AGIB.
MDCT examination protocol
No oral contrast material or fluid.
Triphasic CT examination protocol from the diaphragm to the inferior pubic ramus:
Unenhanced scan (low radiation dose).
Arterial phase: bolus triggering starting at 150 HU in proximal aorta.
Portal phase: 70 sec.
after beginning of CM injectionCM at 4 mL/sec,
followed by 50 mL of saline chaser.
120 kVp,
automatic tube current modulation in x,
y,
and z-axes.
64-detector CT scanner (Aquilion 64; Toshiba,
Tokyo,
Japan).
Image analysis (WS): two and three-dimensional (multiplanar,
volume rendered,
maximum intensity projection) reformations,
as needed.
AGIB.
MDCT examination protocol.
Some tips and questions answered
Oral contrast material or other fluid can dilute the extravasated and mask active bleedingUnenhanced scan depicts any pre-existing intraluminal hyperattenuating materialcan be avoided?: - false positive rate can increaseArterial phase: often shows the jet of intraluminal contrast,
whose modification in the portal phase is diagnostic of active bleedingcan be avoided?: - diagnostic reliability can decrease
- your interventional radiologist may need itPortal venous phase: confirms active bleeding and etiologycan be avoided? - we are currently studying the impact of a further reduction of radiation dose on diagnostic accuracy
- any help will be welcome
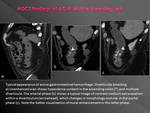
MDCT findings of AGIB
Active bleeding: jetsRecent bleeding: clotsOther signsPitfalls and equivocal findings
MDCT findings of AGIB.
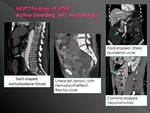
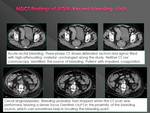
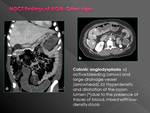
Active bleeding: jets
The likelihood for detection of bleeding correlates to the bleeding velocityMDCT angiography depicts bleeding intensity of 0.5 to 1 ml/min,
comparable to
that reported for conventional angiography
Occasionally,
arterial jet may be the most relevant findingPortal venous phase identifies GI bleeding with higher sensitivity than arterial phase,
because more time is available to collect and produce greater density *Change in the appearance of the jet from arterial to portal phases confirms active bleeding,
mainly when unenhanced scan showed no hyperdense intraluminal material Extravasation shape varies depending of velocity of bleeding,
arterial or venous origin or distance between bleeding site and the collection zone on the bowel wall.
Can be linear,
circular,
spot or fold-shaped,
or form a fluid-contrast level
.Fig. 6 Fig. 7 Fig. 8 Fig. 9 Fig. 10
MDCT findings of AGIB.
Other signs.
Etiology of bleeding
Minor CT findings are usually seen in venous-portal phase,
and are useful to reinforce the diagnosis.
Include:
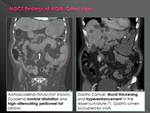
•Abnormal mural enhancement
•High-attenuating peribowel fat
•Intestinal wall thickening
•Polyp or tumor
•Vascular dilatation
•Intramural hematoma
•Focal dilatation of a full bowel segment
In presence of clinical bleeding,
CT demonstration of a potentially hemorrhagic lesion (ie.
tumor,
infection,
enlarged vessel) suggests a possible cause of bleeding.
This is not possible when the lesion is highly prevalent (eg.
diverticula),
without direct CT evidence of active bleeding
Fig. 12 Fig. 13 Fig. 14
MDCT findings of AGIB.
Pitfalls.
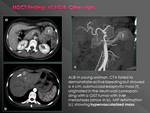
False negative
Intermittent nature of gastrointestinal bleeding.
Bleeding rate below the detectable limit.
Thin jet•when indicated,
always obtain three-phase study.
Dilution:presence of intestinal fluidnever give positive or negative oral contrast!
Many other: blood pressure,
misinterpretation,
etc.Fig. 16
MDCT findings of AGIB.
Pitfalls.
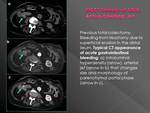
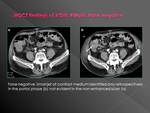
False positive
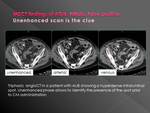
Typical context of mistake: hyperintense focus in vascular phases without having performed native phase
Presence in the bowel lumen of any hyperattenuating substance as clips,
suture or embolization material,
medication,
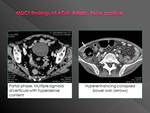
foreign bodies or rests of prior oral contrast can simulate bleedingIt is relatively common the presence of barium within a diverticulum,
which may mimic clots or even active bleeding
The presence of residual contrast material from a previous examination in the topogram or unenhanced scan may make it advisable to suspend the exploration
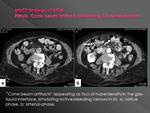
Hyperenhancing collapsed bowel wall may be another potential cause of error
Cone beam artifacts arises when there is a marked difference in attenuation between two adjacent tissues,
usually intraluminal gas and intestinal wall. They usually appear in the gas-wall interface as circumscribed linear opacities that mimic CM extravasationFig. 18 Fig. 19 Fig. 20
Main causes of AGIB.
Causes of acute massive rectal bleed located in upper GI tract.
Fig. 21
Main causes of AGIB.
Lower GI tract (ALIB).Fig. 22