From November 2009 to November 2010 we enrolled 167 consecutive patients with a suspicion of prostate cancer (prostate specific antigen greater than 4 ng/ml and/or positive digital rectal examination).
We excluded from the present analysis the patients who underwent a re-biopsy after one or more previous negative sets and the patients who underwent the first set of biopsy for a PSA greater than 20 ng/ml.
All patients were adequately informed about the method of execution of the procedure and its potential complications and were asked to provide a written consent.
Patients were given a fluoroquinolone antibiotic on the day of the procedure and on the 3 following days.
Biopsies were performed in all patients in the left lateral decubitus,
using 18-gauge needles and a biopsy gun,
providing 15 or 22-mm-long tissue cores.
In all cases an anaesthetic block of the peri-prostatic plexus was performed administering 2 ml of 1% Lidocaine at the prostate apex.
All examinations were performed using a Toshiba nemio (Toshiba medical systems,
Japan) unit equipped with a multi-frequency end fire type rectal probe (4-7.5MHz).
12-core TRUS-guided needle biopsy was performed by a single radiologist.
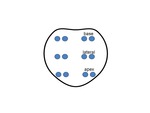
In addition to the standard sextant biopsy technique,
six more biopsy cores were obtained from the lateral peripheral zone (fig.1).
All patients were clinically evaluated 15 days after biopsy to record the complications related to the procedure.
Needle cores were stretched and placed in an independent container in according to the pre-embedding methods of prostate needle biopsy specimens (fig.
2).
Each sampled core has been numbered,
identified by site and prostate lobe.
The core biopsies were distributed in couples on labeled tissue cassettes (fig.3).
Cores were labeled from 1 to 12.
One-way analysis of variance and x2 analysis were used to compare,
respectively,
means and proportions.
Patients were divided into quartiles according to prostate volume: ≤ 30,
30.1-50,
50.1-70 and > 70 cc.
We chose the 12-core scheme as a baseline.
Therefore,
we subtracted one single core per each side of the prostate,
and we calculated the cancer detection rates for each scheme with 10,
8 and 6 cores.
Detection rates of the different schemes were stratified according to the different TRUS estimated prostate volumes.