Discussion
The thoracic cage in infants and young children is inherently plastic,
meaning rib fractures are uncommon in this age group; it takes significant force to fracture the ribs of a healthy infant skeleton.
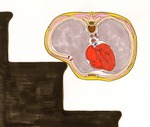
It is possible to fracture anywhere along the length of the rib arc,
as a result of severe accidental (figure 1) or non-accidental trauma,
though when present in a child less than 3 years of age, such fractures are highly predictive of NAI.
It takes less force to fracture a rib,
which is abnormal as a result of an underlying congenital or metabolic disorder.
Rib fractures may be single or multiple,
uni- or bilateral,
depending upon how they have been caused.
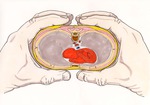
CVJ fractures have been shown in both animal models and through case study reports, to occur as a result of compression or deformation of the rib cage in an antero-posterior direction; for example,
when the chest of an infant is encircled by an adult’s hands (figure 2).
In this position,
forces are generated,
which lever the posterior aspects of the ribs over the adjacent vertebral transverse processes,
resulting in fractures in the region of the rib head and neck,
close to their articulation with the vertebral body.
Similar directional forces can arise if an infant is thrown or slammed face-forwards into a solid surface or object (figure 3),
though would be more likely to be associated with visible bruising over the chest and/or face in these circumstances.
Compared with posterior and lateral rib fractures,
CCJ fractures are much less common,
and reportedly require more force to cause them.
They too can result from antero-posterior compression forces,
where the sternum and costal cartilages are depressed,
leading to maximum tension along the inner aspect of the rib in the region of the CCJ (figure 2),
which explains the CT finding of buckle fractures along the anterior inner rib cortices in three of the study patients.
CCJ fractures may also occur as a consequence of a direct blow to the adjacent chest wall,
in which case they can be associated with intra-thoracic or intra-abdominal organ injuries and visible bruising at the site of impact.
Rib fractures as a consequence of cardio-pulmonary resuscitation (CPR) are much less common in children than in adults (0-2% versus 13-97% respectively).
Dolinak's paper from 2007 commented that CPR-related rib fractures in infants are subtle and are likely to be missed even at autopsy,
unless the parietal pleura is stripped-back and the internal surface of the thorax examined visually and by palpation.
In the 8 children he described with rib fractures secondary to CPR,
the fracture types and location mirrored those found in the present study,
which were attributed to CPR.
That is,
the fractures were anterolateral in location,
were often bilateral and symmetrical,
thereby reflecting the forces imparted to the mid-sternum by chest compressions,
and involved the 2nd-6th ribs.
As in the study population,
many of the fractures Dolinak describes were of the buckle variety,
with little or no associated haemorrhage at the fracture site,
and none could be identified on pre-autopsy chest radiographs.
A 2009 paper by Weber and colleagues echoed Dolinak's findings,
and again stressed the importance of pleural stripping to search for rib fractures during infant autopsies.
Neither Dolinak nor Weber described CCJ fractures in association with CPR.
A literature review on CPR-realted rib fractures in children,
published by Maguire in 2006,
describes only 3 children with rib fractures (one with CCJ and two with mid-clavicular fractures) in 923 children following CPR,
that was performed variably by both trained medical personnel and lay people.
In all 3 cases,
the fractures were multiple and anterior,
but no posterior rib fractures were identified.
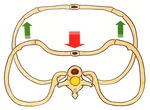
The outlined work from the literature and the current study support the accepted theories describing the biomechanical forces required to fracture the ribs of a young child: when the infant’s back is supported on a firm surface and the chest compressed during CPR (figure 4),
the posterior ribs cannot migrate over their transverse processes and therefore,
do not fracture at the CVJ.
The antero-posterior compressive forces generated can,
however,
cause anterior fractures.
Similarly,
if the child is resuscitated on a soft surface such as a bed,
the chest as a whole is pressed into the soft surface and rib leverage cannot take place,
meaning posterior rib fractures do not occur in these circumstances either.
Only one published study of 12 cases (Wootton-Gorges et al 2008) compares the detection of rib fractures on CT exams to chest radiographs in NAI.
However,
this study differs from the current one,
in that it was retrospective and involved live children,
not all of whom had CT chest examinations; children for whom abdomino-pelvic CT studies had been performed were also included.
The presence or absence of rib fractures was accepted from the initial imaging studies,
and no follow up examinations were performed.
Despite these limitations,
the authors concluded CT was more sensitive than chest radiography for the detection of rib fractures in NAI,
though cautioned it should be used judiciously given the risks of the radiation dose each patient receives.
The current study is both prospective and larger,
comparing chest radiography from skeletal survey examinations with CT chest studies,
using autopsy and histology as the gold standard to detect rib fractures in recently deceased infants,
in whom NAI cannot immediately be discounted.
Radiation risks are not an issue.
Conclusion
The authors recommend post-mortem CT chest examinations be performed alongside skeletal surveys in infants,
whether they are alleged victims of NAI or have been classified initially as SUDI.
This group of infants includes those who are dead upon arrival at hospital or who die in the two-week period before it is possible to obtain follow-up chest radiographs.
NAI is a diagnosis of exclusion.
Rib fractures,
particularly when they are multiple and of different ages are highly suggestive of the diagnosis,
and CVJ fractures are rarely found in any other circumstances.
The conceivable consequences both medico-legally and to any surviving siblings of missing such fractures are huge. Ribs with both definite and suspected fractures should be resected at autopsy to confirm or refute their presence.
Moreover,
the location and type of any fractures seen on the CT study may help to differentiate between those resulting from trauma - be it accidental or non-accidental,
and those occuring subsequent to vigorous CPR.
Acknowledgment: with thanks to Mr Brendan Ellis,
Medical Artist,
Royal Victoria Hospital,
Belfast for providing the diagrams used in producing this poster