Tubes,
Line,
Devices and Imaging Findings
Endotracheal Tubes
- Commonly used in early resuscitation
- Usually changed over to tracheostomy if prolonged ventilation support is required.
- ET tube should be between 2 and 4 centimeters above the carina
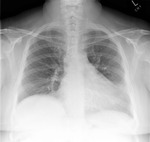
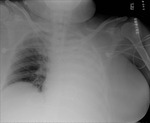
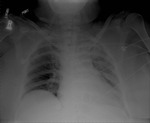
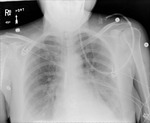
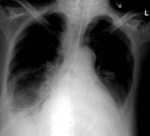
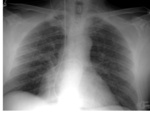
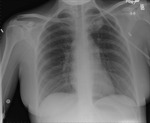
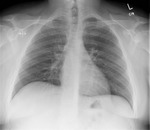
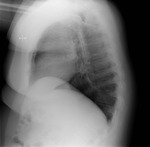
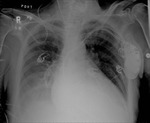
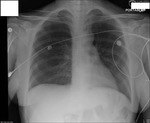
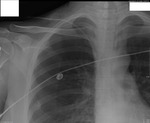
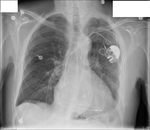
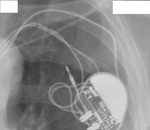
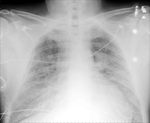
Figures 1-3
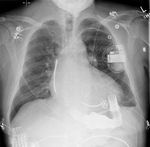
This patient,
who required reintubation after valve replacement and sternotomy (1) initially had the ET tube placed to deep,
leading to collapse of the left lung (2).
Following retraction of the ET tube to correct position,
the left lung re-expanded (3).
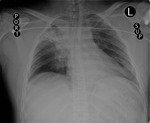
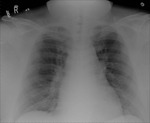
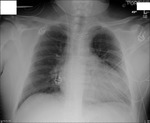
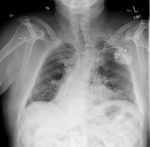
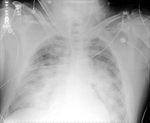
Figure 4
This patient had an intubation with the ET tube entering into the right bronchus intermedius.
Again,
partial lung collapse (of the right upper lobe) resulted.
Note the correctly positioned NG tube into the stomach.
Nasogastric Tubes
- These are used both for deflation and protection of airway tree.
- Feeding tubes appear like NG tubes,
but tend to be of larger caliber and frequently have a metalic tip.
- The normal position should be in a line along the expected course of the esophagus into the stomach (assuming normal anatomy)
Figure 5
This patient has a feeding tube which has recoiled into the esophagus,
and should therefore not be used until proper position is achieved,
as feeding in this location can lead to aspiration.
Figure 6
The NG tube in this patient has inadvertently entered the airways and is located in the right lower lobe bronchus.
Failure to identify this misplacement can result in severe lung injury,
ARDS and death.
Central lines
- There are three main central lines in use: internal jugular vein lines (IJ lines),
percutaneous intravenous central catheters (PICC lines) and Swan Ganz catheters
- The course for the IJ lines should be directly in line with the main venous system into the superior vena cava.
- The course for PICC lines are from the arm through the subclavian vein into the superior vena cava.
They are now often preferred as they are less likely to cause pneumothorax compared to traditional subclavian vein lines.
- The course of Swan Ganz catheters are from internal jugular vein or inferior vena cava,
through the right heart into the main pulmonary artery,
with the tip ideally positioned within the mediastinal contour.
Figure 7
This is a figure demonstrating the appropriate position of an IJ line within the superior vena cava and a Swan Ganz catheter within the right interlobar pulmonary artery.
Figure 8
This demonstrates a Swan Ganz catheter in appropriate position in the right main pulmonary artery.
Figures 9-13
These figures show several misplaced PICC lines,
respectively in the internal jugular vein (9),
coiled in the subclavian vein (10),
within the azygos vein (11 and 12) and too deep into the inferior vena cava (13).
Figure 13
This figure demonstrates a Swan Ganz catheter that is positioned too deep into the right lower lobe pulmonary artery.
The risk here is that with insufflation of the balloon in order to obtain wedge pressure,
pulmonary artery dissection or rupture can occur.
Figures 14 and 15
This patient underwent placement of a subclavian line,
which resulted in a pneumothorax (14).
A zoomed in image clearly outlines the pleural edge (15).
Two-lead pacemakers
- These are the more standard pacemakers
- They require two electrodes to be positioned in the right atrium and right ventricle
Figure 16
This patient had left continuation of the superior vena cava,
and since most pacemakers are placed in the left superior chest,
the electrode wires follow the course of the left subclavian vein to the left superior vena cava,
which drains into the right heart.
Figures 17 and 18
This patient was referred for follow-up of a pacemaker,
and the chest radiograph demonstrated a broken pacemaker lead (18).
The zoomed in image highlights the need for scrutiny,
using a zoomed in approach to check the length of the wire (19).
Biventricular pacemakers
- These pacemakers are required when both ventricles are in need of electrical stimulation
- The require positioning of a total of three electrodes in the right atrium,
right ventricle and the coronary sinus (for pacing of the left ventricle)
Figure 12 shows appropriate placement of a three lead pacemaker.
Aortic Balloon Pump
- These are inserted to support the heart in acute heart failure situations,
usually following myocardial infarction or immediately after cardiac surgery.
- The pump is outside the body,
and connected through a line to a balloon,
which is inflated and deflated in rhythm with the heart.
- There is a metallic marker at the tip of the balloon,
which should be located below the aortic arch.
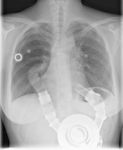
Figures 19 and 20
This patient suffered from acute pulmonary edema due to heart failure of acute onset (19).
A balloon pump was inserted to improve cardiac output (20),
and the patient was also intubated and a NG tube was placed.
Ventricular Assist Device (VAD)
- There are devices specifically to assist the left ventricle and those where both ventricles are supported.
- The devices are used to bridge a heart that is expected to recover (e.g.
myocardiopathy in the context of myocarditis) or where heart transplant is considered.
Figure 21
This patient received a left VAD.
Previous aortic valve replacement and appropriate placements of a biventricular pacemaker and a PICC line are noted.
Figure 22
This patient received a bi VAD.
Notice the central venous access port with a catheter positioned in the superior vena cava.