result from PTA or the cases showing repeated restenosis are indication for autotransplantation or bypass operation using venous graft. Stenosis at anastomotic site after those operations would also be a good indication for renal PTA (Fig. 8).
5. IgG4-related periaortitis
Definition
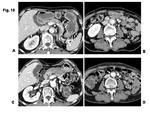
Recently, relationship between IgG4 and idiopathic sclerosing lesions has attracted much attention (20, 21). IgG4-related sclerosing disease is a systemic disease characterized by a fibro-inflammatory tissue which develops around the abdominal aorta and the iliac arteries, and spreads into the surrounding retroperitoneum with elevated serum IgG4 concentrations and extensive infiltration of IgG4-positive plasma cells around the vessels (Fig. 9). Retroperitoneal fibrosis can occur as part of this disease. Although several reports support the theory that it could result from a local inflammatory reaction to antigens in the atherosclerotic plaques of the abdominal aorta, the etiology of this new entity is still unclear. Retroperitoneal involvement often causes hydronephrosis. Inflammatory abdominal aortic aneurysm (IAAA) could be one of the manifestations of IgG4-related disease.
Treatment
Steroid therapy has a favorable effect on IgG4-related sclerosing disease. Percutaneous nephrostomy or ureterostomy will be performed for severe hydronephrosis. Endovascular aneurysm repair of IAAA is reported in patients at high risk for a surgical procedure (22). It is necessary to know that the disease is frequently complicated with the collagen disease such as systemic lupus erythematosus, Sjogren syndrome, and autoimmune pancreatitis, other systemic vasculitis and malignant neoplasms (Fig. 10).
6. Collagen diseases (Behçet disease)
Definition
Collagen disease such as malignant rheumatoid arthritis, SLE, dermatomyositis also cause vasculitis in kidney or intestinal tract frequently(Fig. 3). Behçet syndrome is an inflammatory disorder involving multiple organ systems with well-known clinical manifestations including recurrent aphthous stomatitis, genital ulceration, and relapsing uveitis, skin lesions, arthritis, and neurologic and gastrointestinal involvement. The etiology of the disease is still unclear. Vascular-Behçet syndrome appears in approximately 10% of the patients and manifests as arterial occlusion, aneurysm, venous occlusion, and varices. Although vascular involvement in Behçet disease is not frequent, it increases mortality to 20% (23). In vascular involvement, arterial lesions are less frequent than venous lesions and usually develop in the aorta and pulmonary artery and in their major branches. Histologically, the vascular manifestation is a vasculitis of the vasa vasorum of the large arteries and veins that causes wall compromise, thrombosis, obstruction, and aneurysm formation. Perforation of the arterial wall due to obliterative endarteritis of the vasa vasorum may result in aneurysm formation or rupture. The most common site of aneurysm formation is the abdominal aorta followed by the pulmonary, femoral, and subclavian arteries (24).
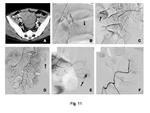
Gastrointestinal manifestation has been reported to be involved in 15%-65% of patients with Behçet syndrome (25); the usual site is the ileocecal area, especially the terminal ileum. The hallmark of Behçet syndrome is the presence of large, deeply penetrating ulcerations of the submucosa, muscle layer, or entire intestinal wall. As a result, a high prevalence of complications such as perforation, hemorrhage, fistula, and peritonitis has been reported. Massive gastrointestinal bleeding is usually from the mucosal ulcerative lesions and rarely occurs from the rupture of visceral arterial aneurysm (Fig. 11) (25).
Treatment
In addition to medical therapy including anti-inflammatory and immunosuppressive agents, the management of gastrointestinal bleeding involves colonoscopic, angiographic, or surgical therapy, or any combination of these techniques. Selective angiography has proven useful for both the diagnosis and treatment of intestinal bleeding. Interventional radiology play an important role on emergent embolization and its basics regarding the treatment of strategy and techniques are the same as described in the section of PAN. Aneurysms of aorta and large arterial branches are good indications of endovascular stentgraft treatment.