The study was conducted with the approval of institutional review board and was compliant with Health Insurance Portability and Accountability Act regulations.
Informed consent was waived by the Institutional Review Board.
In our institution,
patients with high suspicion for pancreatic adenocarcinoma are referred to for pancreatic MDCT Angiography asfirst CTstudy. This study includes 144 consecutive patients referred for pancreatic CTA for suspected pancreatic neoplasm.
These patients were assigned to either standard or split bolus spectral MDCT protocol accordingly to scanner availability.
Of those,
69 scans that were reported as normal on clinical interpretation by two radiologists in service comprised by a radiology resident and an experienced abdominal imager staff.
These studies were reviewed again by one of the investigators (ORB,
8 years of experience in abdominal imaging) who confirmed the original interpretation.
The patients were also considered as having normal pancreas by tentative clinical assessment based in part on the results of the CT scan were not include in any further analysis.
One case with split bolus pancreatic CTA was excluded due to the poor quality.
This patient was very obese (430 pounds) and a standard pancreatic CTA that was performed subsequently was also of low image quality.
The remaining 74 patients with pancreatic lesions were included in this study.
Of these,
38 had single bolus pancreatic CTA and 36 split bolus spectral imaging.
Scanning Technique
Split bolus spectral studies were performed on a 64-detector GE Discovery CT750 HD with Gemstone Spectral Imaging (General Electric Medical Systems,
Milwaukee,
WI).
Standard protocol studies were performed on a 64-detector GE VCT scanner (General Electric Medical Systems,
Milwaukee,
WI).
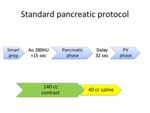
Standard protocol CT scan was obtained with filtered back projection reconstruction with non-contrast,
late arterial (pancreatic) and portal venous phases.
ASIR (Adaptive Statistical Iterative Reconstruction) of 30% was implemented to reduce the radiation dose in all phases.
The low mA non-contrast scan was performed with helical scan,
120kVp,
large SFOV,
200mA,
noise index of 26,
pitch 1.375,
collimation of 64 x 0.625 mm and reconstructed with slice thickness of 5mm and interval of 5mm. The late arterial (pancreatic) phase was scanned to include pancreas only with 120kVp,
large SFOV,
675mA,
NI (noise index) of 19,
automatic tube current modulation,
pitch 0.984,
collimation of 64 x 0.625 mm,
and reconstructed with slice thickness of 2.5mm and interval of 2.5mm.
Portal venous phase included the whole liver and was scanned with 120kVp,
large SFOV,
600mA,
NI of 13.88,
automatic tube current modulation,
pitch 1.375,
rotation of 0.5 sec,
collimation of 64 x 0.625 mm,
and reconstructed with slice thickness of 5mm and interval of 5mm.
Bolus tracking was used to ascertain the late arterial phase,
which was triggered 15 seconds after aortic enhancement reached 300HU.
The portal venous phase was scanned 32 seconds after pancreatic phase or 75 seconds after initiation of contrast injection,
whichever occurs earlier.
Total of 140cc of contrast was injected at a rate of 4-5 cc/sec,
followed by 40cc of saline chaser.
Split bolus spectral CT scan was performed first with a low-mA non-contrast scan of the abdomen with 120kVp,
large SFOV,
200mA,
NI of 26,
automatic tube current modulation,
ASIR of 30%,
pitch 1.375,
collimation of 64 x 0.625mm and reconstructed with slice thickness of 5mm and interval of 5mm.
This was followed by a single helical GSI-10 scan,
performed with gemstone spectral acquisition (GSI),
140kVp,
600mA,
automatic tube current modulation,
pitch of 1.375,
rotation of 0.8 sec,
collimation of 64 x 0.625mm.
The spectral images were then reconstructed at 60keV and at 77kev; both with 2.5 mm slice width and interval.
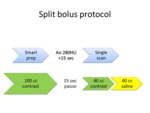
The split bolus protocol included two contrast injections separated by a short pause geared to provide a combined arterial-venous phase.
First 100 cc of contrast was injected for the portal venous phase at approximately 70 sec and second 40 cc of contrast to boost the pancreatic phase at approximately 35 sec after the second injection.
Empirically,
with an injection rate of 5 cc/sec,
the first dose of 100 cc lasts 20 sec; after a pause of 15 sec,
a second dose of 40 cc lasts 8 sec and scan is done 35 sec after the second bolus (pancreatic phase) or 70 sec after the first bolus (portal venous phase).
At the injection rate of 4 cc/sec the pause is set at 10 sec.
The second bolus is followed by 40 cc of saline chaser.
Based on these empirical delays,
we used bolus tracking set after the initiation of the second bolus and set to start scanning 15 sec after the aorta reached 280HU.
For both studies we used Omnipaque 350,
(Iohexol,
350 mg/mL,
GE Healthcare) with 4-5cc/sec injection rate into the antecubital fossa vein.