This retrospective study was approved by the investigational review board,
and the requirement for informed patient consent was waived.
A search of our institution’s histopathology,
radiology,
and medical records for the period between February 2001 and October 2011 revealed 130 patients with AIP.
Patient data were included according to the following criteria: (a) clinical diagnosis of AIP based on fulfillment of Italian diagnostic criteria for AIP,
(b) histopathologically proved AIP,
(c) radiological diagnosis of focal form of PAI and (d) availability of MR examination findings.
Exclusion criteria were as follows: (a) there was a lack of available follow-up examination findings because such examinations were performed at other institutions or by using other (not MR) imaging techniques (37 patients),
and (b) the diagnosis of the diffuse form of AIP (56 patients).
Thus,
the final study population comprised 37 patients with a mean age of 51,8 years (age range,
25-78): 26 men (mean age 52,2 years; age range,
26-78 years) and 11 women (mean age 51,6 years; age range,
25-73 years) (Table 1).
All patients underwent contrast material-enhanced MR imaging with MR cholangiopancreatography at diagnosis,
after steroid treatment and during the follow-up period (median follow-up period 23,9 months; range 4,1-126,7 months).
After the diagnosis was rendered,
all patients underwent treatment with high-dose steroid: they received 1 mg per kilogram of body weight for 7-15 days,
after which the dose was tapered to 2,5-5,0 mg per week.
Steroid treatment was also administered after the first episode of recurrent AIP,
whereas after the second episode an immunosuppressive therapy was administered: 2 mg/kg azathioprine per day.
IMAGE ANALYSIS
The MR images were analyzed at a workstation by a radiologist (R.M.,
15 year experience in gastrointestinal radiology) who was aware of the diagnosis of AIP.
The MR imaging parameters were assessed with qualitative and quantitative image analysis at diagnosis,
after steroid treatment,
and at follow-up MR imaging.
The qualitative image analysis parameters assessed included:
- Presence of anatomical malformations of the pancreatic ductal system (eg pancreas divisum).
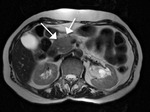
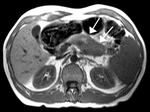
- Site (head-uncinate process or body-tail of the pancreas) of pancreatic lesions (Fig. 1,
Fig. 2).
- Signal intensity of the pancreatic parenchyma.
- Contrast enhancement of pancreatic parenchyma during the delayed phase,
as compared with the portal venous phase.
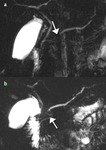
- Type of stenosis (complete Fig. 3 or thread-like Fig. 4 ) of the MPD.
- Dilation of side branches (Fig. 5).
- Presence of the “duct penetrating sign” after administration of secretin (Fig. 6).
A second radiologist,
who was not involved in the qualitative image analysis,
used an electronic caliper to perform quantitative image analysis of the following parameters at a workstation:
- Number of stenoses of the main pancreatic duct (Fig. 7).
- Length of the MPD stricture.
- Extent of upstream dilation within the lesion.
MR IMAGING
MR imaging was performed with a 1.5-T MR unit (Magnetom Symphony; Siemens,
Erlangen,
Germany) by using a four-channel phased array coil.
The patients were asked to fast for 4-6 hours before the MR examination and were given 50-150 mL of superparamagnetic iron oxide particles (ferumoxsil,
Lumirem; Guerbet,
Aulnay-sous- Bois,
France) orally just before the examination to prevent the overlap of fluid-containing organs on the MR images.
The MR imaging pulse sequences and parameters used are reported in Table 2.
Dynamic contrast-enhanced MR imag- ing involved a quadriphasic study after the injection of 0.1 mmol of a gadolinium chelate gadobenate dimeglumine (Multi- Hance; Bracco,
Milan,
Italy) or gadoterate meglumine (Dotarem,
Guerbet,
Aulnay-sous-Bois,
France) per kilogram of body weight,
administered at 2.0– 2.5 ml/sec by using a power injector (Medrad,
Pittsburgh,
Pa).
Images were obtained before the contrast material administration and during the late arterial pancreatic,
portal venous,
and delayed phases (35-45,
75-80,
and >180 seconds after contrast material administration,
respectively).