CT imaging of peritoneal carcinomatosis
Peritoneal Carcinosis is characterized by the presence of neoplastic implants with different morphological features and distribution in peritoneal cavity (6-10).
Radiologist should evaluate:
1.
Morphology
2.
Localization
Morphological aspects:
There are three board categories:
Solid implants
Cystic implants
Mixed implants

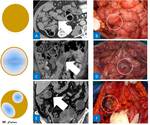
Fig. 4: Different aspects of peritoneal implants. A) Axial contrast enhanced CT scan showing solid implants (arrow) presenting as several homogenous soft tissue nodules; B) Intraoperative image of solid implants (circle). C) Coronal contrast enhanced CT image showing a cystic implant (arrow) over small bowel loops appearing hypodense due to the internal fluid component. D) Intraoperative image of cystic implants (circle).
E Axial contrast enhanced CT image showing a 4 cm implant of peritoneal carcinomatosis (arrow) presenting an ovular shape and a mixed structure consisted of a mucinous cystic component and a solid irregular rounded wall showing contrast enhancement. F Intraoperative image of mixed implants (circle).
In all types of categories calcifications can be present or not.

Fig. 5
Solid,
cystic and mixed implants can present with different patterns that depicts typical aspects of peritoneal carcinomatosis (10).
Micronodular Pattern
Micronodular pattern is characterized by the presence of tiny 1-5 mm milky spots of peritoneal implants diffusely involving the tunica serosa and subserosal fat.
Greater omentum,
lesser omentum and mesentery are typically involved.

Fig. 6: Micronodular Patter: a)and c) CT axial images showing several 4-5 mm implants involving great omentum and mesentery. b) Surgical specimen of mesentery.
Nodular Pattern
Nodular pattern is characterized by the presence of > 5 mm nodular implants diffusely involving the tunica serosa and subserosal fat .
Nodules may have an oval shape with rounded contours or a star shape appearence with spiculated margins providing a stellate pattern.

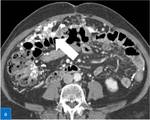
Fig. 7: a) Axial CT image showing a stellate nodule over ascending colon.
Omental cake
Omental cake consists of a diffuse nodular involvement of the greater omentum in association with fibrotic tissue.
This leadis to a consolidation of the omental fat that seems to be stratified.

Fig. 16: Omental Cake: a) CT axial image showing diffuse great omentum involvement b) Surgical specimen
Plaque like pattern
This aspect is typically found in subdiaphragmatic spaces and is due to the confluence of multiple nodular implants.
Plaques are irregular soft-tissue thickenings of inconstant extension that coat abdominal viscera and peritoneal walls presenting a lower attenuation than the parenchyma on contrast-enhanced scans.

Fig. 8: "Plaque like" implant: a) Axial contrast enhanced CT image showing a “plaque-like” implant (arrow) over hepatic surface appearing relatively hyopdense in comparison with surrounding parenchyma, due to the presence of a mucinous component.b) Surgical intervention confirms the plaque like implant (arrowhead).
Mass like pattern
Mass like pattern is typically found in pelvis and comes out from the same mechanism of 'plaque like' appearance.
In this case,
the confluence of multiple nodular implants can lead to the formation of tissue mass which can reach sizes of several centimeters.
When an individual masses are about 10 cm in diameter or larger it is called “bulky tumor”.

Fig. 9: "Mass like" implant: a) Axial contrast enhanced CT image showing a large inhomogeneous soft tissue mass (arrow) located in left iliac fossa. b) Surgical intervention confirms the bulky malignant mass.
Teca aspect
Small bowel loops appear completely enveloped by a thickened layer of visceral peritoneum that covers the bowel loops as a sleeve.
Sometimes neoplastic tissue that completely coated small bowel loops causes small bowel obstruction with consequent dilatation of proximal loops,
a condition called “ileal freezing”.

Fig. 10: Teca Aspect: a) CT coronal image b)CT axial image c) CT axial image showing small bowel loops
completely coated by a thickened visceral peritoneum. Neoplastic tissue produces small bowel
obstruction with consequent dilatation of proximal loops, a condition called "ileal freezing". d)
Surgical specimen.
Neoplastic Ascitis
Ascites may be due to increased capillary permeability and fluid production or to obstructed lymphatic vessels and decreased absorption. During inspiration fluid accumulates in sub- diaphragmatic spaces,
paracolic gutters and epiploon retrocavity. In some cases,
also in advanced stages,
there is only few ascitis or it is absent.

Fig. 11
Localization of peritoneal carcinomatosis
Radiologists must specify every sites of peritoneal carcinomatosis in order to provide a staging as detailed as possible.
The best rule to make a good report is to carefully check the surface of the bodies
covered by the peritoneal layer,
peritoneal ligaments and peritoneal spaces that surround them.
The most common sites involved by peritoneal carcinomatosis will now be considered dividing abdomen in upper-mesocolic space,
infra-mesocolic space and pelvis and considering also retropertoneal space,
subperitoneal space and subcutaneus metastases.
Uppermesocolic space:

Fig. 12
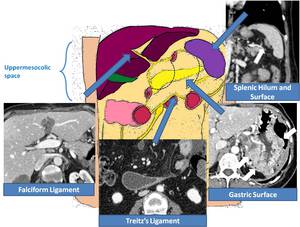
Fig. 13
Inframesocolic space:

Fig. 14

Fig. 15
Pelvis:

Fig. 17

Fig. 18
Subcutaneus tissue ("Sister Mary Joseph's Nodule") and Retroperitoneal space:

Fig. 20: A patient with pancreatic adenocarcinoma(arrowhead) presented with multiple cystic implants in subcutaneus tissue(white arrow), called siter Mary Joseph's nodule, and retroperitoneal implants (blue arrow).
Subperitoneal space:

Fig. 21: Multiple cystic implants of carcinomatosis (arrow) inside mesorectum, in a patient with rectal mucinous adenocarcinoma.
Reporting Scheme

Fig. 19