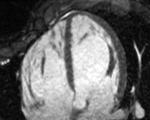
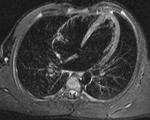
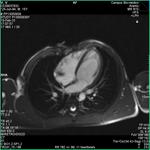
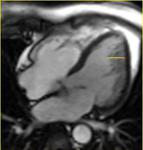
Myocardial non compaction is a condition that is now being defined and is more frequent than expected,
as in the past it has often been misunderstood because of inadequate diagnostic instruments.
The development of echocardiography and highly performing MR sequences allow an accurate study of this condition.
Infact MR allows is now able to define:
- morphology: volume of cardiac chambers;
- cardiac function: total/sectoral contractility
- perfusion: in condition of rest and stress
- late enhancement: necrosis/fibrosis areas.
Echocardiographics criteria for Non-compacted myocardium are:
- Absence of coexistent cardiac anomalies
- Wall left ventricle segmental thickening composed by two layers; uncompacted/compacted myocardium ratio >2:1 in endsystole with wall myocardium thickening;
- Disease main localization in middle-side apical and middle-lower regions of left ventricle;
- In color doppler examination presence of blood flow through deep recesses normally perfused.
Some authors proposed different criteria for MR diagnosis of non-compacted myocardium; Petersen suggested as the main criteria segmental thickening of left ventricle wall composed by two layers; trabeculae/compacted layer ratio > 2,3 in end-diastole; main localization of trabeculae in distal segments,
from anterior wall in clockwise manner.
Jacquier instead proposed other criteria: left ventricle % of trabeculation 3 times higher in NCM (32 +/- 10%) than DCM (11 +/- 4%),
HCM (12 +/- 4%) and healthy patients (12 +/- 5%); trabeculation mass >20% than LV total mass predictive of non-compacted myocardium (sensitivity 93,7% e specificity 93,7%).
Pujadas took into consideration diastolic and systolic disfunction as diagnostic criteria.
Other authors considered also the possibility to evaluate the relative hypoperfusion and myocardic fibrosis.
Considering all these premises,
our image analisys includes the following diagnostic criteria:
- Left ventricle wall segmental thickening composed by two layers;
- trabeculation/compacted layer>2,3 in end-diastole.
- Evaluation of hypoperfusion
- extension of myocardic fibrosis
- main localization in distal segments,
from anterior wall in clockwise.
(Accessory:)
(- LV % of trabeculation 3 times higher in MNC)
(- trabeculation mass>20% of whole LV mass)
In conclusion,
comparing echocardiography and MR examinations in terms of advantages and disadvantages,
we evidence that:
- Echocardiography has low cost,
is more accessible,
doesn't use ionizing radiation,
but is operator-dependant,
sometimes not practicable because of inadequate acoustic window,
it performes a geometric calculation of FE.
- On the other hand,
MR also doesn't use ionizing radiation,
allows perfusion and late enhancement evaluation,
is highly feasible and is reliable in quantification of FEV,
provides panoramic evaluation and contrast resolution,
but is expensive,
has long duration of examination,
and sometimes is controindicated (PMK,
calustrophobia,...).